Diagnostic imaging in acute chest pain
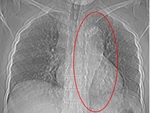
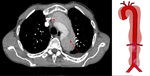
Chest radiography usually represents the first imaging modality performed in patients with widening of the superior mediastinum and displacement of aortic wall calcifications, in the appropiate clinical setting, may suggest the diagnosis of aortic dissection, however, these findings may be difficult to evaluate.
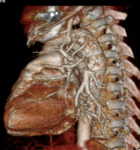
CT scan using helical technology is fast and easy to perform and can be obtained at any time of day and night; can cover large anatomic areas with good spatial resolution and short scan duration
Magnetic resonance imaging allows assessment of the mediastinum and thoracic aorta in multiple projections. Although the relatively long scan duration and the limited access to the patient may represent a drawback.
Road to computerized tomography angiography...
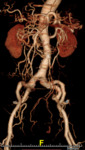
In emergency situations, the aim of the imaging modalities implemented must surpass the simple diagnosis of acute aortic dissection. Imaging should rapidly provide an overall evaluation of the entire aortic dissection including visceral branches, iliac and common femoral arteries.
The technique of CT angiography depend on the perfomance of the equipment used. The examination must explore the entire thoracic and abdominal aorta together with the iliac and common femoral arteries. The visualization and images processing are perfomed interactively on a workstation. Excessive narrow window witdh may conceal the dissected intimal flap so the window setting must be adapted for arterial exploration. Reformatted image reconstruction takes only a few minutes and can be used in emergency situations.
The maximum intensity projection (MIP) reformats appear to be less informative because they do not generally allow differentation between the two dissection channels.
To inform the study has been said...
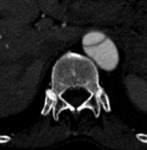
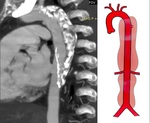
The examination begins with the acquisition of an unenhanced CT scan. It is important, because may see internal displacement of intimal calcifications, and complications, for example acute hemorrhage ( pleural, pericardial or mediastinal ). After unenhanced CT, contrast-enhanced CT is perfomed with a bolus injection of nonionic contrast material.
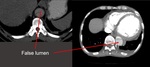
The main finding on contrast-enhanced CT, is an intimal flap that separates the true lumen from the false lumen. It is important, because this distinction recently has become particularly important for planning endovascular treatment dissection.
Differentiation of the true lumen from the false lumen in important for planning endovascular intervention. Important signs that indicate the false lumen include a larger cross sectional area, the cobweb sign and the beak sign. Cobweb sign as slender linear areas of low attenuation specific to the false lumen due to residual ribbons of media that have incompletely sheared away during the dissection process. Beak sign seen at cross-sectional imaging as a wedge of hematoma that creates a space for the propagation of the false lumen. With contrast-enhanced, the true lumen is in continuity with the undisected portion of the aorta and the false lumen may become thrombosed.
Classification
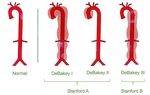
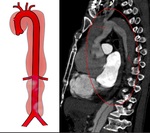
The original system for classification of aortic dissection, the DeBakey system, based of the anatomical and pathological features, has been superseded by the Stanford system, which includes two types based on the need for surgical intervention.
DeBakey (1965)
- Type I: Originates in the ascending aorta, but extends distally and involves the descending aorta.
- Type II: Originates in and is confined to the ascending aorta.
- Type III: Originates in and involves the descending aorta.
Stanford (1970)
- Type A: Involves the ascending aorta irrespective of the site of origin
- Type B: Involves the descending aorta exclusively
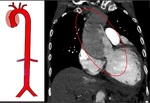
Stanford type A or DeBakey types I and II involves the ascending aorta or the aortic arch. Such dissections account for 70% of cases and typically require urgent surgical intervention. The false lumen courses on the posterior rightward aspect of the aortic arch and anterior leftward aspect of the descending thoracic aorta. An intimal flap defect is noted in the anterior leftward aspect of the true lumen of the ascending aorta. The major aortic arch arch branches are not involved and opacify normally. Within the thoracic aorta, the false lumen is located on the right. The principal risks are rupture, cardiac tamponade and acute aortic valve insufficiency and myocardial infarction. If untreated, type A dissections are associated with a mortality rate of over 50% within 48 hours.
Stanford type B or DeBakey type III involves descending thoracic aorta distal to the left subclavian artery and accounts for 40% of cases. This can often can often be approached conservatively; despite being most often treated medically, due to a more benign prognosis, endovascular stent graft placement can be useful in selected cases, such as suspected rupture, increasing size and ischemic complications.
The report
When writing the reporte, We will used DISSECT, a new mnemomic-based, approach to the evaluation of aortic dissection. It guides clinicians through an asessment of six critical characteristics that facilitate optimal communication of the details that currently influence the selection of a therapeutic option. The six features of aortic dissection include: duration of disease; intimal tear location; size of the dissected aorta; segmental extent of aortic involvement; clinical complications of the dissection, and thrombus within the aortic false lumen. This classification systems. This article was published for European Journal of vascular and endovascular surgery and available online since 2013
The report must be made inmediately, to help with the speedy recovery of the patient and vascular surgeons prefer the Stanford classification.
The final report
-Report findings in unenhanced CT
-Findings the contrast-enhanced CT
- Detect true lumen and false lumen, and report the extension
- Intimal tear location
- Size of the dissected aorta
- Segmental extent of aortic involvement and classify
- Complications of the dissection
- Thrombus or no thrombus
After finishing the report, drink a coffee, take a break and follow the guard...