The technique of a routine US elbow examination must be arranged with patient seated and with the elbow placed over examination table.
US diagnostic equipment should be used with linear-array.
It should be remembered that during ultrasonographic evaluation,
transducer management needs maximum stability over the studied area,
because the curvilinear contours of the elbow joint could result in anisotropy and pathological findings may be subtle.
To avoid anisotropy,
transducer must be placed along the long the axis of tendons or ligaments.
Position 1.
Lateral compartment.
Key structures to be evaluated in this compartment are: radiocapitellar joint,
common extensor tendon (CET) and lateral collateral ligamentous complex.
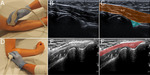
With elbow in extension and supination and in the sagittal axis,
the articulation of radial head with the capitellum.
By displacing the transducer laterally,
the CET,
usually echogenic and fibrillar,
superficial to the bone plane,
in which it is inserted,
is identified.
It is important to evaluate its thickness,
echogenicity and the bone surface of insertion.
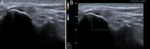
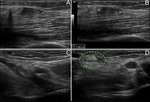
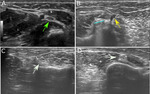
The findings observed in the sagittal plane are tried to confirm in the transverse plane.
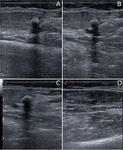
With elbow in 90° flexion,
the CET appears echogenic and attached to the bony structures (figure 1).
Lateral collateral ligamentous complex,
composed by right collateral ligament (RCL),
annular ligament (AL),
and lateral ulnar collateral ligament (LUCL),
It is evaluated with the extended and proned elbow.
LUCL appears as a thin and echogenic structure,
deep to CET that merges distally with AL.
RCL originates in the lower lateral epicondyle and inserts over the radius where it fuses with AL fibers.
Position 2.
Anterior compartment.
Key structures to be evaluated in this compartment are: anterior joint recess,
distal tendon of the biceps,
brachialis muscle,
biceps brachii muscle,
median and radial nerves.
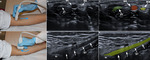
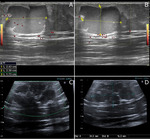
The anterior joint recess must be evaluated in the sagittal and transverse planes.
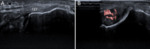
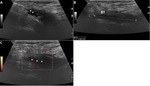
The coronoid fossa is studied in the sagittal plane and is identified as a concavity on the anterior surface of the humerus,
filled by the anterior fat pad (figure 2).
Under normal conditions a small amount of liquid can be seen.
With the elbow in extension and supination we approach axially to locate the distal tendon of the biceps over the brachialis muscle.
The distal tendon of the biceps has a length of 7 cm.
For its easier identification we initially locate proximal to the elbow joint.
Once the tendon is identified,
we follow it until it is inserted into the radial tuberosity.
The transverse plane allows to get an idea of the obliquity of the tendon.
Once its radial insertion is found,
the transducer is turned trying to imitate this obliquity until it represents the tendon on its long axis.
The ulnar insertion of the brachialis is identified in the sagittal and transverse planes as it is more muscular than the biceps tendon.
The median nerve descends with the vasculo-nervous humeral bundle,
passes beneath the aponeurotic expansion of the distal biceps between the two heads of pronator teres and identifies it medially to the biceps tendon together with the brachial artery (figure 2).
The main trunk of radial nerve can be identified in the transverse plane in the anterolateral elbow.
We must follow it distally until its bifurcation in the sensitive branch and posterior interosseous nerve.
Subsequently we follow the posterior interosseous nerve in the transverse plane in its path between the superficial and deep portion of the supinator muscle.
The biceps and brachialis muscles are superficially assessed in images proximal to the supracondylar region.
Transverse study should be performed from 5 cm proximal to 5 cm distal to the trochleo-ulnar joint.
Position 3.
Medial compartment
Key structures to be evaluated in this compartment are: common flexor tendon (CFT) and medial collateral ligament (MCL)
It is evaluated with the arm in extension and in maximum supination.
As an alternative the patient in supine with the arm in abduction and external rotation and the forearm in flexion of 90 degrees.
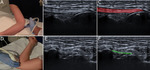
It begins in the sagittal plane identifying the CFT,
shorter and thicker than CET,
in the medial epicondyle.
We value the MCL deep to CFT.
It provides the greatest resistance to valgus stress.
It has three beams (anterior,
posterior and transversal) of which the former is the largest and most important and the one we value.
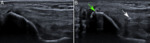
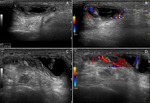
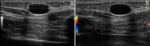
Deep to the posterior part of CFT a sagittal image of the ulnar nerve can be obtained below the muscles of the carpal ulnar flexor.
The study is completed with transverse images of the structures (figure 3).
Position 4.
Posterior compartment
Key structures to be evaluated in this compartment are: distal triceps muscle and tendon,
posterior joint recess,
olecranon bursa,
and ulnar nerve.
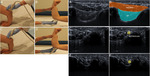
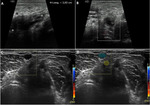
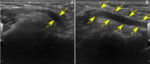
It is explored with the elbow in flexion of 90 degrees,
in maximum pronation with the palm of the hand resting on the table ("crab" position) (figure 4).
The triceps (hypoechoic) and distal triceps tendon (TT) (hyperechoic) muscles should be evaluated in the sagittal and transverse planes until their insertion into the olecranon.
We must evaluate the olecranon fossa,
deep to the triceps,
occupied by a posterior echogenic fat pad.
The dynamic assessment of the ulnar nerve should be performed,
evaluating it in the ulnar canal.
First,
we assess the nerve during the extension,
positioning the probe at one end in the medial epicondyle and in the other in the olecranon.
Later we evaluated the nerve with the flexion of the arm,
keeping one end of the probe in the medial epicondyle.
The ulnar nerve under normal conditions is located posterior to the apex of the medial epicondyle in extension and in flexion.
The diagnosis of ulnar nerve dislocation is made when the nerve during flexion is located in front of the medial epicondyle.
The dislocation of the ulnar nerve can cause nervous irritation due to friction of the nerve when passing in front of the medial epicondyle.
Pathology
Tendinopathies
Echographic findings are similar: hypoechoic areas due to loss of the fibrillar pattern and hyperechoic areas due to calcification and/or fibrosis.
Hypoechoic or anechoic clefts represent areas of fibrillar rupture.
The tendon may be thickened and there may be signs of enthesopathy,
which is manifested by cortical bone irregularity and small calcifications.
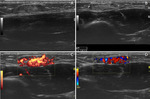
In severe cases,
the Doppler study may show an increased flow in the affected tendons (figures 5,
6,
7).
Tendinous rupture
Biceps
The tendon rupture of the biceps usually occurs due to disinsertion at the level of the radial tuberosity,
although more proximal intratendinous lesions also occur.
In case of complete rupture,
fibrillar pattern of the tendon is not identified,
which is replaced by echogenic or hypoechoic areas that represent hematic or fluid collections in the tendon bed.
The thickened and retracted proximal fibers can be identified proximally.
Tendon rupture is usually associated with a lacertus fibrosus lesion in most cases.
This is identified as a thin echogenic band on the pronator teres.
In case of injury it is thickened,
with heterogeneous and poorly defined echogenicity (figures 8,
9).
In partial ruptures there may be thickening or focal thinning of tendon,
as well as irregularity of the contour,
depending on time of evolution of the rupture.
Triceps
The avulsion of TT due to osseous stripping in the olecranon is more frequent than intratendinous rupture.
Ultrasonography can demonstrate the ascending bone fragment and alterations of the contour of tendon with echogenic or hypoechoic areas surrounding it,
which correspond to the presence of accompanying hematoma.
Inflammatory and degenerative pathology
Bursitis
The causes of bursitis are mainly mechanical,
but it can also be secondary to other factors.
The echogenic content of bursas suggests a hemorrhagic,
inflammatory or septic nature.
Ulnar bursa is located between the tendon of distal biceps and the radial tuberosity.
The echographic appearance of bursitis is an hypoechoic or anechoic mass,
although it may have septa and a thick wall due to inflammatory changes.
When it is relaxed,
it can completely surround the tendon of the biceps simulating tenosynovitis (figure 10).
Olecranon bursitis manifests clinically as a subcutaneous mass in the olecranon area and,
therefore,
is easy to diagnose on clinical examination.
Ultrasound can evaluate both its content and thickness of the wall (figure 11).
Neuropathies
Neuropathies are usually secondary to entrapment or compression of the nerve in a static or dynamic way,
usually in osteofibrous or fibromuscular tunnels.
Noncompressive neuropathies include traumatic nerve injuries,
inflammatory pathology and tumors of the nerve itself.
Ulnar nerve neuropathy occurs mainly at the level of the cubital tunnel of the elbow,
usually on the posterior aspect of the epitrochlea and on the border of the arcuate ligament.
Among the causes that can produce it include the bone spurs in the epitrochlear fossa,
soft tissue masses,
thickening of the lateral ulnar collateral ligament and the accessory anconeus epitrochelearis muscle (figure 12).
The compressive neuropathy of the radial nerve usually occurs when the nerve enters the supinator muscle,
under the Fröhse arch.
It is known as supinator syndrome.
Radial neuropathies secondary to fractures of the humerus or inflammatory cause can be observed,
affecting the radial nerve on its course around the humerus (figure 13).
Tumoral and pseudotumoral pathology
Any bone or soft tissue tumor,
both benign and malignant,
can affect the elbow (figures 14-18).
One of the main causes of mass at the elbow is the increase in size of epitrochlear adenopathies,
usually secondary to inflammatory pathology.
The ultrasound shows the typical appearance of a lymph node with hypoechoic cortical and echogenic hilum.