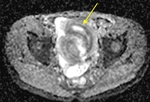
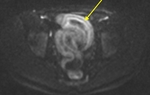
Clinical indications:
- Diagnosis of the inflammatory bowel disease (IBD): luminal, mural and extra-intestinal diagnostic information.
- Crohn’s disease (CD) - the most common clinical indication. For ulcerative colitis, MR scanning is a suitable alternative to colonoscopy.
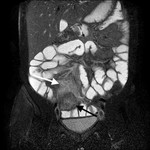
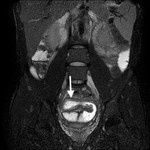
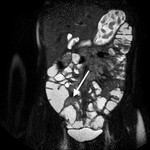
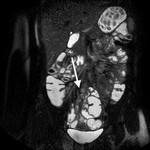
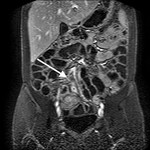
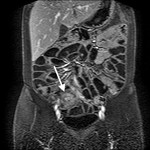
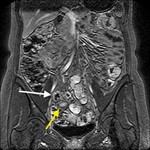
- Assessment of complications ( Table 2 )( Fig. 5 , Fig. 6 , Fig. 7 ).

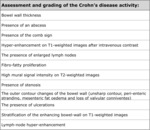
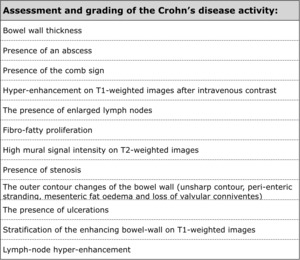
Table 2: Assessment of complications of the Crohn's disease.
- Follow-up of the IBD.
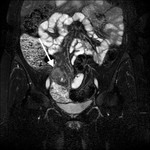
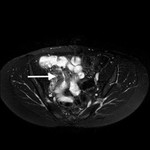
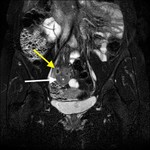
- Small bowel masses ( Table 3 ).

Table 3: Small bowel masses.
- Other small bowel pathologies ( Table 4 ).
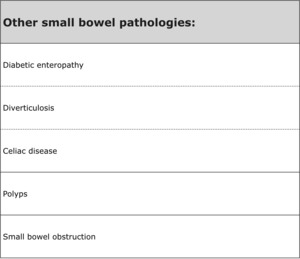
Table 4: Other small bowel pathologies.
MRI protocols and techniques
Patient preparation. Pre-scan fasting time of 4 hours is recommended but can range up to 9 hours. A low residue diet reduces intestinal debris and food material that could be falsely misinterpreted as lesions or filling defects.
Position, in which the patients are scanned:
- Prone - achieves better distension and helps to separate bowel loops, but doesn’t result in better lesion detection.
- Supine - a more comfortable position for the patients (especially relevant in patients with abdominal pain, stomas and cutaneous fistulas).
Intravenous contrast agent:
- Gadolinium-based intravenous contrast agents are mandatory for patients with CD.
- Assessment of mural hyper-enhancement and small-bowel vasculature ( Fig. 8 ).
- Provides improved detection of active inflammation ( Fig. 9 ), evaluate disease activity.
- Helps to detect complications in patients with CD (abscesses and fistulas)( Fig. 10 ).
- Fat-saturated T1-weighted images provide a characterisation of small bowel tumours and detect liver and mesenteric metastases.
- Should not be used in pregnant patients or patients with impaired renal function.
Oral contrast agents are administered to achieve optimal luminal distension ( Table 5 ).
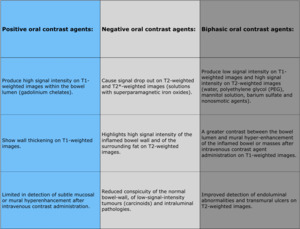
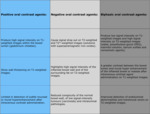
Table 5: Oral contrast agents.
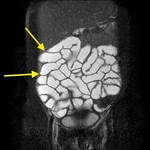
The volume of oral contrast medium - although currently there is no consensus regarding the optimal volume of oral contrast, 1350-1500 ml is considered an adequate volume in the majority of cases. 1350 ml of oral contrast agent can help to achieve good bowel distension( Fig. 11 ), while more than 1500 ml can cause side effects as diarrhoea and abdominal cramping without additional diagnostic value.
The optimal time for the imaging the small bowel is thought to be between 50-60 minutes.
Oral contrast agent should be ingested continuously and steadily over the allocated time to achieve a uniform and consistent distension of the proximal and distal small bowel. Just before the imaging, the patients should be given 200 ml oral contrast agent to outline the stomach and duodenum.
Oral suspension of prokinetic (metoclopramide) is administered with the first portion of the oral contrast material to promote gastric emptying and peristalsis.
Antiperistaltic agents are important to prevent motion artefacts and improve image quality. Antiperistaltic agents (Buscopan, Glucagon) are optimally administered intravenously just before the start of MR examination. A second dose of antiperistaltic agents might be given before intravenous contrast injection.
MR enterography vs. MR enteroclysis
MR enteroclysis:
- Enteric contrast material is administered through a nasojejunal tube.
- Better proximal small bowel distention.
- More stressful procedure.
- Exposes the patient to ionising radiation as the insertion of the nasojejunal tube is performed under fluoroscopy.
MR enterography:
- Contrast agent ingested orally.
MR sequences:
- Essentially the same for both MR enterography and MR enteroclysis with the exception of breath-hold two-dimensional T2-weighted fast-spin echo images being acquired continuously during the administration of the oral contrast agent for MR enteroclysis, but only once for MR enterography. ( Table 6 )
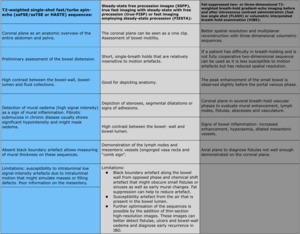
Table 6: MR sequences.
Fat suppressed T2-weighted imaging:
- Axial plane to evaluate mural and mesenteric oedema and intra-abdominal fluid collections.
Diffusion-weighted imaging (DWI):
- Bowel preparation and intravenous contrast are not required.
- Images can be obtained by using a breath-holding single-shot technique or a free-breathing, multiple averaging technique ( Table 7 ).
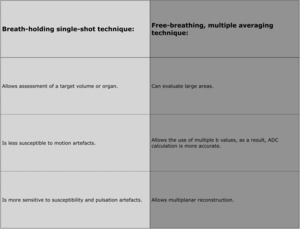
Table 7: Breath-holding single-shot technique vs. free-breathing, multiple averaging technique.
- The use of high b values is recommended to negate the high signal intensity of normal bowel mucosa and shine-through from oral contrast.
- Detection of active inflammation ( Fig. 12 , Fig. 13 ) and abscesses.
- High apparent diffusion coefficient (ADC) values are typically observed in normal bowel segments, moderate in acutely inflamed segments and low in the segments affected by fibrosis. Abscesses are seen as focal areas of diffusion restriction.
- Both intestinal tumours and inflammation have restricted water diffusion and are observed as with high signal intensity on high b values.
Dynamic contrast enhancement:
- Quantitative assessment of tissue perfusion with increased perfusion in inflammation.
- Enhancement is evaluated by calculating objective quantitative and semiquantitative parameters of tissues blood flow on the series of T1-weighted images before, during and after intravenous contrast agent injection.
- Actively inflamed bowel shows different enhancement pattern from the inactive disease. Pathological bowel segments can be identified and differentiation between active or chronic CD can be made.
- A potential tool to monitor the response after treatment.
Cine-MRI:
- Sequences of images are acquired to obtain movies ( Fig. 14 ).
- Postprocessing quantification techniques are used for the assessment of gastrointestinal motility.
- MRI sequence that depicts the bowel wall clearly with a fast acquisition is preferred, like balanced steady-state free procession gradient echo sequence (bFFE).
- Free-breathing protocols are better to measure bowel motility due to longer observation periods but suffer from breathing artefacts.
- Breath-hold protocols are practical for clinical use.
- Decreased bowel motility is observed in inflamed bowel segments compared with non-inflamed segments in CD.
Quantification methods for small bowel motility:
- Visual assessment by a radiologist who grades the contractility (local and global). Simple technique, but susceptible to interpersonal and intrapersonal variations and relatively time-consuming.
- The measurements of the bowel-lumen diameter over time - can be performed manually or semi-automatically.
- The displacement mapping technique allows semi-automated quantitative analysis of global and local small bowel motility by producing easily readable colour maps.
- Gastrointestinal tagging is a fully automated analysis that assesses motility over prolonged periods of time by using tagline applied to the tissue.