Keywords:
Thorax, Lung, CT, Image manipulation / Reconstruction, Computer Applications-General, Radiation safety, Artifacts, Dosimetric comparison
Authors:
S. Carey1, S. Kandel1, J. Kavanagh2, T. Chung1, C. Farrell1, P. Rogalla1; 1Toronto, ON/CA, 2Toronto/CA
DOI:
10.26044/ecr2019/C-3543
Methods and materials
Projection Algorithm:
Similar to Maximum Intensity Projection (MIP),
we create a thick-slab projection from thin-slice data by computing the Hounsfield Unit (HU) value at a given position (i,
j,
k) from the HU values of the voxels at positions (i,j,k),
(i,j,k+1) ...
(i,j,k+r),
where ris the number of voxels satisfying: l = r*w,
l is the desired output slice thickness and wis the width of one voxel in the thin-slice data.
For MIP,
the resultant CT number is the maximum CT number of the pertinent voxels.
For our algorithm,
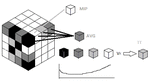
we order the voxels by increasing CT number and apply a weight function to that ordered vector (Fig 1,
2),
essentially creating a weighted average.
Similar to a MIP function,
the highest valued voxels receive the highest weight,
producing an image with sharper contrast than by using an average projection.
Unlike MIP,
none of the CT number information is discarded,
providing a higher resilience to voxel noise.
For further details about the weight function,
see[5].
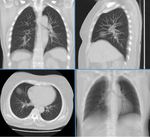
An example of a thoracic tomogram is shown in Fig.
3.
Study Methodology:
To evaluate the thoracic tomagram we prepared a dataset of 22 cases of patients who had undergone a CXR and a same day standard-of-care non-contrast CT of the chest (with mean DLP 44.1).
Scanner specific noise was added to the raw projection data to simulate the target dose of 0.18mSV.
Coronal and sagittal isotropic images were reformatted from axial reconstructions with a slice thickness of 0.8mm.
The projection algorithm was then applied to produce 2cm thick slabs with a 1cm overlap.
The x-rays and thoracic tomograms for the 22 cases were ordered randomly,
producing a sequence of 44 images.
These cases were then reviewed by three chest radiologists with no prior training for the study.
They recorded,
on a scale from -4 (definitely absent/normal) to +4 (definitely present/abnormal) their impression with respect to 13 diagnostic categories (Fig 4).
The ground truth,
collected from the original CT reports,
was compared to the reader’s response for the x-ray and thoracic tomogram for each category.
ROC curves were generated for each category.
The time for interpretation and reader’s image satisfaction score (from 1 to 10) were also recorded and statistically compared.