The injured knee joint is examined using an X-ray in standard projections, CT and MRI. Data from all three imaging modalities are used to analyze anatomical risk factors. The most significant predictors of dislocation are femoral trochlear dysplasia, patella alta, tibial tuberosity lateralization, increased lateral patellar tilt.
Femoral trochlear dysplasia
Femoral trochlear dysplasia is most often and important predictor of recurrent dislocations and unsuccessful surgical treatment.

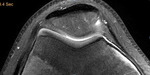
Fig. 1: Normal trochlea.
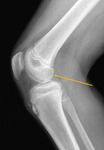
The classification of trochlear dysplasia by Dejour [7] is widely known. The assessment in this classification is based on the analysis of a radiograph in a true lateral projection (Fig. 2) .

Fig. 2: True lateral radiograph of the knee. The projection is considered to be truly lateral, where the posterior surfaces of both condyles of the femur coincide.
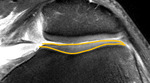
The morphology of the femoral trochlea is more often studied quantitively using axial images of MRI (Fig. 3).

Fig. 3: The use of axial images of MRI is preferable, since the surface of the articular cartilage of the block on them is fully visualized In children, articular cartilage is thicker than in adults, and can vary with age. The difference between the bony and cartilage contour of femoral trochlea.
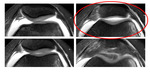
It is customary to take measurements at the most proximal image with an intact cartilaginous trochlea ( Fig. 4 ).

Fig. 4: Selection of image for measurements.
A total of 4 parameters are estimated: the trochlear sulcus angle, the trochlear inclination angle, facet asymmetry, and the groove depth. An important reference line is the posterior intercondylar line (Fig. 5).

Fig. 5: Сonstruction of the posterior intercondylar line. This is the line connecting the posterior surfaces of the condyles of the femur and many measurements are taken with the use of it.
Lateral trochlear inclination angle (Fig. 6)

Fig. 6: Мeasurement of lateral trochlear inclination angle.The angle is measured between the posterior intercondylar line and the line drawn along the cortical layer of the lateral facet.The average inclination angle is 27 degrees, an angle less than 11 degrees indicates the presence of dysplasia [20].
А. Normal trochlea, angle is 27 degrees. B. Dysplasia, angle is 6 degrees
Trochlear facet asymmetry (Fig. 7).

Fig. 7: Мeasurement of trochlear facets asymmetry. The ratio of the medial to the lateral facet length defines trochlear facet asymmetry. Lenghts measurements are made on the cartilaginous surface. A ratio of less than 0.4 indicates trochlear dysplasia.
А. Normal trochlea, ratio is 0,57. B. Dysplasia, ratio is 0,31.
Trochlear groove depth (Fig. 8).

Fig. 8: Measurement of trochlear groove depth. Three perpendiculars are drawn to the posterior intercondylar line - from the most outstanding points of the anterior condyles and from the deepest point of the groove. Groove depth is defined as (A + B)/2 - C. Trochlear groove depth of< 3mm indicates dysplasia. А. Normal trochlea, trochlear groove depth is 6,2 mm. B. Dysplasia, trochlear groove depth is 1,8 mm.
Trochlear sulcus angle (Fig. 9).

Fig. 9: Measurement of trochlear sulcus angle. This angle is defined between the lines drawn along the cartilaginous surfaces of the lateral and medial facets of the trochlea. An angle of more than 145 degrees indicates dysplasia. A. Normal trochlea, angle is 138 degrees. B. Dysplasia, angle is 166 degrees.
The radiologist should note a change in the shape of the groove, its flattening, the convex shape of the trochlea, the presence of a bone spur.

Fig. 10: Severe trochlear dysplasia, the convex shape of the trochlea.
The use of deepening trochleoplasty is possible in skeletal mature patients [10, 26].
Pаtella alta
The patellar height is determined using the Insall-Salvati and Caton-Deschamps indices (Fig. 11).

Fig. 11: Measurement of Insall-Salvati and Caton-Deschamps indices. To evaluate the Insall-Salvati index, it is optimal to use a lateral radiograph in a flexion position of 30 degrees.
The landmarks for Insall-Salvati index measurements are the most cranial and caudal aspects of the patella, and regarding the patellar tendon, the most caudal point of insertion to the patella and the most cranial point of insertion to the tibia. Insall-Salvati index = A/B.
Caton-Deschamps index is measured by using the greatest length of the patellar articular surface and the shortest line between the caudal margin of the patellar articular surface and the anterior aspect of the tibial plateau. Caton-Deschamps index = A1/B1.
Assessment on sagittal sections of CT and MRI is also possible. (Fig. 12).

Fig. 12: Assessment of Insall-Salvati index on different modalities. A sagittal image should be chosen where the length of the patella is maximal. MRI results are more accurate since the joint is in the flexion position during the scan. Patella alta is diagnosed when the Caton-Deschamps index is greater than 1.2 [5], Insall-Salvati index is greater than 1,3 [12]. А. Saggital radiograf, Insall-Salvati index is 1,45. B. CT, Insall-Salvati index is 1,31. MRI, Insall-Salvati index is 1,41.
In cases with severe patella alta, complex surgical intervention may include distalization of tibial tuberosity [26].
Tibial tuberosity lateralization.
Lateralization is usually evaluated using the TT-TG index (Fig. 13).

Fig. 13: Evaluation of TT-TG index. It is preferable to measure it on axial images of CT with a fully extended joint. Two perpendiculars are drawn to the posterior intercondylar line for measurement: from the deepest point of the trochlear groove and the most prominent point of tuberosity. The distance between these perpendiculars is the TT-TG index. The TT-TG index is considered normal when varies from 10 to 15 mm, high - more than 20 mm, 15-20 mm - transitional values. When evaluating the TT-TG index in children, it is worth remembering that it increases with growth, therefore, its final value at the time of skeletal maturity is important. A. Normal - TT-TG index is 12 mm; B. Lateralization - TT-TG index is 20 mm.
Patients with a TT-TG index of 20 mm or more are candidates for the tibial tuberosity medialization. Surgery is possible in skeletal mature patients [26].
To determine the true tibial tuberosity lateralization, the TT-PCL index was proposed [23] (Fig. 14).

Fig. 14: Evaluation of TT-PCL index.. For its measurement, axial MRI images are used. The reference line is the posterior intercondylar line of the tibia.
The TT-PCL index is defined as the distance between the medial edge of the posterior cruciate ligament at the level of attachment to the tibia and the central point of attachment of the patellar ligament to the tuberosity. Values of TT-PCL index greater than 24 mm are abnormal and indicate true lateralization of tuberosity. Normal TT-PCL index, 18 mm.
Lateral patellar tilt.
The most simple, convenient and clinically significant method for evaluation of the the patella position relative to the femoral trochlea is the determination of patellar tilt angle [8] (Fig. 15).

Fig. 15: Assessment of lateral patellar tilt. It is preferable to assess the patellar tilt on axial CT images with a fully straightened knee joint.
To measure the patellar tilt, one need to select an image where the width of the patella is maximum. The angle between the posterior intercondylar line and the line drawn along the maximum equator of the patella should be measured.An angle of more than 20 degrees indicates an increased tension of the lateral structures and a tendency to patellar instability. A. Normal angle, 6 degrees. B. Abnormal angle, 27 degrees.
With an increased angle of patellar tilt, lateral release is often included in the surgical treatment plan [26].
Other factors
Some authors suggest evaluating the patellar articular surface shape to Wiberg (Fig. 16).

Fig. 16: Wiberg type III patella.
Femoral anteversion is an excessive internal twisting of the distal femur compared to its neck (Fig. 17).

Fig. 17: Evaluation of femoral anteversion. Anteversion can be evaluated on CT. It is the angle between the axis of the femoral neck and the posterior intercondylar line. An angle of more than 30 degrees is considered abnormal. Normal angle, 14 degrees.
In this case, surgical treatment with corrective supracondylar osteotomy can be used, including in skeletal immature patients [26].


![Fig. 6: Мeasurement of lateral trochlear inclination angle.The angle is measured between the posterior intercondylar line and the line drawn along the cortical layer of the lateral facet.The average inclination angle is 27 degrees, an angle less than 11 degrees indicates the presence of dysplasia [20].
А. Normal trochlea, angle is 27 degrees. B. Dysplasia, angle is 6 degrees](https://epos.myesr.org/posterimage/esr/ecr2020/154122/media/882695?maxheight=150&maxwidth=150)





![Fig. 12: Assessment of Insall-Salvati index on different modalities. A sagittal image should be chosen where the length of the patella is maximal. MRI results are more accurate since the joint is in the flexion position during the scan. Patella alta is diagnosed when the Caton-Deschamps index is greater than 1.2 [5], Insall-Salvati index is greater than 1,3 [12]. А. Saggital radiograf, Insall-Salvati index is 1,45. B. CT, Insall-Salvati index is 1,31. MRI, Insall-Salvati index is 1,41.](https://epos.myesr.org/posterimage/esr/ecr2020/154122/media/882933?maxheight=150&maxwidth=150)






















