I. Anatomical Review
Bone
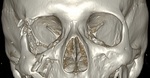
The orbits are symmetrical, pyramid-shaped sockets located anteriorly in the skull. Each is bounded by the periosteum of seven cranial bones with an open, anterolateral base and a posteromedially directed apex.

Fig. 2: Orbital Bones
References: JRCB. Palma de Mallorca / España 2020
The orbit has a rim and four walls that separate it from other cranial structures:
- Roof: frontal bone and lesser wing of the sphenoid; above it are the frontal sinus and anterior cranial fossa. Includes the supraorbital notch (supraorbital vessels and nerve), and anterolaterally the lacrimal gland fossa.
- Lateral wall: formed by the zygomatic bone and greater wing of the sphenoid bones; posterolaterally are the middle cranial fossa and the temporal fossa, as well as the lateral face.
- Floor: zygomatic, maxillary and palatine bones, with the maxillary sinus beneath. The infraorbital vessels and nerve pass through the floor to emerge at the infraorbital foramen below the orbital rim.
- Medial wall: maxillary, lacrimal, ethmoid and sphenoid bones; medially are ehtmoidal cells, the sphenoid sinus and nasal cavity. Anteriorly is the lacrimal sac fossa communicated with the nasal cavity through the nasolacrimal duct.
- Apex: site of the optic foramen and canal (carries the optic nerve, ophthalmic artery), that communicates with the cavernous sinuses. The inferior and superior orbital fissure carry branches of the III, IV, V and VI craneal nerve and vessels.
The Globe
It has three layers:
- Sclera: outermost layer, consisting of collagen-elastic fibers.
- Uvea: intermediate vascular and pigmentary tissue, consisting of the choroid, ciliary body and iris.
- Retina: innermost neurosensory layer.

Fig. 3: Schematic drawing of the globe and supporting structures.
References: JRCB. Palma de Mallorca / España 2020
Supporting Structures
- Tenon’s capsule: or fascia bulbi, its fibers blend anteriorly with the sclera and posteriorly with the sheath of the optic nerve. It forms sleeves over the extrinsic muscles, and expands to form check and suspensory ligaments.
- Orbital septum: an extension of the orbital periosteum that reaches the tarsal plates. It is a protective anatomical barrier and demarcates preseptal and postseptal spaces.
- Muscles: the inferior, medial, lateral and superior rectus muscles insert jointly at the annulus of Zinn to the bony apex, and then at the anterior portion of the globe, delineating the intraconal space. There are also superior and inferior oblique muscles.
- Vessels: the ophthalmic artery is a branch of the internal carotid artery and supplies the optic nerve and retina (central retinal artery).
II. Pathology and CT findings
TRAUMA
Injuries to the orbit present in varied scenarios, from blunt trauma, to penetrating injuries and polytrauma patients, sometimes limiting anamnesis and physical examination. This makes CT an essential tool in evaluation. Orbital lesions can be potentially overlooked if not a clinical priority, or present with unsuspected intracranial findings.
Nonenhanced Computed Tomography (NE-CT) is usually sufficient in the evaluation of orbital trauma.
Foreign bodies should always be evaluated with CT first; MRI is contraindicated in case of metallic foreign objects due to potential displacement and further damage. Plastic or organic matter are not easily identified with CT and can go unnoticed with this technique.

Fig. 5: NE-CT of a 42-year-old man that presented to the ED after a hunting accident with direct impact of a shotgun pellet to the left eye. Sagittal (A) image evidences the metallic pellet lodged in the retrobulbar portion of the optic nerve and the air bubble inside the globe. Hypodense defect in the lens (arrow) in the trajectory of the projectile, and amorphous hyperdense material inside the globe compatible with vitreous hemorrhage (asterisk). (B) Axial image shows metallic pellet impacted at the back of the left globe and an air bubble indicating perforation.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Fractures
There is a broad variety of fractures, with the floor and medial wall being the thinnest and weakest. Indirect signs that should alert the radiologist to search for fractures include:
- Hyperdense content in the paranasal sinuses: can indicate hematic content, especially if there is an air-fluid level.
- Air bubbles in the orbital spaces
- Adjacent soft tissue swelling
- Other associated facial or cranial fractures or injuries

Fig. 4: 3D rendering of a right blow-out orbital fracture involving the lateral wall and floor of the orbit.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Reporting of orbital fractures should include important characteristics that can impact clinical decision-making:
- Blow-out fractures: bone fragments are displaced out of the orbital space, risking entrapment of the rectus muscles due to herniation inferiorly into the maxillary sinus (Fig. 9) or medially into the ethmoidal cells (Fig. 12).
- Blow-in fractures: bone fragments are displaced into the orbital space, decreasing orbital volume with potential compromise of function.
- Measurements: of the bone fragment, defect, and approximate displacement can be useful for surgical planning.
- Associated cranial injuries: other craniofacial fractures or intracranial bleeding (Fig. 7).

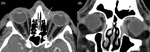
Fig. 6: NE-CT of a 69-year-old woman who suffered an accidental fall. (A) Blow-out fracture of the right orbit, with fragment displacement into the ehtmoidal cells and into the maxillary sinus (arrows). (B) The right globe is grossly-deformed due to rupture, with heterogeneous hyperdense content due to vitreous hemorrhage.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca/ España 2020
Globe Injuries
Open-globe injury or rupture results from perforating trauma (40% associated to foreign bodies, 37% from lacerations), contusions by transmission of increased pressures to the weakest points of the globe (22%), or chemical damage. Initial images can be normal if a lesion is too small to be clinically and radiologically apparent.

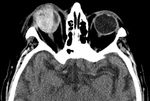
Fig. 11: NE-CT of a 90-year-old man that suffered a fall getting out of bed. (A) Shows the right globe of decreased size and with air bubbles in its interior (asterisk) as signs of globe rupture. (B) Subdural hemorrhage against the right margin of the cerebral falx as an associated intracraneal lesion.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Signs of open-globe injury (Fig. 6, Fig. 11) that should be reported to alert clinicians of this possibility include:
- Gross or subtle globe deformity
- Loss of globe volume or asymmetry with the other eye
- Intraocular gas
- Intraocular or intraconal foreign bodies
- Thickened, hazy or irregular globe margins
- Variations in anterior chamber size (Fig. 13)
- Vitreous hemorrhage (Fig. 8)

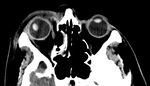
Fig. 13: NE-CT of a 16-year-old male with Ehlers-Danlos syndrome who suffered trauma to the right orbital area. Axial image shows a deformed right globe, with loss of volume and irregular contour compatible with rupture, and an increased anterior chamber indicative of lens subluxation.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Lens dislocation: as a result of penetrating trauma that pushes it into the vitreous cavity, or from blunt trauma with changes in shape and pressure, damaging the zonule and suspensory fibers (Fig. 14).

Fig. 14: NE-CT of a 44-year-old man that presented with trauma to the right eye and a palpebral laceration. Ophthalmologist referred iridodonesis ("dancing" iris) on examination. Axial image shows an abnormally-positioned, verticalized lens, indicating damage to the medial suspensory fibers.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Carotid-cavernous fistula: communication between the carotid circulation and the cavernous sinus can present after orbital trauma. If suspected, intravenous contrast should be administered. CT findings are in relation to increased flow, with congestion (fat stranding, proptosis, thickening of extrinsic muscles) and venous enlargement, as well as abnormal, increased enhancement of the ophthalmic vein similar to that of the carotid circulation (Fig. 15).

Fig. 15: CE-CT of a 37-year-old man that presented to the ED two weeks after trauma to the right orbit. Axial images before (A) and after (B) contrast administration show an enlarged superior ophthalmic vein (asterisk) that has a similar enhancement to that of the internal carotid circulation (C, arrow).
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Orbital compartment syndrome: is usually a clinical diagnosis and a complication of processes that increase intraorbital volume (abscess, oedema, hemorrhage, fracture displacement, et cetera). Signs such as tenting of the globe, stretching of the optic nerve and proptosis should alert to this possibility.

Fig. 16: NE-CT of a 59-year-old man who received a punch to the left eye. Sagittal (A) image shows the blow-out floor fracture (arrow) with dense hematic content in the maxillary sinus (MS) and intraorbital hematoma (asterisk). Axial (B) image evidences proptosis, a stretched optic nerve and "tenting" of the left globe (dashed red line). Such findings should raise suspicion of orbital compartment syndrome.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
INFECTION
Cellulitis
Infections constitute 60% of primary orbital processes, with two thirds of cellulitis secondary to adjoining paranasal sinus pathology, and a fourth due to intraocular foreign bodies. Differing clinical management classifies cellulitis into preseptal or periorbitary when infection extends only to the soft tissues outside of the orbit, and orbital or postseptal when infection spreads beyond the orbital septum.
Contrast-enhanced CT (CE-CT) is useful in the diagnosis of orbital infections, serving to establish extension and allowing definition of abscesses and other complications.

Fig. 17: CT of a 79-year-old woman that presented three weeks after suffering from viral conjunctivitis with swelling and redness over the right eye. Axial images before (A) and after (B) intravenous contrast administration. There are inflammatory changes of the soft tissues (arrow) and linear enhancement in the area of the tarsus (arrowheads). There is no extension beyond the orbital septum (asterisk in the normal intraconal fat).
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Infection can spread progressively from the outermost layers of the skin toward the orbit; CT findings include:
- Inflammatory changes: of preseptal soft tissue, with increased thickness of the soft planes and fat stranding. When findings do not extend beyond the orbital septum, preseptal cellulitis (Fig. 17) is diagnosed in the appropriate clinical context.
- Proptosis: inflammation causes an increase in the volume of orbital contents, pushing the globe outward.
- Fat stranding: due to inflammation and edema.
- Thickening of extraocular muscles: diffuse or adjacent to an abscess, best visualized in the coronal plane.
- Abscess: free fluid might organize into an abscess. Subperiosteal abscesses (Fig. 18, Fig. 19) affect the periosteum of the orbit, usually spreading from adjacent paranasal sinuses.
- Thrombosis: uncontrolled infection can predispose to ophthalmic vein thrombosis or cavernous sinus thrombosis.

Fig. 18: CE-CT of a 9-year old girl that presented with proptosis and diplopia. (A) Axial image shows subperiosteal abscess (asterisk) located against the medial wall of the right orbit, with hypodense center and hyperenhancing rim. Stranding of the intraconal fat (F). Coronal (B) image demonstrates thickening of the inferior (IR) and medial rectus (MR) muscles, likely due to contiguous inflammation in the vicinity of the abscess. There is bilateral maxillary sinus (MS) and ethmoidal cell occupation, consistent with sinus infection as the primary cause of the orbital complications.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Inflammation of the lacrimal sac (dacryocystitis) can be primary or a complication of cellulitis. Findings include enlargement of the lacrimal sac and hyperenhancement after contrast administration (Fig. 20).

Fig. 20: CE-CT of a 68-year-old man who complained of swelling and redness of the periorbital area. (A) There is a rounded hypodense image that corresponds to the subtly-enlarged left lacrimal sac with a hyperenhancing rim (arrow), compatible with dacryocystitis. (B) Dashed red line in the nasolacrimal duct. Notice the soft-tissue density around the lacrimal sac due to inflammatory changes of the surrounding fat.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020
Intraocular infection (endophthalmitis) results from contiguous spread (i.e. orbital cellulitis), penetrating injury or surgical manipulation of the globe. In addition to aforementioned findings, thickening of globe covers, post-contrast enhancement (increased choroidal uptake) and dense content of the vitreous should be reported to alert of this sight-threatening diagnosis (Fig. 21).

Fig. 21: CE-CT of a 68-year-old diabetic man that presented with redness, pain and swelling of the left eye. In addition to proptosis and thickening of the soft planes, there is a linear enhancement of the entire left globe, with ill-defined hyperdense images in its interior that could indicate detritus or bleeding, and stranding in the retrobulbar intraconal fat.
References: Servicio de Radiodiagnóstico, Hospital Universitario Son Llàtzer, Palma de Mallorca / España 2020