Type:
Educational Exhibit
Keywords:
Not applicable, Outcomes, Diagnostic procedure, Ultrasound, MR, CT, Liver, Arteries / Aorta, Anatomy, Vascular
Authors:
A. Asokan1, F. Abubacker Sulaiman2, A. RAJENDRAN3, A. CHELLADURAI1, V. K. Jagan4, A. N. PARIMALAI3, N. Chidambaranathan5; 1CHENNAI/IN, 2Chennai, TN/IN, 3Chennai, TA/IN, 4Coimbatore/IN, 5Chennai, Tamil Nadu/IN
DOI:
10.26044/ecr2020/C-07726
Findings and procedure details
- Assessment of hepatic vascular anatomy in the donor is very important for optimal donor performance after hepatectomy and successful liver transplantation in the recipient. Only 35% of the population has been shown to possess conventional HA, HV and PV anatomy, with variant HA and HV each found in 40% of the population, and variant PV anatomy found in 20%. Therefore, knowledge and awareness of variant hepatic vasculature is critical in liver donor evaluation and surgical planning.
- Computerized tomographic angiography (CTA) helps to clearly delineate the vascular anatomy preoperatively, which would help the surgeon by anticipation of a vascular anomaly.
- Every attempt should be made to carefully dissect and preserve anomalous vessels unless their division or resection is dictated by the need to obtain oncological clearance.
- An international classification describing the principal variations in the vascular anatomy of the liver was proposed by several authors, including Adachi in 1928, Michels in 1966, Hiatt in 1994 and Abdullah in 2006. Despite these studies, there are still some rare hepatic variations which are not found in these classifications.
Hepatic arterial anatomy:
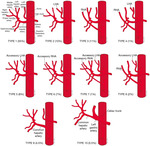
- Conventional hepatic arterial anatomy is defined as a common hepatic artery arising from the celiac axis supplying the whole liver through right and left hepatic arteries, resulting from normal hepatic embryological development. This normal anatomical configuration has been reported in as low as 55% of the population.
- The Michels Classification describes ten anatomic variant categories , but only a subset of these are surgically relevant for donor liver transplant evaluation. Accessory hepatic arteries are variant arteries present in addition to the conventional hepatic arterial anatomy while replaced hepatic arteries are present in place of the conventional hepatic artery anatomy.
- An important variation not covered by the Michels Classification is the origin of the segment IV hepatic artery or middle hepatic artery, a relevant finding for both right and left donor hepatectomy donor candidates.
- These anatomical variants are most relevant in living donors where arterial supply to both the graft and the remnant liver has to be fully maintained. They also are important in deceased donors, to determine the possibility of splitting the liver into two grafts if that was intended, and, in the case of a full liver graft, to determine the arterial reconstruction required to maintain arterial supply. This reconstruction is often performed ex-vivo prior to implanting the graft.
Portal venous anatomy:
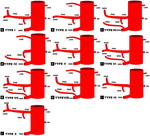
- Conventional PV anatomy (PVA) has been reported in 65–80% of the population, but up to a fifth of donor candidates have been excluded from consideration due to PVA variants.
- Conventional PVA describes the main portal vein (MPV) formed by the confluence of the splenic vein (SV) and superior mesenteric vein (SMV) before it branches into the right portal vein (RPV) and left portal vein (LPV) at the hilum. The RPV then divides into anterior RPV (ARPV) which supplies segments V and VIII, and the posterior RPV (PRPV) which supplies segments VI and VII. The LPV supplies segments II, III and IV, and branches from both the RPV and LPV supply segment I.
- PV anatomical variants is of significant surgical relevance . Additional surgical considerations are the angle of the MPV bifurcation, with too small an angle allowing for possible compromised portal vein supply in the recipient of whole livers as the donor liver hypertrophies and encases both the RPV and LPV, as well as the length of the MPV and its diameter at the anticipated site of anastomosis, both of which also influence surgical technique.
Hepatic venous anatomy:
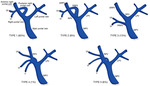
- Normal HV anatomy is seen in up to 70% of the population and describes three hepatic veins; the right hepatic vein (RHV) draining segments V, VI, VII and VIII, the MHV draining segments IV, V and VIII, and the left hepatic vein (LHV) draining segments II and III, with segment I draining directly into the inferior vena cava (IVC).
- Approximately 60% of patients demonstrate common drainage of the LHV and MHV into the IVC. . Pre-operative identification of accessory HVs in the donor is important to minimize excessive bleeding during the transplant hepatectomy, while accurate estimation of their distance from the HV/IVC confluence permits accurate surgical planning as a distance greater than 4 cm often precludes a single anastomosis with the conventional donor HV to the recipient IVC.
- Accessory HVs smaller than 0.3 cm in diameter can be ligated with minimal risk of graft congestion. The most common accessory HV, an accessory inferior RHV draining predominantly segments VI and VII directly into the IVC, can be present in up to 47% of donors, while variant segment VIII drainage via a separate accessory vein is seen in 9%.