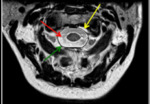
Epidural pathologies
Most spinal lesions present with myelopathy and or radiculopathy due to the tight space between the epidural space and the spinal nerves.
Herniated Disc:
May extend into the epidural space by perforating the intervertebral disc, posterior annulus fibrous and posterior longitudinal ligament.
Appears as a disc extrusion, protrusion or sequestration. The sequestered fragment may migrate laterally, cranially or caudally in the epidural space. [Figure 7]
Epidural infections:
Pyogenic:
They can be primary causes, secondary to trauma, surgical intervention, or as a complication of vertebral osteomyelitis. Secondary hematogenous type which is more encountered in diabetics, alcoholics, cancer patients and those with immunosuppressive conditions or medications (4). Staph aureus as the most common isolated pathogen in both forms. (5).[Figure 8].
Tuberculosis (TB)
TB is common in third world countries, mainly caused by hematogenous spread of mycobacterium TB from a primary lung, lymph node or the GI tract (6). Spinal involvement accounts for 2% of all TB cases. (7)
The disease primarily involves the vertebrae with relative sparing of the disc until late in process. Vertebral lamina erosion, soft tissue epidural abscesses and posterior spinal myositis are the MRI findings. Limb weakness, neuropathy and neural pathology can result from epidural abscesses.
Neoplastic process:
Benign:
Spinal epidural lipomatosis:
This pathology is defined by unencapsulated aggregates of lipoid tissue in the epidural space (8). The condition can be attributed to steroid use, Cushing’s syndrome or idiopathic causes. The dorsal epidural space is where this is most prominent.
It is known for its circumferential mass effect on the dural sac and is diagnosed when epidural fat thickness excess 7mm. (9)
Spinal angiolipoma:
This lesion is usually seen in the posterior epidural space (10). The infiltrative subtype, may destruct vertebral bodies or extend through the neural foramina (11). It will show absence flow void and vague boundaries with fat within the lesion, which will differentiate it from the high flow AVMs and capillary hemangiomas.
Hemangiomas:
Depending on the feeding vessel, these lesions are sub classified into arteriovenous, cavernous, capillary, or venous.
Paravertebral Arteriovenous malformation:
This entity is divided into spinal arteriovenous malformations, spinal cord arteriovenous fistulas, dural arteriovenous fistulas, and arteriovenous malformation that are extradural in location but drain into the epidural veins (these are called paravertebral AVMs/AVFs). (12)
The paraspinal AVF is an uncommon variant of spinal AVFs. They include the intracanalicular and vertebral AVFs and can be due to congenital or traumatic etiology. They are mostly encountered in the cervical spine. Muscular or vertebral tributaries act as feeding vessels and drainage is usually via paravertebral, epidural or intradural veins. [Figure 9]
Neoplastic lesions:
Lymphoma:
Spinal lymphomas can be subcategorized into three types which are paraspinal, vertebral, and epidural. (13) Primary spinal epidural lymphomas are very rare and are usually of the Non Hodgkin type (14). It may occur due to hematogenous spread from unidentified lymphoid tissue or direct spread through the neural foramina from vertebral or paravertebral region.
Metastasis:
Spinal metastasis considered the third most common site following lung and liver (15). It can include the vertebral bodies, epidural space, leptomeninges and spinal cord.
Epidural soft tissue metastatic lesions may cause destruction of the adjacent vertebrae, extension along the posterior longitudinal ligament, intervertebral neural foramen involvement or compression of the dural sac and its contents. [Figure 10].
Miscellaneous
Epidural hematoma:
can be spontaneous (from coagulopathy, therapeutic thrombolysis or vascular anomalies) or post traumatic. Patients present acutely due to cord compression and tend to rapidly progress to quickly irreversible neurologic deficits. The source of bleeding is attributed to valveless epidural venous plexus that predispose these vessels to oscillate with any pressure change. (16) It was described that epidural hematoma of the cervical region is attributed to arterial origin from anastomosis between radicular arteries in the epidural space (17).[ Figure 11,12.]
It is usually variable signal intensity according to the age of the hemorrhagic component. Gradient/ SWI sequences will confirm the presence of blood products. Enhancement is usually peripheral but may be variability.