Pathophysiological considerations
NMOSD is immunopathologically distinct of other demyelinating diseases because it has a target: AQP4.
Aquaporin-4 is a protein molecule,
part of a transmembrane water channel,
that plays a role in water/sodium homeostasis,
cardiovascular regulation,
feeding,
and energy homeostasis,
immunomodulation,
vomiting.
It is expressed in the spinal cord,
optic nerve,
hypothalamus,
periventricular areas,
brainstem,
and area postrema,
and in basal cells of the olfactory epithelium as well.
Autoantibodies cause complement activation,
cellular damage,
demyelination,
and necrosis,
leading to blood-brain barrier disruption.
Lesions occur predominantly where these channels are expressed,
starting in the area postrema of medulla oblongata3.
Clinical and epidemiological features
NMO has a preference for Afro-Caribbean female patients in their thirties; it may be found in pediatric patients,
in whom it tends to have a better prognosis.
It may have a broad spectrum of manifestations,
ranging from mild to severe.
Clinical manifestations depend on the location of lesions.
- Optic neuritis
Bilateral and severe vision loss.
- Complete spinal cord syndrome
- Area postrema syndrome
Nausea,
hiccups,
and vomiting.
- Diencephalic syndrome
Narcolepsy/hypersomnia,
hypothermia,
anorexia,
inappropriate diuresis.
- Brainstem syndrome
Ataxia,
oculomotor dysfunction,
long tract signs. 4,6
Diagnostic criteria (2015)
At least one core clinical characteristic
AQP4-Ab (+)
Exclusion of alternative diagnoses
At least two core clinical characteristics occurring as a result of one or more clinical attacks and all of the following requirements:
- At least one core clinical characteristic must be optic neuritis,
acute myelitis with longitudinal extensive transverse myelitis (LETM),
or area postrema syndrome.
- Dissemination in space (two or more different core clinical characteristics).
- MRI requirements,
as applicable.
- AQP4-Ab (-) or testing unavailable.
- Exclusion of alternative diagnoses.
❖ Core clinical characteristics
Optic neuritis,
acute myelitis,
area postrema syndrome,
acute brainstem syndrome,
symptomatic narcolepsy or acute diencephalic clinical syndrome with NMOSD-typical diencephalic MR lesions,
symptomatic cerebral syndrome with NMOSD-typical brain lesions.
❖ MRI requirements for patients with AQP4-Ab (-) or unknown status
- Acute optic neuritis(requires one of the following):
Brain MRI showing a T2-hyperintense lesion or a T1-gadolinium-enhancing lesion extending over more than one-half of the optic nerve length or involving the optic chiasm.
- Acute myelitis (requires one of the following):
Lesion extending over three or more contiguous vertebral segments - longitudinal extensive transverse myelitis(LETM).
Spinal cord atrophy involving three or more contiguous segments
- Area postrema syndrome
o Dorsal medulla/area postrema lesion
- Acute brainstem syndrome
o Periependymal brainstem lesions 5
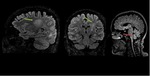
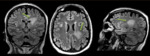
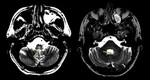
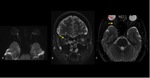
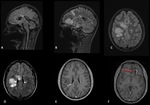
Image findings
MRI is the primary modality.
- Brain: it may be normal.
Asymptomatic abnormalities are present in most seropositive patients.
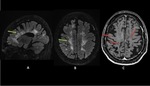
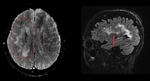
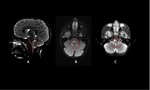
When present,
lesions show the distribution of aquaporin,
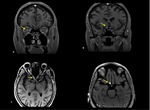
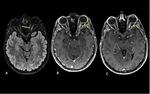
involving periventricular areas (with no "Dawson’s fingers" sign),
corpus callosum (marbled patterned lesions), periaqueductal grey matter,
dorsal pons/medulla,
hypothalamus/medial thalamus; the hemispheric white matter lesions may be larger than 3 cm in diameter (spilled-ink appearances or spindle-shaped),
rarely tumecfative.
There may also be punctate white matter lesions or even envolve corticospinal tract.1,6,7
(Fig. 1, Fig. 2, Fig. 3)
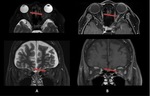
- Orbits: optic neuritis,
with optic nerves hyperintensity and swelling on T2 weighted sequences (Fig. 4),
with contrast enhancement in acute inflammatory phase(Fig. 5, Fig. 6) - these findings are typically bilateral and involve long segments of the optic nerves,
frequently extending to the chiasm.
In chronic phases,
there is optic nerve atrophy with hyperintensity on T2 WI.
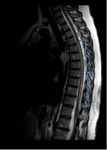
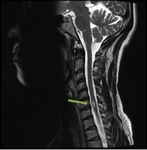
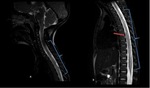
- Spinal cord: extense areas of hyperintensity on T2 WI involving at least three vertebral segments (Fig. 7).
In the acute phase,
there may be spinal cord swelling.
Transverse myelitis may be present in some cases,
as the longitudinal extensive transverse myelitis.
Contrast enhancement is variable (ring-shaped,
thin ependymal enhancement,
ependymitis-like).
Differential diagnosis
- Multiple Sclerosis (MS)
Is the main differential diagnosis for NMOSD.
Both are inflammatory demyelinating diseases affecting the central nervous system,
with outbreaks and remissions (with earlier age of onset on MS).
MS does not have a specific serologic marker.
Optic neuritis on MS usually presents with fewer symptoms (severe visual loss is uncommon).
Area postrema syndrome (nausea,
hiccups,
and vomiting) is rare on MS and common on NMOSD.
On cerebrospinal fluid exam,
it has oligoclonal bands in up to 97% patients,
while in NMOSD this is very unusual.
Imaging findings
Optic neuritis lesions tend to be unilateral and short (Fig. 8),
different from NMOSD,
that involves superior/inferior quadrant extending to the chiasm.
Spinal cord impairment is relatively uncommon in pediatric patients and rare in adults.
It presents as posterior,
asymmetrical and peripheral lesions,
typically extending over one or two vertebrae (Fig. 9).
Brain lesions present as perpendicular to lateral ventricles and corpus callosum (known as "Dawson’s fingers",
perivenular distribution pattern - Fig. 10, Fig. 11).
Lesions are usually smaller and cortical/juxtacortical.
Brain atrophy is severe in chronic cases. 2,3
- Acute Disseminated Encephalomyelitis (ADEM)
A demyelinating disorder that most commonly affects children and young adults.
It presents with encephalopathy,
which is generally monophasic (a key finding for the diagnosis). There is no specific biological marker or confirmatory test. It should be considered especially if onset occurs one to two weeks after viral infection or immunization.
Clinical features include systemic symptoms like a headache, decreased level of consciousness,
cranial nerve palsies,
fever,
seizure,
hemiparesis,
and movement disorders.
In children,
behavioral changes may be the main findings.
Imaging findings
Brainstem and spinal cord are involved,
best seen onT2 and FLAIR WI images.
Contrast enhancement is sometimes seen in acute lesions,
almost always with the same inflammation phase (monophasic disease).
Multiple,
bilateral and asymmetric lesions in the deep and subcortical white matter,
such as thalami and basal ganglia are common,
while periventricular white matter is generally spared (Fig. 12,
Fig. 13).
The lesions range from less than 5 mm to 5 cm. Spinal cord lesions tend to be larger,
similar to NMO-SD (Fig. 14).8