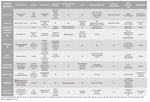
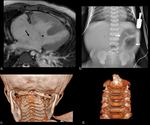
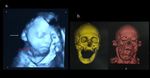
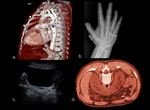
Down syndrome (Figure 1)
Genetic etiology: Is the most common trisomy and also commonest chromosomal disorder, dependent on maternal risk.
Incidence 1 : 700-1000 live births,
dependent of implementation of antenatal screening
Clinical postnatal features: depressed nasal bridge,
macroglossia,
cerebellar and vermian hypoplasia,
Moyamoya syndrome; congenital heart disease 40% (septal defects); anal or duodenal atresia,
Hirschprung disease,
omphalocele; eleven ribs,
deelopmental hip dysplasia,
atlanto-axial subluxation and atlanto-pccipital inestability.
Best imaging tool: the clinicopathological spectrum is wide,
that why it is better to approach the syndrome by systems.
Cardiac MR an echocardiogram are useful for the diagnosis and follow-up of cardiac anomalies.
Prognosis: Survival can be variable with the mean survival often considered at 20 years
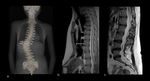
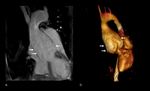
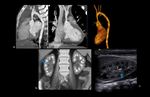
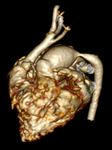
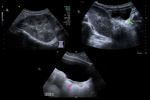
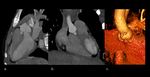
Marfan syndrome.
(Figure 2 and 3)
Genetic etiology: inherited autosomal dominant connective tissue disorder (FBN1 mutation)
Prevalence: 2-3 : 10,000 patients
Clinical features:
Cardiovascular: Aortic root dilation at level of sinuses of Valsalva (75%),
ascending aortic dissection,
mitral valve prolapse (50-70%),
Skeletal: Pectus excavatum,
pectus carinatum,
long arms & legs,
arachnodactyly,
joint hypermobility,
scoliosis,
thoracic lordosis,
pes planus
Ocular: Ectopia lentis (50%)
Pulmonary: Spontaneous pneumothorax (5-10%),
apical blebs
Skin: Stretch marks in absence of weight changes or pregnancy,
recurrent hernia
Dural ectasia
Best imaging tool: AngioCT in acute setting to exclude aortic dissection or rupture.
Ecocardiography or cardiac MRI are the best choice for follow-ip of aortic dilatation or valvular disease.
Prognosis: 90% of the death from cardiovascular complications,
improved detection and treatment has helped tu prolong survival to nearly normal levels.
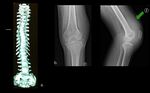
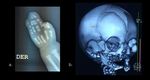
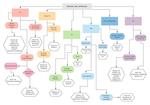
Ehlers-Danlos (Figure 4)
Genetic etiology: Multiple genetic defects apply to collagen synthesis
Clinical features: skin and vascular fragility,
hyperelastic joints,
disproportionate limb legthening
|
Classification system,
the most common are type I-IV
|
|
Type I (gravis)
|
Hyperextensible skin,
sever joint hypermobility,
skin fragility
|
|
Type II (mitis)
|
The milder form of cutaneous and joint manifestation
|
|
Type III
|
Predominance of severe joint hypermobility
|
|
Type IV (acrogenic)
|
Most sever form with premature aging,
spontaneous vascular and bowel rupture (vascular syndrome)
|
|
Type V
|
Rare,
skin stretching
|
|
Type VI
|
Ocular abnormalities
|
|
Type VII
|
Severe joint hypermobility,
dislocations,
skin hyperextensibility with scarring and bruising
|
|
Type VIII
|
Prominent periodontal disease,
rare
|
Best imaging tool: it is best to do the approach according to the systems affected
Hemifacial microsomia.
(Figure 5)
Also known as craniofacial microsomia or otomandibular dysostosis.
Is the second most common congenital facial anomaly,
with a prevalence of 1 : 3,500 births
Genetic etiology: genetic and environmental factors.
Usually sporadic.
Pathology: results from an abnormal development of the 1st and 2nd brachial arches
55% of the patients have extracranial abnormalities.
Cervical spine fusion/segmentation anomalies
CNS (variable): ventriculomegaly,
cerebellar hipoplasia,
cephalocele
Clinical features: external and middle ear anormalies,
unilateral mandibulean temporomandibule joint hypoplasia,
small muscle of mastication.
Best imaging tool: CT for mandibule and temporal bones,
MR for CNS anomalies
Prognosis: depends on the severity and phenotypic heterogeneity
Williams-Beurnen syndrome (Figure 6)
Also known as Williams syndrome,
this syndrome has a constellation of findings.
Genetic etiology: deletion of the Williams-Beurnen syndrome chromosome.
Prevalence 1: 10,000 persons
Clinical Features: craniofacial dysmorphism (pixie facies) Vascular stenosis of middle and large vessels,
cognitive impairment,
diverticular disease,
nephocalcinosis,
Type I Chiari malformation scoliosis.
Best imaging tool: Cardiovascular complications (supravalvular aortic stenosis,
pulmonary arterial stenosis) are the major cause of death in this patients,
that is why MR or CT angiography play a vital role.
Ultrasound is a useful tool to evaluate the presence of nephocalcinosis.
Prognosis: the morbidity and mortality is affected by the cardiovascular,
endocrine,
and nervous systems findings.
DiGeorge syndrome (22q11.2 deletion syndrome) (Figure 7)
Also know as the velocardiofacial syndrome.
Genetic etiology: deletion of the short arm of chromosome 22,
autosomal dominant inherited
Prevalence 1: 4000 live pregnancies
Clinical presentation: Cleft lip +/- palate,
Congenital heart disease (conotruncal anomalies),
characteristic facies,
malformation of 3rd and 4rd pharyngeal pouches.
Best imaging tool: CT scan with contrast can be extremely useful to approach the congenital cardias anomalies,
head and neck CT is required to identify the presence of aberrant course of internal carotid arteries,
hypoplastic adenoids,
and middle ear anomalies.
also to follow the multiple infections to which these patients are at risk because of their characteristic immunodefiency.
The prenatal diagnosis is likely but is often missed or delayed because pregnant women are not routinely screened for this rare entity.
Prognosis: highly variable,
and outcome is determined by the severity of complications
Apert syndrome.
(Figure 8)
Also known as type I acrocephalosyndactyly
Genetic etiology: defect on the fibroblast growth factor receptor 2 (FGFR2) gene,
located on chromosome 10q26.
Can be inherited as an autosomal dominant,
but most cases are sporadic
Present in 1: 65-80,000 pregnancies.
Associations: CNS,
cardiac (10%),
genitourinary anomalies and symphalangism.
Clinical Triad: craniosynostosis,
syndactyly and maxillary hypoplasia.
Best imaging tool/pearls: 3D ultrasound can help to identified abnormalities in prenatal stage.
Prognosis: airway compromise may be the cause of an early death. Early repair of craniosynostosis does not prevent intellectual impairment,
although it can help to prevent intracranial hypertension.
Turner syndrome (Figure 9)
Genetic etiology: 45X,
is the most common of the sex chromosome abnormalities.
Incidence: 1: 2000-5000 of live births (in utero rate is much higher)
Clinical features: primary amenorrhea,
webbed neck,
Madelung deformity,
scoliosis; streak ovary and uterus; pyloric stenosis.
Has been associated with potentially lethal cardiac abnormalities (aortic coarctation)
Best imaging tool: US is key for prenatal diagnosis,
also for the approach of primary amenorrhea.
MRI for cardiac evaluation abnomalies
Prognosis: very variable is dependent on associated anomalies
MURCS association.
(Figure 10)
Müllerian duct aplasia + Renal aplasia/ agenesis + Cervicothoracis Somite dysplasia
Genetic etiology: the cause still unknown ,
mutation of WNT4 has been reported.
Most of the cases are sporadic,
but actual evidence confirm that may be inherited as an autosomal dominant trait with incomplete penetrance.
Clinical features: primary amenorrhea (2nd most common cause),
with development of secondary sexual characters.
Differential diagnose: Goldenhar syndrome,
VACTERL association and Turner syndrome
Best imaging tool: Pre and postnatal ultrasound can be helpful to the müllerian an urogenital anomalies.
In case to suspect a Müllerian defect spine radiographs can be useful to ruled out or confirm the association with vertebral alterations.
Prognosis: varies and is probably dependent on the extent and severity of renal abnormalities
Shprintzen-Goldberg syndrome.
(Figure 11)
Also know as Marfanoid-craniosynostosis syndrome,
is a rare condition affecting many parts of the body
Genetic etiology: autosomal dominant disorder o sporadic caused by mutation of SKI gene
Prevalence: unknown
Pathology: connective tissue disorder
Clinical features: craniosynostosis,
intellectual disability,
hypertelorism,
arachnodactyly,
pectus deformity,
scoliosis,
joint laxity and sinus Valsalva aneurysm
Differential diagnosis: Marfan syndrome (heart problems are more likely and no developmental delay)
Best imaging tool: plain radiograph for skeletal survey,
brain and heart MRI
Prognosis: does not alter lifespan,
although complications from associated abnormalities,
such as intellectual impairment or respiratory problems,
may be expected