Introduction
HT is defined by systolic blood pressure >130mmHg and diastolic blood pressure >80mmHg. It is a very prevalent disease in developed countries (it occurs in approximately 45% of adults) and although it is usually asymptomatic, it is essential to treat it since it represents a cardiovascular risk factor. It can also favor the development of complications such as heart attack, subarachnoid hemorrhage, aortic aneurysm, posterior reversible encephalopathy syndrome...
In most cases the origin is unknown and its management focuses on controlling blood pressure through diet and/or drugs. However, in 10% of patients, the specific and potentially treatable cause can be identified, it is what is known as secondary arterial hypertension. Secondary HT can be of endocrine cause (due to hormonal alterations) or non-endocrine (of the renal origin or due to aortic coarctation). Radiological imaging techniques are very useful in diagnosing the causes of secondary hypertension and its complications, as well as its treatment in some cases by interventional radiology (such as renal vascular stenosis).
Endocrine causes of thyroid origin
Hyperthyroidism
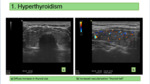
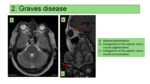
Approximately one-third of patients with hyperthyroidism have hypertension. The diagnosis of this pathology is primarily clinical and analytical, with imaging tests reserved for doubtful cases. It is usually caused by Graves' disease, in which ultrasound (Fig 1) the thyroid is enlarged diffusely and has an increase in vascularization (thyroid hell). When the euthyroid state is reached, the HT resolves. CT and MRI are nonspecific, although in Graves' disease, ocular involvement is very well assessed with MRI, where the increase in spindle-shaped extraocular musculature is observed (respecting tendon portion) as well as increased orbital fat, tear gland and eyelid edema (Fig 2).
Hypothyroidism
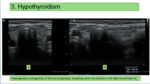
It represents 1% of the causes of hypertension in adults. The most common cause is Hashimoto's thyroiditis, in which the thyroid is enlarged, heterogeneous and has septa. Sometimes hypoechoic micronodules are observed, which is very characteristic of this pathology (Fig 3). Vascularization may be increased, normal or decreased. The euthyroid state achieved after treating these patients resolves the HT in one-third of the patients and decreases it in the rest.
Endocrine causes of adrenal origin
Adrenal hyperplasia
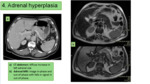
It can be diffuse or nodular and is usually bilateral. When it is diffuse, an enlargement of the entire gland is observed. When it is nodular, it is usually multifocal and in turn, can be divided into macro or micronodular. It may be associated with Cushing's syndrome (in which cortisol increases) or Conn's syndrome (in which aldosterone increases). The signal strength in MRI and attenuation in CT is similar to the normal adrenal gland (Fig 4).
Adenoma
It is the most frequent adrenal lesion and is visualized as an oval or rounded lesion. It is characterized by having intracellular lipids, which is very useful for diagnosis with imaging tests: in MRI there is a signal drop> 20% in out-of-phase sequences, and in CT without contrast, it has a density >10UH. Taking these criteria into account, the specificity for diagnosing adenomas by imaging tests is 92% (Fig 5).
Pheochromocytoma
They account for 5% of the causes of hypertension in the population, and 90% of patients with this disease have hypertension. 90% are located in the adrenal glands, 10% are malignant, 10% bilateral and 10% hereditary.
The presentation on the CT is very variable; homogeneous or heterogeneous, solid or cystic, with or without calcium, may have areas of necrosis, hemorrhage, fibrosis, fatty degeneration ... For this reason, it should be considered as a diagnostic option whenever we find a renal mass in a patient with a compatible clinic. In general, they are round or oval masses of 3-5cm, with soft tissue density. They also have a density >10UH in the CT without contrast and a wash percentage of enhancement <60% (Fig 6,7,8).
In MRI they are hypointense in T1 and hyperintense in T2 and have gadolinium enhancement that can be homogeneous or heterogeneous depending on the solid or cystic component they contain.
Endocrine causes of extra-adrenal origin
Ganglionic: Neuroblastoma, Ganglioneuroblastoma and Ganglioneuroma
These tumors have in common their origin in sympathetic nerve tissue and that can secrete vasoactive amines. They are called neuroblastic tumors and differ according to the degree of cell maturation. The immature tend to be aggressive and occur in children under two years, while the mature occur in older children and tend to behave benignly. Neuroblastoma is the most common extracranial solid neoplasm in children. It is large and heterogeneous, has calcium and areas of necrosis, and can metastasize to liver and bone. It also surrounds vessels without invading them (Fig 9).
Paraganglioma (Extradrenal pheochromocytoma)
It is a form of extra-adrenal pheochromocytoma that can affect the bladder, retroperitoneum, heart, mediastinum, and the carotid and jugular glomus. On CT, it has well-defined edges and is very vascularized, with intense enhancement (Fig 10,11,12).
Neuroendocrine tumors (NETs)
Neuroendocrine tumors are a group of neoplasms heterogeneous for localization characterized by overexpression of somatostatin receptors. The most representative clinical feature is the carcinoid syndrome which is mostly associated with gastrointestinal carcinoid, especially those with hepatic metastases. Carcinoid syndrome is characterized by cutaneous flushing, hypertensive crisis, diarrhea, wheezing, dyspnea and venous telangiectasia (Fig 13,24).
Non-endocrine causes of renal origin
Renal artery stenosis
Renal arterial stenosis accounts for 2% of HT. The most frequent cause is arteriosclerosis, which occurs in older patients and usually affects the proximal third of the renal arteries where it causes focal stenosis. Fibromuscular dysplasia is the second most common cause of renovascular hypertension, typically appears in young people and the 80% are women. The middle third of the artery is usually affected in these cases, which is diffusely and irregularly stenosed. Other less frequent causes are renal artery aneurysm and renal arteriovenous fistula.
Ultrasound, with a sensitivity of 81% and a specificity of 87% for the diagnosis of stenosis >60%, is usually the diagnostic technique initially used for its safety. First, an ultrasound with mode B is performed for the assessment of morphology, size and renal parenchymal pathology. It would then be done in Doppler mode which is considered pathological when the following criteria are met:
- PSV> 180 cm/s at the site of the stenosis
- Nephroaortic index >3,5
- Nephrorrenal index ≥4
- Post stenotic turbulence
- Decreased colour flow concerning the contralateral kidney
- Tardus-parvus type wave
- Acceleration time >0,07s
- Acceleration rate
- Difference in RI between both kidneys, RI>5% being abnormal, stenosis being suspected on the side with lower RI
The angio-CT has a sensitivity of 94% and a specificity of 99% for the diagnosis of stenosis >50%. The proper technique to do would be with bolus at high flows (between 90-150 cc of iodinated intravenous contrast at 3-4 cc/s with bolus tracking) in addition to fine cuts and reconstructions (Fig 14,15).
Angio-RM has a sensitivity of 90% and a specificity of 86% for stenosis >60%. The proper technique to do would be with intravenous contrast (gadolinium) at 0.2 mmol/kg of gadolinium at 1.5–2 ml/s and reconstructions.
Renal parenchymal diseases: Chronic pyelonephritis, AD polycystic kidney disease, acute glomerulonephritis, diabetic nephropathy, kidney cancer
Diseases that affect the renal parenchyma are a common cause of secondary arterial hypertension, in which there is usually no response to antihypertensive treatment. In imaging tests, the findings vary according to the disease, being frequent in all of them (especially in advanced stages) atrophy and thinning of the cortex. Also, some have typical characteristics such as the presence of multiple renal cysts that alter the normal renal morphology of polycystic kidney disease (Fig 16) or the presence of renal scars with a global renal asymmetry of chronic pyelonephritis (Fig 17) or solid mass with necrosis and calcifications in kidney cancer (Fig 18).
Other non-endocrine causes
Aortic coarctation
It accounts for 0.2% of the causes of high blood pressure. The mechanism by which it is produced is unclear, and after the repair of the defect, there are patients in whom HT recurs or persists. The angio-CT allows a rapid diagnosis that indicates the location and severity of the stenosis. The angio-MR also allows to assess the collaterals and quantify the flow through the aorta.
HTA complications
Subarachnoid and intraparenchymal hemorrhage (Fig 19).
Stroke (Fig 20).
Acute aortic syndrome (Fig 21).
Left ventricular hypertrophy and acute myocardial infarction (Fig 22).
Posterior Reversible Encephalopathy Syndrome (Fig 23).