In our study,
we only illustrated central nervous system (CNS) involvement of TS.
Four common CNS abnormalities were found.
A patient could present more than one feature.
Tubers (grossly akin to potato tubers),
after which the disease tuberous sclerosis is named,
are glioneuronal hamartomas composed of enlarged atypical and disorganized neuronal and glial elements with astrocytosis.
They were found in all patients and were multiple and bilateral in 8 patients (57,1%).
They were located in the frontal lobes in 10 patients (71,4%) although they could usually appear anywhere in the parenchyma from the cortex to white matter.
On CT,
tubers appeared hypodense.
They were calcified in 7 patients (50%) and showed enhancement in only 14,2% of cases (n=2).
MRI is more applicable than CT for detection of cortical tubers.
Types of tubers have been described based on their imaging appearance on MRI:
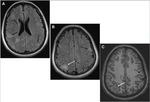
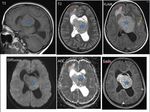
- Type A tubers were mildly hyperintense on T2WI/FLAIR,
isointense on T1WI,
and hence harder to detect.
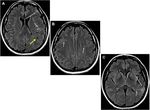
- Type B tubers were hyperintense on T2WI and hypointense on T1WI.
Fig. 2
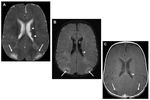
- Type C (cystic) tubers were prominently hyperintense on T2WI,
centrally suppress on FLAIR,
and are hypointense on T1WI Fig. 3 .
Patients with type C tubers predominance have more severe manifestations,
have a higher incidence of subependymal Giant Cell Astrocytoma (SEGA),
and have been associated with TSC2 gene mutations.
Calcified lesions had hypointense signal on T2* weighted sequences.
Only 14,2% of cortical tubers (n=2) was enhanced by MRI.
On diffusion tensor imaging,
tubers had decreased fractional anisotropy (FA) and increased apparent diffusion coefficients (ADCs).
- Subependymal Nodules (SENs)
SENs are hamartomatous lesions that are scattered along the ependymal surface of the lateral ventricles.
Although they can occur anywhere along the lateral ventricle,
they are most common at the caudothalamic groove in the region of the foramen of Monro.
They usually occur as multiple nodules.
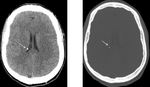
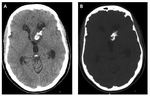
CT is a useful tool for detection of subependymal nodules.
They were present in all patients and appeared as a multiple small foci along the lateral ventricles bilaterally on unenhanced CT.
They contained dense calcification in 12 patients (85,7%),
thus more than are cortical tubers Fig. 4.
At MRI,
SENs were hyperintense on T1-weighted images and iso to hyperintense on T2-weighted images.
They had lower signal intensity on T2-weighted images than do cortical tubers,
probably because subependymal nodules have high water content.
The T2 signal depends on whether they are calcified.
Most SENs (85,7%) were calcified and showed enhancement in 2 patients (14,2%) but enhancement does not imply that a nodule is going to transform into a SEGA or that surgical intervention is necessary. Fig. 5
- White Matter Abnormalities
They are harder to identify by CT.
On MRI,
it included:
a) Superficial white matter abnormalities associated with cortical tubers,
b) Radial white matter bands,
and
c) Cystlike white matter lesions.
a) Superficial white matter abnormalities were present in 4 patients (28,5%) and were seen as high-intensity areas on T2-weighted images and decreased-intensity areas on T1-weighted images.
They are related to almost all cortical tubers.
They reflect reduced myelin or increased gliotic reaction.
Fig. 6
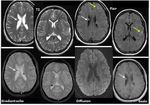
b) Radial Migration Lines (RMLs) were present in 7 patients (50%).
They are the most common lesions in TS.
They were seen on MRI as thin straight or curvilinear bands of hyperintensity on T2/Flair-weighted images and iso- to hypointensity to normal white matter on T1-weighted images run from ventricular or juxtaventricular white matter to the deep surface of cortical tubers or normal-appearing cortex.
They were thus most commonly identified in the subcortical white matter.
These lines did not enhance.
They represent arrested migratory neurons and glial cells.
They were bilateral and located predominantly in frontal lobes.
They uncommonly involve cerebellar white matter.
Fig. 7
The strong correlation between RML,
tubers,
and subependymal nodules suggests that these lesions originate from a common biological dysfunction in the periventricular zone.
c) White matter cystlike lesions were located in deep white matter,
typically near the lateral ventricles.
At MRI,
they were seen in 1 patient (7,1%) as small well-demarcated lesions of similar intensity to that of cerebrospinal fluid with all sequences.
They resemble perivascular spaces.
These lesions are considered rare.
Although the pathogenesis of cystlike lesions remains unclear,
they are considered to reflect cystic degeneration of white matter or dilated perivascular spaces.
- Subependymal Giant Cell Astrocytoma (SEGAs)
SEGAs are the most common brain tumors in TS.
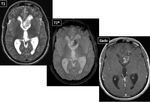
They occured in 4 patients (28,5%) and were unilateral in all cases.
SEGAs were isodense or hyperdense on CT and showed calcifications in 3 cases.
Fig. 8
On MRI,
they were hypointense/isointense on T1WI and hyperintense on T2WI.
They are vascular tumors,
with intense enhancement,
particularly in noncalcified lesions.
Fig. 6 and Fig. 9
The typical location of SGCAs was in foramen of Monro,
leading to obstructive hydrocephalus.
They are believed to arise from SENs but,
unlike SENs,
are larger tumors (>1 cm) with more intense enhancement and show growth,
with a growth rate of less than 0.5 cm/y in longest dimension.
- Infratentorial abnormalities :
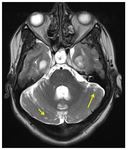
Cerebellar tubers were found in 3 patients (21,4%) and appeared as a wedge-shaped lesions (presumably from the inward migration of the granule cell neurons from the surface) that were hyperintense on T2WI and hypointense to isointense on T1WI.
Fig. 10 They were calcified in 1 patient and showed enhancement in one patient (33,3%) than supratentorial tubers enhancement (14,5%).
A zebralike pattern of enhancement has been described,
presumably reflecting the cerebellar anatomy,
with interposed cerebrospinal fluid–filled sulci.
Other infratentorial abnormalities seen in TS included :
- Linear and gyriform cerebellar folia calcifications,
- Vermis and cerebellar hemispheric hypoplasia,
and agenesis.
- Cerebellar atrophy occured in 2 patients but it is unclear whether this is from the presence of cerebellar tubers,
or a primary aberrant neuronal developmental process,
or a sequela of seizures and treatment of the same.