Patients presenting with recurrent abdominal pain were meticulously evaluated using ultrasonogram, Doppler and CT studies based on the need of the study identified. Many of the patients were found to have vascular causes like compression of the celiac artery by the median arcuate ligament (median arcuate ligament syndrome), compression of duodenum by the superior mesenteric artery (SMA syndrome), compression of left renal vein in between superior mesenteric artery and aorta (nutcracker syndrome) in addition to the atherosclerotic manifestations and post inflammatory vascular manifestations. We present here few of the cases where vascular causes were the culprit leading to the patient's symptoms.
MEDIAN ARCUATE LIGAMENT SYNDROME
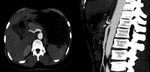
Median arcuate ligament syndrome or Dunbar syndrome refers to compression of the celiac artery at its origin by the diaphragmatic crura or the median arcuate ligament leading to upper abdominal pain. Radiologically, CT angiography shows superior indentation of the celiac artery leading to focal narrowing of the proximal celiac trunk forming a hook like appearance [1] (Fig 1 and Fig 2). There can be associated post stenotic dilatation of the celiac artery with or without evidence of collateral formation. No associated atherosclerotic changes are noted.
SUPERIOR MESENTERIC ARTERY SYNDROME
Superior mesenteric artery syndrome refers to narrow origin of superior mesenteric artery leading to compression of 3rd part of duodenum between the aorta and the artery. There is dilatation of 1st and 2nd part of duodenum with transition to collapsed duodenum noted at the level of compression by the superior mesenteric artery [2] (Fig 4). Aorto-mesenteric angle is less than 25 degree in the sagittal plane and aorto-mesenteric distance is <8mm (Fig 4). Other causes of intestinal obstruction as for example scleroderma or duodenal stricture can exacerbate the symptoms of SMA syndrome leading to added compression in the region.
NUTCRACKER SYNDROME
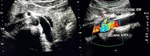
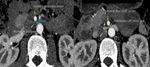
Nutcracker syndrome refers to a vascular compression disorder where the left renal vein is compressed between the superior mesenteric artery and the aorta [3] (Fig 7). The narrow angle of origin between the superior mesenteric artery and the aorta leads to compression of the left renal vein and hence results in renal venous hypertension. It commonly presents as haematuria as a result of rupture of thin-walled veins into the collecting system. It can co-exist with SMA syndrome where there is also compression of 3rd part of duodenum between the aorta and the superior mesenteric artery. Radiologically, the following features are seen:
- Left renal vein stenosis with possible development of collateral pathways (especially along the left gonadal vein).
- Reduced aortic-mesenteric angle in the sagittal plane (< 25 degree) (Fig 6).
- Compression ratio (CR) >2.2 where compression ratio is calculated as CR=P-C/C , i.e. diameter of pre-compressed vein (P) minus diameter of compressed vein (C) divided by the diameter of the compressed vein (C) (Fig 5).
SPLENIC ARTERY ANEURYSM
The most common visceral arterial aneurysm is the splenic artery aneurysm. It arises in association with atherosclerosis or secondary to fibromuscular dysplasia [4]. It most commonly arises from the distal portion of the splenic artery and is mostly saccular in nature (Fig 9 and Fig 10). Peripheral calcification is common in these aneurysms. Splenic arterial pseudoaneurysms can also occur secondary to pancreatitis or trauma. When pseudoaneurysms occur, they can arise either from the main splenic artery or from the branches.
POST –INFLAMMATORY PSEUDOANEURYSMS
Abdominal pseudoaneurysms commonly occur as a result of inflammatory changes associated with the pancreatitis. Most common arteries to be involved are the splenic artery and the gastroduodenal artery [5]. On CT angiography there is focal contrast filled outpouching with or without active extravasation of contrast (Fig 11, Fig 12, Fig 13). Early arterial embolization can prevent the high mortality associated with the rupture of these pseudoaneurysms.
RETRO-AORTIC LEFT RENAL VEIN
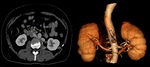
Retro-aortic left renal vein is a normal anatomical variation in the course of the left renal vein where the left renal vein courses behind the aorta to drain into the inferior vena cava [6] (Fig 8). Recognizing retro-aortic left renal vein is important in cases of retroperitoneal surgeries so as to avoid the complications associated with its injury. Sometimes, the vein can be compressed between the aorta and the vertebral body giving rise to atypical nutcracker syndrome.
CHRONIC MESENTERIC ISCHAEMIA
The most common cause of chronic mesenteric ischemia is atherosclerosis. It commonly involves the proximal portions of the celiac artery, superior mesenteric artery or the inferior mesenteric artery [7] (Fig 14, Fig 15). There is good collateralization occurring between the vascular territories of these vessels as a result of which patients experience symptoms only after two or three major mesenteric vessels are involved. Atherosclerotic plaques can lead to partial, or in advanced cases, complete occlusion of the visceral abdominal aortic branches at the level of the origin. CT angiography in these cases shows atherosclerotic changes in the abdominal aorta and the degree of narrowing of the visceral branches.
ABDOMINAL AORTIC DISSECTION
Though most commonly noted in elderly hypertensive patients, abdominal aortic dissections can also occur secondary to trauma, connective tissue diseases or in pregnancy [8]. CT angiography is the investigation of choice and can not only help in the diagnosis but also in early detection of complications associated with the dissection. CT angiography gives detail evaluation regarding the true and the false lumen, dissection and occlusion of branch vessels, aneurysmal dilatation and distal thromboembolism (Fig 16 and Fig 17).
Hence, a careful evaluation of the abdominal vessels can lead us to the diagnosis in many of the cases where we do not see obvious visceral causes of abdominal pain.