CT Protocol
A diagnostic protocol of a patient with suspected acute ischemic stroke of the anterior circle, occurring within 6 hours must include a unenhanced CT scan and a multiphase CT-angiography.
In case of unknown onset or onset > 6 hours the diagnostic protocol requires the use of advanced techniques such as perfusion-CT.
The time for the execution of the entire protocol, processing and interpretation of the results must be approximately 15 minutes.
Unenhanced CT
Unenhanced CT allows to:
- recognize stroke mimics like hemorrhagic lesion, neoplasms, AVM, etc. Fig2
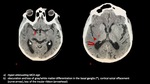
- identify the early sign of ischemia: subtle hypoattenuation, obscuration and loss of gray/white matter differentiation in the basal ganglia, cortical sulcal effacement, loss of the insular ribbon, and hyperattenuation of a large vessel (Hyper-attenuating MCA sign or dot sign in an M2 branch) Fig 3.
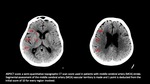
- evaluate the extension of the infarct core through the ASPECT score Fig 4.
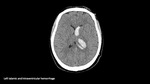
For a correct evaluation of the images, a narrow window is useful.
Multiphase CT-angiography
With multiphase CT-angiography, it is possible to identify the point of occlusion (extra and / or intracranial, anterior or posterior circulation) and to evaluate cerebral collateral circulation.
CT angiography is a thin-section volumetric CT examination performed with a time-optimized bolus (60ml) of nonionic contrast medium (injection rate 4-5 ml / sec). The examination includes three phases, the first arterial, from the aortic arch to the vertex, the second and third consecutive from the skull-base to the vertex.
For a correct evaluation of the images, a narrow window and MPR and MIP reconstructions are useful Fig5.
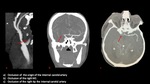
Collateral classification score (Menon et al.)
| Poor |
The delay enhancement is of 3 phases (absence of injection) or 2 phases (appearance in the third phase) with reduced extension compared to the contralateral hemisphere Fig6 |
| Intermediate |
The delay is of 2 phases with equal extension or 1 phase with reduced extension respect to the contralateral hemisphere |
| Good |
The delay is of 1 phase with equal extension or there is no delay respect to the contralateral hemisphere Fig7
|
Perfusion CT
It measures the blood flow along the cerebral microcirculation, and by means of mathematical algorithms it allows to obtain colorimetric maps of the most important cerebral hemodynamic parameters:
- CBF: cerebral blood flow, quantity of blood that passes through a certain volume of tissue in a given time (ml / 100g / min).
- CBV: cerebral blood volume, amount of blood that passes through a certain volume of tissue (ml / 100g)
- MTT: mean transit time, indicates the time it takes for the blood to cross the cerebral capillaries (sec)
- TTP or Tmax: time to peak of the residual function curve, indicates the time that elapses from the beginning to the maximum peak of the curve, reflects the delay of the contrast bolus (sec).
Perfusion CT through the interpretation of maps differentiates the ischemic core from the potentially salvage ischemic penumbra area. In particular, it is possible to calculate the ischemic penumbra using the classic MTT-CBV mismatch in which MTT indicates the all hypoperfused brain tissue with slowed circulation, core+penumbra (threshold values rMTT>145%), while the CBV indicates the hypovolemic brain tissue (threshold values <2ml/100g). Another mismatch that can be calculated is between Tmax(core+penumbra) and CBF(core), which according to recent RCT seems to be more reliable than the classic model Fig8.