Keywords:
Genital / Reproductive system female, Interventional vascular, MR, Embolisation, Treatment effects, Neoplasia
Authors:
E. Y. Auyoung, L. Ratnam, R. Das, S. M. Ameli, L. Mailli; London/UK
DOI:
10.26044/ecr2019/C-3533
Methods and materials
Patient selection: A retrospective study identified consecutive non-randomised patients (mean age: 45 years; age range: 30-60) who referred for UAE for symptomatic fibroids at one centre,
in one year.
As per recommended UAE standard protocol,
all patients were required to have underwent a pre-procedural MRI and a post-procedural MRI,
six months after embolization.
Patients without these images were excluded from the study and thus a total study group of 64 women were identified.
Data acquisition: All MRI scans were performed using a 1.5 Tesla (T) system according to identical protocols: axial T1 fast spin echo (FSE); sagittal and axial T2 FSE and axial T1 fat saturated post-contrast sequences.
Slice thickness of 5 mm was used with variable fields of view.
Contrast-enhanced sequences were acquired after intravenous injection of 20 mL gadolinium–DOTA.
Fluoroscopic-triggered MRA was performed at the region of interest at the abdominal aorta with triggering of image acquisition occurring at approximately 25 seconds.
Maximum-intensity projections of the abdomen and pelvis to the level of the renal arteries were reconstructed.
The embolization procedure was performed by certified interventional radiologists in our institution via a bilateral transfemoral approach under local anaesthesia with selective catheterisation of uterine arteries with 4F RIM catheters.
Two types of embolic agents were used: non-spherical PVA (n = 16) 350–500 μm and Microspheres (n = 48) 700-900μm. In both groups,
if greater than four vials were used,
the size of particles used were increased.
Embolization was achieved with angiographic stasis of contrast within the transverse segments of the uterine arteries for approximately 10 cardiac beats.
Data review: All images were independently reviewed retrospectively by two experienced radiologists with subsequent consensus review.
On both pre-procedural and post-procedural images,
the three-dimensional maximal measurements of the uterus and dominant fibroids were obtained using axial and sagittal T2-weighted MR images and the volume calculated.
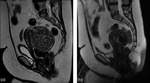
In each dominant intramural fibroid identified,
additional measurements were obtained to record the shortest distance between (a) the fibroid and the endometrial wall,
and (b) the fibroid and the serosal wall - as seen in Figure 1.
After obtaining preliminary results suggesting potential parameters to predict migration of intramural fibroids,
we tested our findings against the non-dominant intramural fibroids in all our cases to assess the reproducibility of our results.
Statistical analysis: Paired sample t-tests were performed to assess pre- and post-embolization variations in the dominant intramural fibroid’s volume and maximal diameter.
A two-sample T-test was used to analyse parameters between migrated and non-migrated dominant intramural fibroids.
Statistical significance was set to a p-value of 0.05.
Statistical power was not tested.