RADIOLOGICAL EVALUATION OF EPISTAXIS
Fig. 3 
Fig. 3: Etiologic factors of epistaxis.
IMAGE-BASED REVIEW
A.TRAUMA
Local trauma to the nasal mucosa is a common cause of epistaxis, especially among the pediatric population.
- The most common cause of epistaxis is trauma from digital manipulation.
- Children may present with epistaxis after digital trauma or local irritation from foreign bodies.
- Other sources of local trauma: nasal or facial bone fractures, foreign body insertion, septal perforation from substance abuse, and iatrogenic trauma (from surgery or placement of appliances).
Fig. 4
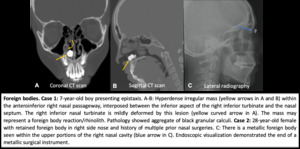
Fig. 4: Foreign bodies.
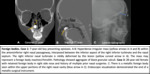
Fig. 5
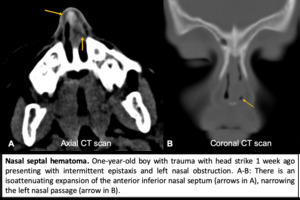
Fig. 5: Nasal septal hematoma.
Fig. 6
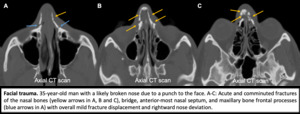
Fig. 6: Facial trauma.
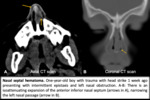
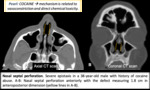
Fig. 7
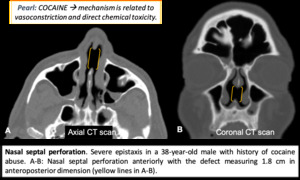
Fig. 7: Nasal septal perforation.
B. VASCULAR ABNORMALITIES AND VASCULAR MALFORMATIONS
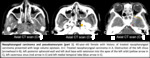
Granulomatosis with polyangiitis (Wegener Granulomatosis):
- C-ANCA+ granulomatous necrotizing vasculitis.
- Osseous/cartilaginous erosion, neoosteogenesis, nodular mucosal thickening, orbital disease, rare intracranial involvement.
- Advanced Wegener granulomatosis --> destructive lesions of the hard palate, sinonasal-oral fistulas, or complete nasal septal destruction.
- Chronic disease --> thickening of the paranasal sinuses walls + reduction of the sinus volume.
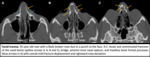
Fig. 8
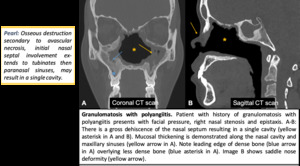
Fig. 8: Granulomatosis with polyangiitis.
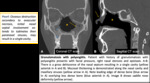
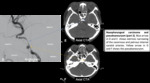
Hereditary hemorrhagic telangiectasia [HHT] (Rendu-Osler-Weber Syndrome):
- Nasal mucosal telangiectasias --> recurrent epistaxis, often refractory to standard techniques.
- Diagnostic criteria: recurrent epistaxis + multiple vascular dilatations (lips, nose…) + arteriovenous malformations or fistulas in the internal organs (lungs, liver…) + first-degree relative with the condition.
Fig. 9
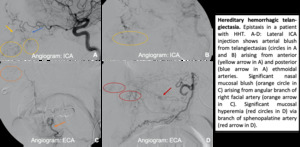
Fig. 9: Hereditary hemorrhagic telangiectasia.
C. NEOPLASTIC
Nasopharynx
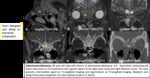
Juvenile angiofibroma (JNA):
- Adolescent males.
- Arises from sphenopalatine foramen, widens pterygopalatine fossa.
- Benign but locally aggressive with skull base invasion.
- Enhancement, vascular flow voids.
Fig. 10
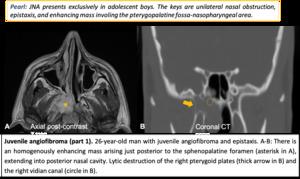
Fig. 10: JNA
Fig. 11
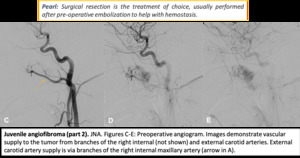
Fig. 11: JNA (part 2).
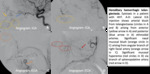
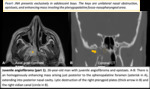
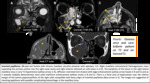
Nasopharyngeal carcinoma:
- WHO classification: I. Keratinizing SCC (EtOH/smoking); II. Non-keratinizing SCC; and III. Undifferentiated carcinoma (most common, EBV infection).
- Late presentation is common. Often present with neck mass.
- Early nodal metastases. Common skull base invasion and perineural spread.
Fig. 12
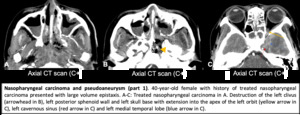
Fig. 12: Nasopharyngeal carcinoma and pseudoaneurysm (part 1).
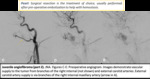
Fig. 13
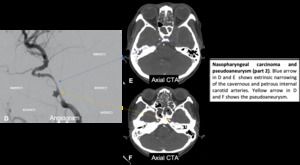
Fig. 13: Nasopharyngeal carcinoma and pseudoaneurysm (part 2).
Sinonasal tumors: WHO Classification (2017, abbreviated
| Carcinomas: squamous cell ca, adenoca, sinonasal undifferentiated ca |
| Teratocarcinosarcoma |
| Papillomas: inverted |
| Salivary gland tumors |
|
Malignant soft tissue tumors: rhabdomyosarcoma, angiosarcoma
Borderline/low grade soft tissue tumors: desmoid
Benign soft tissue tumors: schwannoma
|
| Other tumors: meningioma |
| Hematolymphoid tumors: lymphoma and plasma cells neoplasm |
| Neuroectodermal tumors: esthesioneuroblastoma, melanoma |
- All diagnoses must be confirmed by biopsy.
- Accurate tumor mapping is critical for surgical and/or RT treatment planning.
Inverted papilloma:
- Benign epithelial neoplasm, locally aggressive. Bone expansion and/or erosion.
- Osseous strut indicates site of origin --> must be resected.
- Cerebriform pattern on T2 and enhanced T1.
- May degenerate to squamous cell carcinoma (5%) --> invasion, loss of cerebriform morphology.
Fig. 14
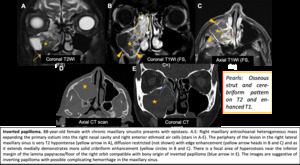
Fig. 14: Inverted papilloma.
Neuroectodermal tumors: Esthesioneuroblastoma (Olfactory Neuroblastoma)
- Arises from olfactory epithelium.
- Nasal cavity mass +/- transcranial extension. Occasional calcification.
- Marginal cysts along intracranial component.
- Hypervascular tumor.
- Express somatostatin receptors.
Fig. 15
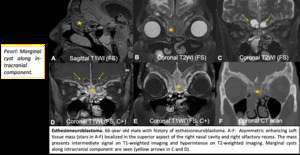
Fig. 15: Esthesioneuroblastoma.
Hematolymphoid tumors: Lymphoma
- Extranodal NK/T cell types. Nasal cavity more often affected than sinuses.
- Lobular, expansile, infiltrative.
- Homogenous, mild ↑ T2 SI. Restricted diffusion.
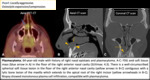
Fig. 16
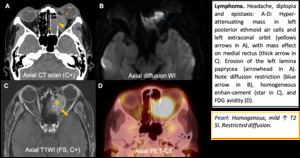
Fig. 16: Lymphoma.
Hematolymphoid tumors: Plasmacytoma
- Younger than patients with MM. Most common presenting symptom ---> pain.
- Bubbly +/- soft tissue mass. Locally aggressive + involvement and destruction of adjacent structures.
- Osteolytic expansion/compression.
- T1: Hypointense with curvilinear low-signal areas. T2: Hypointense or heterogeneous. Mild-moderate diffuse enhancement.
Fig. 17
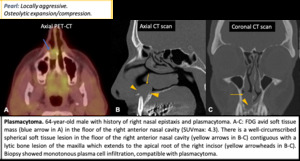
Fig. 17: Plasmocytoma.
Fig. 18
Fig. 18: Summary.