CT of the soft tissues of the head,
neck and chest is the imaging of choice for assessing cervicofacial cellulitis.
Ct interpretation and evaluation require a good knowledge of the anatomy and CT anatomy to understand the modalities of local and distant spread of the disease.
v Ct anatomy of head and neck fascia and compartments
Cervical fascia
Facial planes divide the neck into potential spaces.
The two main fascial divisions of the neck are the superficial cervical fascia and deep cervical fascia.
Deep cervical fascia is again divided into an investing layer,
pretracheal fascia and prevertebral fascia.
The superficial fascia is just beneath the dermis and covers platysma and muscles of the expression.
Fascial spaces or compartments
For educational purposes,
spaces in the head and neck can be divided into cranial (related to the skull and face) and cervical (related to the cervical spine),
although these distinctions are not absolute.
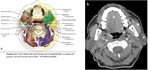
1. Cranial fascial “spaces” (Figure 1)
The cranial fascial spaces include the spaces relared to the parotid gland,
muscles of mastication,
and the submandibular gland.
Parotid space. The deep lobe of the parotid gland extends posteromedial to the mandible and forms a lateral border of the parapharyngeal space.
The spread of infection from the parotid to the parapharyngeal space indicates that the fascia covering this part of the parotid does not provide a functional barrier.
Masticator space.
It is limited by the masseter,
pterygoid,
and temporal muscles in continuity with but not including the superficial and deep temporal spaces.
Superficial and deep temporal spaces. The superficial temporal space is the space between the temporal fascia covering the temporalis and the temporoparietal fascia.
The deep temporal space lies betwwen the temporalis,
the periosteum of the temporal bone,
and the lateral pterygoid muscle.
Both spaces freely communicate anteriorly and the deep temporal space communicates with the masticator space.
Infratemporal space. It is the post-maxillary region between the ramus of the mandible laterally and the pharyngeal wall medially inferior to the zygomatic arch.
Buccal space. It is bordered anterolaterally by subcutaneous tissue and the zygomaticus major,
minor and risorius muscles; medially by the buccinator; and posteriorly by the mandible,
masseter and pterygoid muscles.
Continuity of the buccal fat pad with the temporoparietal fat pad is well described.
Infection in this region is stated to always involve the masticator compartment; and spread into the parotid,
temporal and submandibular spaces occurs with disease progression.
Submandibular space.
It is subdivided into a sublingual space superior to the mylohyoid,
a submaxillary space inferior and lateral to the mylohyoid,
and a submental space centrally.
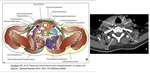
2. Cervical fascial “spaces” (Figure 2)
The cervical fascial spaces include the historical “deep spaces”- the parapharyngeal,
retropharyngeal,
danger,
prevertebral,
and visceral spaces- as well as the more recently defined pharyngeal mucosal and anterior and posterior cervical spaces.
Parapharyngeal space. It is commonly described as an inverted pyramid or triangle with the skull base superiorly and the greater cornu of hyoid bone or mandible inferiorly.
Laterally,
it is bordered by the medial pterygoid muscle and parotid gland; posteriorly by the prevertebral muscles or carotid sheath,
and medially by the visceral fascia covering the pharyngeal muscles.
Carotid space. This is bound by the carotid sheath.
Pharyngeal mucosal space. It is the space deep to the visceral layer of deep cervical fascia (DCF) encircling the pharyngeal constrictor muscles between the skull base and cricoid cartilage.
The pharyngeal mucosa represents the deepest limit of this space.
Retropharyngeal and danger spaces. There are two spaces bounded by visceral fascia anteriorly,
prevertebral fascia posteriorly,
and the alar fascia in betwwen- known as the retropharyngeal space (anterior) and the danger space (posterior).
The retropharyngeal space contains lymph nodes,
whereas the danger space has no specific contents.
Prevertebral or perivertebral space. It is a space between the middle layer of deep cervical fascia (MLDCF) anteriorly and the deep layer of deep cervical (DLDCF) posteriorly,
extending round to the spinous processes posteriorly.
It has been divided into anterior or “prevertebral” and posterior or “paraspinal” portions by fascial attachments to the transverse processes of the cervical vertebrae.
Anterior and posterior cervical spaces. They are region occupied by the anterior and posterior triangles of the neck.
The posterior cervical space is described between the DLDCF covering the scalene muscles and the sternocleidomastoid- trapezius fascia,
and is limited anteriorly by the carotid sheath.
The posterior cervical space theorretically communicates with the axilla,
but spread of infection between these sites is uncommon.
Visceral space. It is a potential space between the trachea,
oesophagus,
and thyroid,
and their surrounding visceral fascia.
v Results of our study
CT revealed a facial topography of the infection in 22 cases and cervicofacial topography in 10 cases.
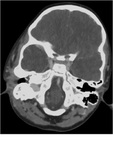
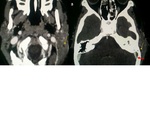
It showed superficial cellulitis in 22 patients with subcutaneous fat densification in fourteen of them (Figure 3) and abscess collection in eight of them (Figure 4).
An extension to the deep spaces was noted in 10 patients.
Submandibular space involvement was noted in 4 patients (Figure 5),
retropharyngeal one in 1 patient (Figure 6).
Posterior cervical space was involved in 1 patient (Figure 7),
and the infection involved multiple deep spaces in 4 patients (Figure 8,
9).
Infections transgressing fascial boundaries and involving vertically oriented spaces necessitate often surgical treatment.
The risk is the vertical spread of the infection along and around the upper airways and the upper digestive tract to the mediastinum and / or the skull base.
Venous thrombosis complication was noted in 3 patients (Figure 10), osteitis in 4 patients and periosteal abscess in 1 patient.
The common cause of infection in our patients was due to odontogenic origin identified in 12 patients.
Tonsilopharyngeal origin was noted in 2 patients and traumatic one in 1 patient with cellulitis involving the posterior cervical space.
We diagnosed one case of tubercular etiology involving the retropharyngeal space (Figure 11). However,
the infection etiology was unknown in 16 patients.