The total number of incident reports in the study period between December 2017 to November 2018 hospital-wide was 224 on a total of 18,623 MRI patient scanned – an incidence rate of 1.2%. Wherein in 16,958 (91.06%) were outpatients, 1665 (8.94%) were inpatients, with May having the highest number of logged incidents with 34 (15.18%). Given its availability, 33 (14.73%) were open MRI related incidents. Most of the reports were made by clinical staff (98.66%) and the remaining were by the administration team.
Table 1 gives the breakdown of incidents reported for inpatients and outpatients.
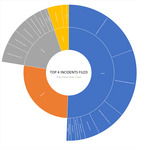
Table 2 shows the top 4 primary incident types with a breakdown of their secondary incident types.
In the 12-listed primary incident types, Table 1 showed that 6 of them were only occurring with outpatients, 1 incident has no patient involvement as it was due to equipment issues, and the 5 left have a combination of inpatient and outpatient encounter for an incident type.
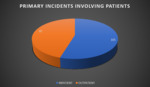
Astonishingly, the outpatient group was not the leading cause of incident reports based on the top 4 incidents filed. According to the data, a prominent feature is that a significantly high number of inpatients faced clinical incidents. Breach of confidentiality and safeguarding had the least reported incidents with 1 and both of which with outpatient involvement only.
There was a significant difference in the number of patients encountered in booking issues; while this number was 43 in outpatients, with inpatients it was a mere 4. The number of patients with MRI safety issues was slightly higher in inpatients than in inpatients. 16 outpatients recorded at this level, whereas the number in outpatient is 10.
The highest percentage of those secondary incidents was Incomplete/inaccurate documentation (34, 38.20%) as a lot of inpatients were coming down for an MRI without identification bands on. The nearly same number of patients, (28, 31.46%) was noted for patient procedure/ pathway delays. 12 (13.48%) were for patient collapse or deterioration due to contrast administration. Surprisingly, a similar close percentage of 14.73% of incidents were under booking issues that were mistakenly scheduled for the conventional scanner when they clearly needed the open MRI system.
In contrast to everyone’s expectations, the number for MRI safety is more comfortable with only 8 with Implant/ device related issues being its highest in secondary incidents, mostly related to lack of information and contraindications. The two least documented was heating related and projectile, with 3 and 1 respectively. Finally, 6 filed for imaging equipment relating directly to the scanning equipment.
In general, it seems that most patients who are inpatients dominate both primary and secondary incidents. By contrast, outpatients have a more comfortable experience over those who were admitted in the hospital, despite the numbers, no real harm has surfaced, nor legal implications faced for inpatients.
The study database included all incident reports without exceptions admitted to the MRI unit in the study period. Due to underreporting, the data may, however, not necessarily represent all adverse outcomes. This study bias may, therefore, have limited the impact of incident reports for the unit’s improvement. Examples of action taken to improve were updating the MRI pre-scan questionnaire slips for a focused management appointment journey for scanxious and corpulent inpatients from ward to us as the inpatients were leading the incidents filed. Future implementation of encouraging incident reporting, education to filling it and a system to follow to standardise the categories to promote it further.