Keywords:
Performed at one institution, Observational, Retrospective, Cancer, Screening, Mammography, Breast
Authors:
T. Presa 1, M. Moreland2, A. Kumar3, J. K. Juttla4; 1London/UK, 2Maidenhead/UK, 3Slough/UK, 4Harrow/UK
DOI:
10.26044/ecr2020/C-04410
Results
Interval cancers (Fig. 5)
One hundred and sixteen women were diagnosed with an interval breast cancer, which represents an average of 2.1 women per 1000 women screened in our unit, which is in line with the NHS Breast Screening Programme (2.2-3.7/1000 women screened) and European rates (0.8-2.1/1000 women screened) (3).
Most of the interval cancers were diagnosed in the first two years after the screening mammogram. Forty-six of the interval cancers were grade 3 IDC or ILC, which represents 40% of all the interval cancers.
Type of interval
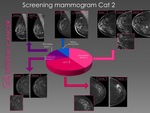
Of the 46 G3 interval cancers, 36 were category 1, 10 were category 2, and none were category 3 (Fig. 6). This could be interpreted that the majority of the G3 interval cancers (90%) were occult or not present in the screening mammogram prior to the diagnosis.
The average time between the screening and the presentation was 17 months (1 to 28 months).
Radiological features
The retrospective analysis of the 10 screening mammograms for the category 2 cancers showed subtle findings. These consisted of 4 asymmetric densities (ASD) (average size 14 mm), 3 clusters of MCC (average size 7 mm), one architectural distortion of 9 mm, one well-defined lesion of 6 mm and one mammogram with diffuse changes (Fig. 7). All the subtle findings were small, with an average of 13 mm, with the exception of two larger asymmetric densities (32 mm and 40 mm).
At the time of the diagnosis, the majority of the lesions presented as an irregular mass or ASD: 25 asymmetric densities, 9 irregular masses, 3 spiculated masses, 3 well-defined lesions, 2 architectural distortions and 4 patients with MCC. The size of the lesions at the time of diagnosis was between 7 mm and 65 mm, with an average size of 31 mm (large lesions).
Prognostic factors
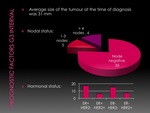
Of the 46 interval cancers (Fig. 8):
- Thirty-five were node-negative, 5 patients had 1–3 positive nodes,and 6 patients had more than 4 positive nodes. Seventy-six percent were stage I at the time of diagnosis.
- Seventeen were ER-positive/HER2-negative, 16 triple-negative, 6 ER-positive/HER2-positive and 7 ER-negative/HER2-positive. The triple-negative cancers represented 32% of the interval cancers and 36% were Luminal A. The proportion of interval cancers that were triple-negative was higher than the percentage of triple negatives diagnosed through the screening programme or symptomatic services (20%)(4).