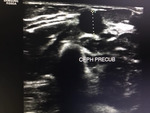
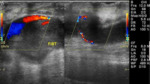
Pre-operative assessment:
Preoperative duplex ultrasound is useful in identification of vessel anatomical location,
patency and diameter.
It helps in the prognostic assessment of the vessels in terms of their ability to dilate and remodeling.
Several international guidelines on vascular access creation recommend using duplex ultrasonography to assess the possible AVF configurations pre-operatively.
Knowledge of the vascular dimensions would benefit clinical decision making regarding the AVF configuration.
From a haemodynamic point of view,
the smaller the diameters of the vessel the higher the blood flow resistance is.
Accordingly,
clinical guidelines on AVF creation now recommend minimum arterial and venous luminal diameters for forearm (>2.0 mm) and upper arm (>3.0 mm) arteriovenous fistulas.
Complete scanning of the veins of the upper limb is done by measuring the diameters at multiple discrete locations,
as well as measuring the arterial diameters and exclusion of any stenosis For a proper AVF reconstruction,
certain requirements should be met,
including a luminal diameter of 2.5mm or greater at the anastomosis point,
absence of obstruction,continuation with proximal central veins,
presence of a straight segment for cannulation and to be within 1 cm of the skin surface .
One of the most important predictive factors for radio-cephalic AVF success is measuring the venous distensibility with absolute diameter increase above 0.4 mm after 2-minute tourniquet placement.
Postoperative Assessment:
The primary imaging modality for arteriovenous fistulas(AVF) assessment is also the ultrasound,
although digital subtraction angiography as the gold standard tool may be needed in some cases with the previlage of therapeutic intervention ability.
Imaging is used mainly to:
● Confirm AVF maturation mainly by the assessment of flow velocity and fistula diameter.
● Assess early and late complications as swelling due to extravasation ,
haematoma or infection ,stenosis of the vascular access vessels,
thrombosis and steal syndrome.
Systenic assessment approach
·Minimal pressure should be applied by the transducer in order to minimize deformity of the vein and false measurements of the vein diameter.
·Each vascular structures are assessed longitudinally and transversely.
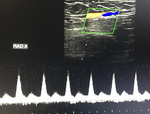
·Arterial assessment starts from the subclavian artery down to the brachial artery,
radial and ulnar arteries,
and site of anastomosis.
·Venous assessment comprises cephalic and basilic veins,
perforator veins,
brachial veins,
subclavian vein and site of anastomosis.
Items to be assessed for each vessel :
· The depth from the skin surface
· Internal vessel diameters
· Wall thickness and irregularities
· Vessel courses
· Steno-occlusive lesions
· Focal color aliasing
· Peak systolic
· Flow Volume
Useable Fistulae usually have :
Flow volume greater than 600mL/min
Diameter at least 0.6cm
Not more than 0.6cm deep
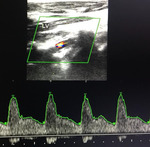
Measurement of flow volume
Volume (ml/min) = Cross-sectional area (cm2) x Mean Velocity (cm/sec) x 60
The recommended sites for measurement of flow are the feeding artery and the draining vein.
Flow volumes < 300 carries high risk of occlusion,
while flow volumes >3.000 in adults and >700 in children has a high risk of high cardiac output failure.
Causes of Immature fistula
Maturation of AVF depends on a variety of forces induced in the vascular system following AVF formation.
Remodelling of the arterial limb intimal layer will lead to vessel dilatation,
which will allow the arteries to accommodate more blood; while at the venous side,
the process can result in excessive intimal thickening resulting in narrowing of the venous limb and subsequent stenosis and thrombosis,
eventually failure of AVF maturation.
The presence of one or more accessory veins can contribute in failure of fistula maturation if seen within 10 cm from the anastomosis site.
1- Stenosis and Occlusion
Duplex ultrasound detects stenosis which can lead to decreased flow within the AVF.
Stenosis most commonly occurs at the arteriovenous anastomosis,
yet it could also occur at the feeding artery,
draining vein or the central veins.
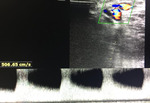
Image Findings
- Percentage of diameter reduction; significant stenosis is reported if there’s >50% diameter reduction
- Aliasing at site of stenosis
- PSV (Anastomosis PSV > 400 cm/sec,
Draining vein PSV > 300 cm/sec)
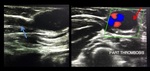
2- Thrombosis
Thrombosis is the most common cause of access failure,
it could be an early or a late complication.
Duplex ultrasound is the most accurate non invasive procedure to detect thrombus formation.
Image Findings
The site,
extension and age of the thrombus are easily detected by Duplex ultrasound.This can help in decision making with regards to the treatment; whether the patient is candidate for thrombectomy or not.
3- Steal Syndrome
AVF dialysis related steal syndrome isn’t a frequent complication,
yet it’s serious with significant patient implications including pain,
loss of extremity function or loss of access.
Duplex Findings
Reversal of direction of flow directed to the fistula,
noted in the radial artery distal to the anastomosis site.
4- Aneurysm
Aneurysm is a common serious complication.
Aneurysms occur due to either weakened wall from inappropriate cannulation,
or due to increased intraluminal pressure for proximal venous stenosis.
It could also be due to repeated cannulation of the arterialized vein.
Presence of ulcerated skin indicates by-pass and excision of the aneurysm to prevent massive hemorrhage.
Image Findings
US gray scale shows focal dilatation of the venous side of the fistula.
The presence of intraluminal thrombosis,
obstructive kinks and a rapidly enlarging aneurysm will probably require surgical intervention.
5- High output Cardiac Failure
Patients present with symptoms of heart failure.
Ligating the access or banding are the recommended treatment options.
Image Findings:
Flow volume >3L/min in adults.
6- Infection and Hematoma
Abscess and hematoma are diagnosed by US gray scale in combination with Duplex ultrasound.
Hematoma should be serially monitored to assess the size.
Additionally,
Color Doppler would better be used to assess any fluid collection adjacent to the fistula.