Orbital fractures
Orbital blow-out fracture
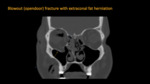
Orbital blow-out fracture (OBF) is a displaced wall fracture with fragments directed away from the orbital cavity, due to an impact of an object larger than the orbital aperture. It may be termed as pure (if the orbital rim is spared) (Fig. 3) or impure (if the orbital rim is involved). The most common orbital wall involved in OBF is the orbital floor followed by the medial orbital wall.
Orbital blowout fractures can be categorized into opendoor (Fig. 4) and trapdoor blowout fractures. The opendoor fracture is usually large, displaced, and frequently comminuted. Intraorbital contents, including the extraocular muscles, can herniate through the defect and cause enophthalmos. Incarceration of soft tissues is rare.
The trapdoor fracture is minimally displaced with a hinged flap of bone that returns to its original position. This results in potential trapping or incarceration of an extraocular muscle or extraconal fat that herniated through the fracture defect (Fig. 5). This mechanism is dependent on bone elasticity that characterizes children’s bones; however, it may be also seen in the adult population. Rapid release of entrapped tissue is vital to prevent permanent abnormal motility caused by to tissue ischemia or scarring.
Orbital blow-in fracture
Orbital blow-in fracture (Fig. 4) occurs when there is a displaced wall fracture with fragments displacing within the orbital cavity. This type of fracture is mostly seen with orbital roof fractures and are usually caused by direct blow to the forehead. The displaced fragments can cause injury to extraocular muscles or extends to the orbital apex, resulting in optic nerve injury. It is generally seen with associated supraorbital rim and frontal sinus fractures. Of note, the orbital roof is part of the anterior cranial fossa and usual complications may include dural tears with subsequent cerebrospinal fluid leaks or brain injuries.
Naso-orbitoethmoid complex fracture
Naso‐orbitoethmoidal (NOE) complex fractures are caused by a high-impact directed to the nose and transmitted posteriorly through the ethmoid bone. It involves the nasal bones, frontal process of maxilla, ethmoidal sinuses, and medial orbital walls. Complications include exophthalmos, telecanthus (due to medial canthal tendon injury), medial rectus muscle entrapment, and cerebrospinal fluid rhinorrhea or meningoencephalocele due to cribriform plate fracture.
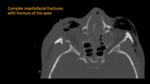
Zygomaticomaxillary complex fracture
Zygomaticomaxillary (ZMC) complex fracture (Fig. 6) is caused by a direct high-impact trauma to the malar eminence of the cheek. It involves the zygomatic arch, lateral orbital wall, the anterior and lateral walls of maxillary sinus, and the orbital floor. It is also called tetrapod fracture due to the concomitant separation of four sutures of zygoma: the zygomaticosphenoid, frontozygomatic, zygomaticomaxillary and zygomaticotemporal sutures, with resultant dissociation of the underlying zygomatic bone from the calvaria. Common complications of ZMC are increased orbital volume with resultant enophthalmos and/or difficulty in mastication because of temporalis muscle impingement.
Orbital Apex fracture
Fracture of the orbital apex (Fig. 7) is usually seen with complex cranio-facial fractures, with involvement of the wing of the sphenoid bone. The fracture line may include the optic canal or superior orbital fissure resulting in injury to traversing nerves and vascular structures.
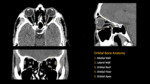
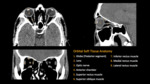
Soft tissue injuries
Anterior Chamber Injury
Anterior chamber injury is usually associated with penetrating trauma and includes corneal laceration. On CT, a decrease in AP diameter of the eye globe signifies a decrease in anterior chamber volume due to injury. It is important to rule out anterior subluxation of the lens as it can mimic corneal laceration, which can be done by determining the position of the lens (Fig. 9).
Lens Injury
The most common cause of lens injury is blunt trauma that cause deformation of the eye and orbit. This deformation results in stretch injury (partial or total) to the zonular fibers, causing dislocation of the lens. Lens dislocation may be anterior or posterior, posterior being more common due to the iris impeding anterior subluxation. Diagnosis is usually made clinically, but CT may help in a clear depiction of the lens position (Fig. 8). It is important to rule out an underlying connective tissue disorder that may cause nontraumatic lens dislocation.
Globe Rupture
Open globe injuries are an important cause of monocular blindness. Diagnosis may be made clinically if intraocular contents are visible during clinical examination. If not, CT may be ordered with a sensitivity of about 75%. CT findings suggesting an open-globe injury include a change in globe contour, volume loss, the “flat tire” sign (Fig. 10), intraocular air, scleral discontinuity, and intraocular foreign bodies5.
Retinal and Choroidal detachment
Retinal detachment occurs when the retinal layer separates from the choroid. Subretinal fluid accumulates between these layers, causing a characteristic V-shaped configuration with the base at the ora serrata and the apex at the optic disk on axial cross-section imaging (Fig. 11). Furhermore, choroidal detachment (Fig. 12) has a biconvex shape, sparing the optic disk and posterior third of the globe and extending anteriorly beyond the ora serrata. Diagnosed with MRI is preferred. Trauma may also cause vitreous hemorrhage (Fig. 13).
Carotid Cavernous Fistula
Carotid cavernous fistulas are most commonly due to trauma (sometimes weeks after event) and result from a direct communication between the cavernous internal carotid artery and the cavernous sinus. It causes an increased sinus pressure with blood flow reversal into the venous tributaries resulting in arterialization. On contrast enhanced CT, a dilated superior ophthalmic vein is seen (Fig. 14). Diagnosis may be confirmed with a CT angiography or conventional angiography.
Optic Nerve Injury
Optic nerve injuries may result from direct or indirect trauma to the orbit that causes nerve or vascular compression. When suspected, a high-resolution CT scan should be ordered to look for apex fractures. If no foreign body is suspected, assessment with MRI should be considered to evaluate for macroscopic optic nerve swelling. Neither CT nor MRI are sensitive enough to pick up early microscopic changes, causing a high number of false negatives when evaluating for optic nerve injuries. Optic nerve injuries may also be associated with retrobulbar hematomas (Fig. 15).
Intraorbital Foreign Body
CT has a high sensitivity for radiopaque foreign bodies, catching metal fragments less than 1mm in size. Most common foreign bodies are made of glass or metal (Fig. 16). MRI may only be used after a metallic foreign body has been absolutely ruled out. If not, permanent blindness may occur. Wood foreign bodies are more challenging to detect due to its hypoattenuation on CT imaging. Opposed to air, wooden foreign bodies can display a geometric margin and may change attenuation over time due to changes in water content5.