Type:
Educational Exhibit
Keywords:
Education and training, Venous access, Catheters, Ultrasound, Fluoroscopy, Vascular, Spleen, Interventional vascular
Authors:
G. Kumar1, M. kolber2, H. shah2, M. Still3, D. Lamus2, S. Kalva4, M. reddick2; 1Plano/US, 2Dallas/US, 3Dallas, TX/US, 4BOSTON, MA/US
DOI:
10.26044/ecr2019/C-3726
Findings and procedure details
In this educational exhibit,
we will present several cases of trans splenic venous access used in the creation of TIPS,
variceal embolization,
and portal venous recanalization with stenting,
etc.
Splenic tracts closures were performed with plugs,
coils or gel foam.
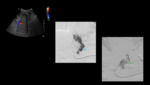
Case 1: (Figure 1) A 54 years old pt with h/o Alcoholic cirrhosis presented with acute onset hematemesis.
EGD was unsuccessful.
Emergent abdominal CT scan demonstrated thrombosed main portal vein (MPV) with large gastric varices.
Transjugular or percutaneous transhepatic portal venous access was deemed difficult.
Ultrasound-guided access to the splenic vein was obtained (red arrow) using a 25 G needle.
Access was then upsized to a 5 Fr hemostatic sheath.
Splenic venogram was performed and a large gastric varix (blue arrow) was identified.
The varix was selected and successfully embolized with coils (green arrow). The splenic access track was closed with gel foam slurry.
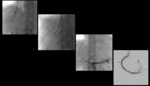
Case 2: (Figure 2) A 69 years old pt with Non-alcoholic steatohepatitis and cirrhosis (NASH cirrhosis) presented with refractory ascites.
Review of her imaging studies revealed chronic thrombosis of the intrahepatic portal veins.
After obtaining trans-splenic access,
a loop snare (red arrow) was advanced into the patent section of the portal vein and used as a target for Colapinto needle (blue arrow) advanced from trans-jugular venous access.
Once the needle was able to puncture through the snare loop,
a guidewire was advanced through the needle and a through and through access was established.
The track was dilated and a TIPS stent (green arrow) was successfully inserted.
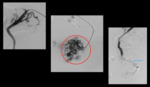
Case 3: (Figure 3) A 66 years old pt with h/o colon cancer s/p sigmoid resection and colostomy,
presented with acute onset bleeding from the colostomy site.
Review of cross-sectional imaging revealed extensive liver metastasis and portal vein thrombosis,
and a complex network of portosystemic collaterals (varices) surrounding the colostomy site.
After an unsuccessful attempt at percutaneous access to the varices,
trans-splenic access to the splenic vein was obtained.
The catheter was then manipulated into the inferior mesenteric vein (IMV).
Venogram confirmed the presence of portosystemic collaterals (red circle).
The IMV was then successfully embolized with nBCA/ lipiodol and coils (blue arrow).
The splenic track was closed with gel foam slurry.
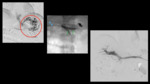
Case 4: (Figure 4) A 58 years old pt with chronic HCV cirrhosis presented with acute onset hematemesis and gradually worsening ascites.
EGD was unsuccessful.
CT abdomen revealed chronic occlusion of the main portal vein as well as the central segments of splenic vein and superior mesenteric vein (SMV).
Large gastric and several small mesenteric portosystemic collaterals (varices) were also evident.
After obtaining trans-splenic access,
splenic venogram confirmed CT findings.
Successful coil embolization of the gastric varices was performed.
Subsequently,
assisted with two percutaneous transhepatic portal venous accesses,
the splenic and mesenteric veins were recanalized and kissing stents were successfully inserted.
Subsequent CT study a few days later demonstrated patency of the stents as well as the resolution of gastric and mesenteric varices.