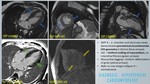
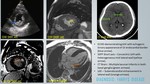
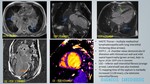
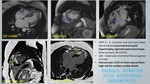
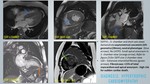
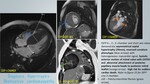
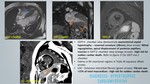
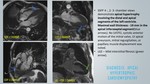
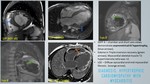
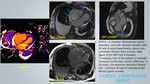
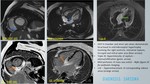
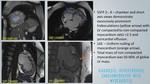
A total of 400 MRI cardiac scans of patients with clinical presentation of LVH were retrospectively reviewed for MR characteristics with clinical and laboratory parameters correlation.
The following cases were observed:
- Pressure overload: Hypertension,
subvalvular aortic membrane,
aortic valvular stenosis,
supravalvular aortic stenosis,
coarctation of aorta.
- Volume overload: Valvular regurgitation.
- Infiltrative cardiomyopathies: Amyloidosis,
Anderson-Fabry disease,
Sarcoidosis.
- Non-infiltrative cardiomyopathy: HCM.
- Inflammatory cardiomyopathy: Myocarditis,
Endomyocardial fibrosis.
- Neoplasm.
- Unclassified cardiomyopathy: Left ventricular non-compaction.
Findings:
A. PRESSURE OVERLOAD:
1. HYPERTENSION:
The most common cause for LVH with a prevalence of 36–41%.
An increased LVM is strongly linked to an increased risk of cardiovascular events [5].
CARDIAC MRI FINDINGS:
Functional assessment:
• Diastolic dysfunction.
•Symmetric/concentric LVH (<15mm) geometry always less when compared to HCM.
• More substantial hypertrophy (> 16 mm) fall into a gray zone – to differentiate HTN from HCM as a cause,
clinical evaluation after antihypertensive treatment help to define the correct diagnosis [6] - figure 8,
9.
• Normal wall motion.
Midwall circumferential strain by CMR tagging is depressed [7].
Structural assessment:
• Rest-stress perfusion: Inducible ischemic in chronic hypertensives secondary to microvascular obstruction.
• Late gadolinium enhancement (LGE): Diffuse (poorly evaluable as LGE is dependent on T1 mapping) or Focal mid-myocardial fibrosis (45%) typically in the basal septum [8].
The criteria for prognostic stratification:
- Presence of diastolic dysfunction,
- Concentric LVH,
- Inducible ischemia,
- Diffuse or focal mid-myocardial fibrosis.
2. LEFT VENTRICLE OUTFLOW TRACT OBSTRUCTION – AORTIC STENOSIS and VOLUME OVERLOAD - AORTIC REGURGITATION:
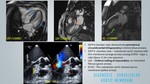
a) SUBVALVULAR AORTIC MEMBRANE - figure 10,11:
- Subvalvular aortic stenosis is not so uncommon,
estimated 6.5% prevalence and 14% of left ventricle out flow tract obstruction (LVOTO) in literature [9].
- Associations: ASD,
VSD OR ASVD.
- Three types:
- Discrete: Thin,
crescent-shaped membrane,
commonest.
- Thick fibromuscular ridge.
- Tubular.
b) AORTIC VALVULAR STENOSIS - figure 12,13:
- Most common cause of LVOTO.
- Most common cause for aortic stenosis (AS) is calcified valve in elderly and bicuspid in young population.
- Bicuspid aortic valve is the most common cause for aortic valve replacement(AVR) as it is more prone for aortic aneurysm,
endocarditis and dissection.
- Most common acquired cause in developing countries is rheumatic heart disease(RHD).
- Patients with AS progresses slowly to compensatory LVH,
fibrosis and heart failure.
c) SUPRAVALVULAR AORTIC STENOSIS - figure 14,15:
Causes:
- Congenital: isolated or Syndromic (William syndrome)
- Acquired: Iatrogenic.
Types:
- Thick fibrous ring above the aortic valve with hourglass appearance,
- Thin fibrous membrane.
- Diffuse narrowing.
d) COARCTATION OF AORTA - figure 12:
- Common congenital heart disease accounting for approximately 6–8% [10].
- Location types: Preductal/infantile,
juxtaductal or postductal.
- Commonest collaterals to develop are internal mammary,
intercostal arteries,
and thyrocervical trunks.
- Associations: Bicuspid aortic valve (most common).
VSD,
ASD,
pulmonary artery stenosis.
e) AORTIC REGURGITATION - figure 15:
- Aortic insufficiency leading to retrograde flow during diastole and increase in volume overload.
- Causes: Dysfunction of leaflets or aortic root/ascending aorta dilatation or inflammation.
- Most common cause in developing countries is rheumatic heart disease.
CARDIAC MRI FINDINGS:
Functional assessment:
- Identification of membrane/aortic valvular / supravalvular stenosis/coarctation of aorta.
- Concentric LVH geometry.
- Phase contrast imaging: Quantification of gradient - Depending on the gradient across obstruction - Diastolic to systolic dysfunction.
- Aortic valvular regurgitation quantification (regurgitant volume and fraction),
- Aortic stenosis quantification (valve area and mean gradient) – increasing the risk of endocarditis [11],
help in transcutaneous AVR planning.
Structural assessment:
- Late gadolinium enhancement: Focal mid-myocardial and RV insertional fibrosis (25% of cases) if wall thickness >18mm.
- MRA: To assess coarctation of aorta and associated findings.
The criteria for prognostic stratification:
- Concentric LVH >20mm.
- Female sex,
Age > 30years in subvalvular aortic stenosis.
- High gradient Degree LVOTO ≥80 mmHg
- Turbulent flow produced by the membrane.
- Severe aortic regurgitation (regurgitation fraction >50%)/stenosis (stenotic area <1cm2 and mean gradient >40mmHg).
- Extent of LGE correlate with clinical evolution after aortic valve replacement [12].
B. INFILTRATIVE CARDIOMYOPATHIES
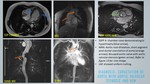
1. AMYLOIDOSIS - figure 16:
Amyloidosis is a heterogeneous disease in which there is accumulation of insoluble fibrillar proteinaceous material in myocardial interstitium predominantly in subendocardial layer leading to fibrosis.
Four types of amyloidosis: Primary AL amyloidosis (multiple myeloma),
Secondary AA amyloidosis (infection or inflammatory disorders),
Senile amyloidosis,
hereditary amyloidosis.
CMR assessment and prognostic stratification [13]:
- Diffuse LVH with decrease in signal intensity on T1-weighted images.
- Reversed blood pool to myocardium relationship - myocardium reaches null point before blood pool - figure 17.
- Thickening (> 6 mm) of the interatrial septum and posterior right atrial wall.
- Marked thickening of the LV wall is associated with a survival time of less than 6 months.
- Diffuse or focal subendocardial LGE.
- Pericardial and pleural effusion.
- CMR vs endomyocardial biopsy: Good sensitivity (80%) and high specificity (94%) [14].
2. ANDERSON-FABRY DISEASE:
X linked recessive lysosomal storage disorder due to beta-Galactosidase A enzyme deficiency.
Myocardial accumulation of glycosphingolipids leads to LVH which results in arrhythmias and heart failure.
CMR assessment and prognostic stratification - figure 18:
- Concentric LVH to dilated cardiomyopathy in severe cases.
- Mid myocardial LGE in the basal inferolateral segment – indicates poor response to enzyme replacement therapy [15].
- Medical renal disease and deep gray matter ischemic strokes are supporting evidence.
3. SARCOIDOSIS:
A multisystem granulomatous disease of unknown etiology.
In cardiac sarcoid,
there is myocardial inflammation with scarring.
Cardiac involvement is a major prognostic factor.
CMR assessment and prognostic stratification [16] - figure 19,
20:
- LV dysfunction.
- Inflammatory phase: Myocardial edema on IR sequence,
improves after steroid therapy.
- Fibrotic phase: Patchy mid wall,
subepicardial LGE in basal septum and lateral wall - higher rate of adverse events,
including cardiac death,
during a 21-month follow-up,
also guide for biopsy.
- Pericardial thickening/effusion.
- Pulmonary sarcoid and enlarged hilar lymph nodes.
C. NON-INFILTRATIVE CARDIOMYOPATHY:
HYPERTROPHIC CARDIOMYOPATHY:
HCM is an inherited cardiac disorder manifesting as segmental or diffuse LVH with a non-dilated hyperdynamic LV,
in the absence of cardiac or systemic disease.
It is the leading cause of sudden death in infants and young adults.
It has an estimated prevalence of 0.3-0.5% [17].
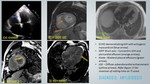
Cardiac MRI assessment - figure 21- 28:
- Asymmetric LVH: Five phenotypic forms: Reverse curvature septum,
Sigmoid septum,
Neutral septum,
Apical,
Mid-ventricular.
- Systolic anterior motion of the mitral valve with LVOTO,
mitral regurgitation.
- LV apical aneurysm.
- Abnormal thickening or attachments of papillary muscles,
abnormal chordal attachments from the posteromedial papillary muscle to the anteroseptum/septum.
- Patchy mid-wall LGE enhancement (up to 75%) in hypertrophied septal segments
- Screening of family members.
The criteria for prognostic stratification of HCM include:
- LV wall thickness - >30mm is an independent risk factor for sudden death,
- LVOTO with depressed ejection fraction (burned-out phase),
- Presence of fibrosis of >15% of total myocardial mass is associated with sudden cardiac death and warrants for primary prevention implantable cardioverter defibrillator therapy.
C. INFLAMMATORY CARDIOMYOPATHY:
1. MYOCARDITIS:
Myocarditis refers to inflammation of myocardium.
The most common etiology is viral infection.
There is direct cardiomyocyte injury leading to elevated troponin levels followed by edema,
necrosis and contractile dysfunction.
Cardiac MRI assessment and prognostic stratification:
- Lake Louise Criteria: high specificity and positive predictive value :- T2 myocardium to skeletal muscle ratio >1.9,
early gadolinium enhancement ratio between myocardium and skeletal muscle >4,
delayed enhancement in subepicardial and or mid-myocardium [18] - figure 29.
- T2-STIR assesses myocardial edema and early gadolinium enhancement assesses inflammatory hyperaemia and necrosis.
The presence of necrosis is associated with higher cardiovascular mortality.
2. ENDOMYOCARDIAL FIBROSIS:
Aka Loeffler’s hypereosinophilic endocarditis is restrictive cardiomyopathy due to increased eosinophil count and serotonin secretion which causing damage and necrosis of the endocardium.
CMR assessment and prognostic stratification [19] - figure 30,31:
- Restrictive cardiomyopathy - small ventricles,
diastolic dysfunction,
biatrial dilatation.
- Focal LVH,
predominantly in apex.
- Diffuse or focal edema and subendocardial LGE.
- Thrombi formation.
E. NEOPLASM:
Gamuts:
Metastases are the most common cardiac malignancy.
Most common primary tumor is sarcoma and benign tumor is myxoma.
Right sided tumors are more commonly malignant and left sided tumors are more commonly benign.
CMR assessment and prognostic stratification [20]:
- Location,
size,
infiltration,
presence of pleural/pericardial effusions.
- Contrast enhancement characteristics.
Differentiation from thrombus.
- Descriptors of malignancy: Large size (>5cm),
multiplicity,
ill-defined,
invasion,
pericardial and pleural involvement,
Triple IR hyperintensity,
early and late gadolinium enhancement - figure 32,33.
E. UNCLASSIFIED CARDIOMYOPATHY:
LV NON-COMPACTION:
LVNC or spongy myocardium is a rare autosomal dominant disease characterized by the presence of non-compacted myocardial layer.
Alteration in myocardial structure leading to thromboembolism and arrhythmias.
CMR assessment and prognostic stratification [21]:
- Prominent trabeculation and deep intertrabecular recesses in the mid to distal anterior,
lateral and apical segments.
- Non-compacted to compacted (NC/C) ratio of > 2.3 in diastole is pathognomonic,
with a high degree of sensitivity (100%),
specificity (93%) compared to echocardiogram - figure 34.
- Noncompacted myocardial mass (defined at end-diastole) greater than 20-25% of the global LV mass,
noncompacted mass greater than 15 g/m2.
- Subendocardial hyperenhancement corresponding to fibrosis.
- Thrombi formation.