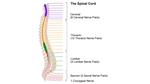
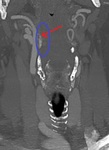
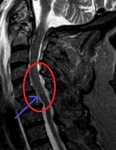
Anatomy:
The cervical spine primarily functions to position the head while maintaining stability of the spinal cord. The thoracolumbar spine is the primary load-bearing structure of the axial skeleton.
Both sections of the spine are subject to multiple tangential forces,
which act around a fulcrum described as the instantaneous axis of rotation (IAR),
located in the posterior third of the vertebral body. Depending on the direction of the force vector acting on the IAR,
characteristic injury patterns such as the ones described below will result.
The patterns of injury,
if not initally recognized,
can lead to devastating neurologic consequences.
Thus,
it is essential for the radiologist to carefully search for the subtle sequelae associated with these injury patterns.
Imaging:
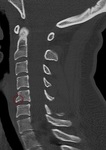
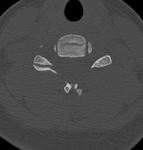
CT: Depending on the clinical context and presentation of the patient,
a CT of the spine (cervical,
thoracolumbar,
sacral) will be performed first to characterize the anatomy,
extent,
and morphologic pattern of the injury.
This is almost always the first imaging modality employed in the emergent setting after the inciting trauma.
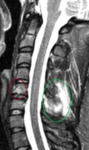
MRI: An MRI is performed in the acute setting if there are acute neurologic deficits associated with the traumatic injury to help characterize the extent of ligamentous injury and involvement of the spinal cord,
nerve roots,
and epidural hematoma.
An MRI can also be helpful in characterizing the recency of vertebral column injuries and can guide the clinician in potential surgical planning.
Types of Fractures:
Teardrop Fractures:
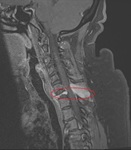
Flexion Teardrop Fractures are fractures of the anteroinferior aspect of a cervical vertebral body due to flexion of the spine along with vertical axial compression.
Severe flexion and compression forces (e.g.
deceleration during a motor vehicle collision,
"diving impact" type injury) combine to produce this characteristic pattern of injury.
Most characteristic findings will include a "teardrop" sign represented by a triangular fragment of the anteroinferior lip of the vertebral body with posterior displacement of the posterior vertebral body relative to the intact inferior cervical column.
Flexion teardrop fractures are usually unstable and will almost alway require open reduction/internal fixation as translocation of the unstable posterior vertebral body with the potential for spinal cord compression resulting in paralysis.
Extension teardrop fractures are fractures caused by forced extension of the neck with resultant avulsion of the anteroinferior corner of the vertebral body.
The extension mechanism will result in disruption of the anterior longitudinal ligament,
hence the fracture will be stable in flexion,
unstable in extension.
This injury pattern will usually occur at C2,
and portends more conservative management than a flexion teardrop fracture as the vertebrae below the site of injury are not at risk of causing spinal cord impingmenet.
In helping differentiate between a flexion teardrop fracture and an extension teardrop fracture,
both CT and MRI of the spine are performed to help characterize these fracture patterns: a CT is usually performed first in an emergent setting to help identify the anatomy and location of the fracture,
while an MRI helps to better delineate the extent of ligamentous and paravertebral soft tissue injury,
and involvent of the associated spinal nerve roots.
The MRI will help between a flexion teardrop fracture and an extension teardrop fracture: whereas an extension teardrop fracture will involve only the anterior longitudinal ligament,
a flexion teardrop fracture will involve the ligamentum flavum and the posterior longitudinal ligament,
hence explaining its inherent instability.
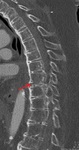
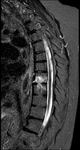
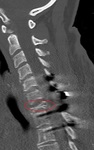
Burst Fracture: are fractures of the vertebral body related to high-energy axial loading spinal trauma resulting in disruption of the posterior vertebral body cortex and resultant retropulsion into the spinal canal.
This can present in many different ways,
but the general principle is the same: an inciting trauma will result in axial loading which will drive the vertebral body downwards onto the vertebral disc.
Posterior retropulsion of the vertebral body into the spinal canal can result in cord compression.
CT of the spine is performed to help characterize the acuity of the fracture in the emergent setting.
An MRI will help to better delineate the extent of the fracture deformity,
ligamentous injury,
and involvement of the spinal cord.
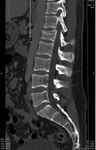
Wedge Compression Fracture: is a hyperflexion type fracture that results from axial loading.
Most of these will typically affect the anterior column of the vertebral body,
hence the term anterior wedge compression fracture.
These fractures are typically seen in the setting of insufficiency,
secondary to osteoporosis or neoplasm.
A small percentage of these will be secondary to trauma.
A CT of the spine is typically performed first to help characterize the acuity of the fracture in the emergent setting,
with an MRI helping to better delineate the extent of fracture deformity and ligamentous injury.
These injuries are typically less serious than the burst fracture,
as an anterior wedge compression fracture in isolation will not result in spinal cord compression.
Long-term complications if not recognized in the emergent setting can include loss of disc height and resultant degenerative changes involving adjacent vertebral bodies.
Transverse Process Fractures: are a common sequela of trauma which most commonly affect the lumbosacral vertebrae.
These fractures are stable fractures,
but will help point the radiologist in the direction of evaluating for further traumatic injury as there exists a high association between these entities.
Cervical spinous process fractures have a high association with blunt cerebrovascular injury (BCVI) and will necessitate the need for a CTA head and neck,
whereas lumbar spinous process fractures have a high association with abdominal organ injuries and will necessitate the need for a CT abdomen/pelvis.
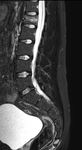
Chance Fracture: is a special type of hyperflexion/distraction fracture that results from axial loading and resultant tri-columnar collapse of the vertebral body.
These fractures are usually seen in the setting of "seat-belt" type injuries and sudden deceleration,
where the most shared history is a back-seat passanger with a seat-belt at the time of the motor vehicle collision.
If unrecognized in the emergent setting,
this injury can cause progressive kyphosis with resultant pain and deformity of the vertebral column.
These fractures are also highly associated with visceral organ injury,
including splenic rupture,
bowel perforation,
and tear of the mesentery being the most common organs injured.
A CT scan of the spine is the first imaging examination performed,
with an MRI of the spine helping delineate the extent of ligamentous injury.
In all cases with a suspected Chance fracture,
a CT of the thorax/abdomen/pelvis must be performed to help delineate any organ injury given its high association.
Treatment will usually depend on the clinical setting.
As these fractures are unstable fractures of the vertebral column,
posterior spinal fusion will eventually be performed after any emergent,
life-threatening injuries are treated.
Insufficency Fracture: are fractures that can occur in the setting of diffuse osseous dimineralization with or without a history of minor trauma.
These fractures of the vertebral column can be seen in the setting of osteoporosis,
previous traumatic injury to the vertebral body with new trauma,
and malignancy.
A CT is usually the first imaging test performed,
with an MRI being especially helpful in characterizing malignancy if suspected as a cause.
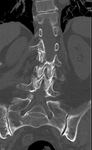
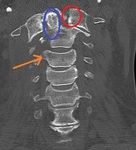
Jefferson Fracture: is a burst fracture of the C1 vertebral body.
This is a special axial-loading type of injury where the head is usually involved in a hyperflexion type of trauma where the occipital condyles are driven into the lateral masses of the C1 vertebral body.
A typical mechanism is a diving type injury.
These fractures are highly associated with other inciting trauma,
namely,
C-spine injuries (especially a C2 fracture),
a concurrent head injury (e.g.
depressed calvarial fracture,
subarachnoid hemorrhage),
vertebral artery injuries (blunt cerebrovascular injury),
and cranial nerve injury.
A CT scan of the C-spine will almost always be diagnostic of this entity.
Importance of recognizing this pattern of injury will help drive the patient care.
A CTA of the head and neck will almost always be performed in this setting to help delineate the extent of BCVI.
An MRI of the cervical spine can help delineate ligamentous injury and associated sequelae of this injury pattern,
but will be less useful in evaluating the fracture deformity.
Treatment of a Jefferson fracture is usually conservative unless ligamentous injury or epidural hematoma is diagnosed on MRI,
in which case,
more aggressive treatment will be employed. Treatment will be employed in these cases to prevent listhesis of the vertebral columns below the fractured C1 vertebral body.