Acute aortic syndromes (AAS) include several distinct clinical entities that present with similar clinical symptoms; thus, highlighting the importance of imaging as an early assessment tool to help differentiate them.
Imaging modalities include contrast-enhanced computed tomography (CT), magnetic resonance imaging (MRI), and transesophageal echocardiography (TEE). However, the use of CT as the primary imaging modality has increased significantly.
Acute Aortic Syndromes (AAS) can be categorized into 6 different types according to the American College of Cardiology Foundation/American Heart Association.
- Aortic dissections (ADs) - true and false lumen separated by an intimal flap with an entry and re-entry tear (Class I- spontaneous and V- iatrogenic)
- Intramural hematomas (IMHs) - intimal-medial tear leading to hematoma in the wall of the aorta without a re-entry tear (Class II)
- Some develop contrast filled pools, such as ulcer-like projections (ULPs) or intramural blood pools (IBPs)
- Limited intimal tears (LITs) - intimal-medial tears without a dissection flap, separating the true lumen from the false lumen (Class III)
- Penetrating atherosclerotic ulcers (PAUs) - located in the intimal-medial layer of the descending aorta due to underlying atherosclerotic disease (Class IV)
- Rupturing/leaking thoracic aneurysms (RTAs) (VI)
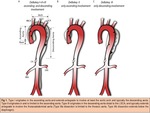
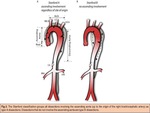
ADs are also classified using the DeBakey (Fig. 1) and Stanford (Fig. 2) classification systems. The Stanford classification is easy to use and effectively guides management because it separates patients into those who benefit from urgent surgical repair (type A) and those who should have medical management unless complications arise or high-risk features are present (type B). However, the Stanford classification system is limited by:
- Its lack of description of the PIT (size, location etc.)
- The direction of propagation of the FL from the PIT
The DeBakey classification system categorizes ADs according to the site of the PIT and distal involvement of the dissection flap. however, it also does not capture the complete spectrum of thoracic ADs.
Neither classification system describes:
- Dissections limited to the arch
- Type B dissections with retrograde extension into the arch
All classification systems omit description of characteristics of the descending aorta that have prognostic impact:
- Presence of aneurysms or pseudoaneurysms
- FL size and shape, partial thrombosis
- Growth over time
- True luminal collapse
The term “non-A-non-B dissection” has been used to describe ADs limited to the arch or those with retrograde propagation to the aortic arch from a site distal to the subclavian artery.
The Stanford classification system classifies IMHs in the same manner as ADs, however, their management is not as well defined.
IMHs have a more variable natural history with some regressing and resolving completely over time, while others progress to dissection, aneurysm, or ulcer-like projections (ULPs). Poor prognostic markers for IMH include:
- Involvement of the ascending aorta
- Aneurysmal dilatation or maximum aortic diameter ³45 mm
- Increased wall thickness ³10 mm
- Presence of ULPs
- Periaortic hemorrhage
- Pleural effusion
ULPs and intramural blood pools (IBPs) both appear as contrast filled collections on CT.
IBPs often do not communicate with the TL or have a very small communication (<2mm)
- Typically located in the descending aorta near the origins of lumbar, intercostal, and bronchial artery branches
- Decrease the probability of IMH resorption
- Carry lower risk of future complications requiring surgical intervention as compared to ULPs
ULPs are new sites of intimal disruption that communicate with the TL (>3 mm)
- Develop over time on follow up imaging
- Difficult to distinguish them from an evolving PIT *especially if the PIT was missed on the baseline CTA
LITs are also classified into Stanford type A (ascending aorta) and B (transverse arch and descending aorta). LITs are often located in the ascending aorta and associated with aortic dilatation. Interestingly, most patients with type B LITs (unlike ADs and IMHs) have aneurysmal aortas.
On CT, an eccentric bulging contour external to the natural aortic boundaries is one clue that a LIT is present and when viewed angiographically, a “mushroom cap” lesion may be visible.
A PAU develops when an ulcerated atheroma erodes the inner arterial wall that may result in a hematoma in the intimomedial layer and are typically accompanied by calcifications and thickening of the aortic wall due to underlying atherosclerotic disease.