We present a series of paediatric cases attending our radiology institution over several years with history of pretibial swelling, not felt to be solely secondary to trauma. Whilst clinical evaluation, ultrasound and plain film alone were sufficient to make a firm diagnosis in some cases, the remainder required further imaging. MRI was useful in narrowing the differential diagnosis and assessing underlying bony involvement, however histological evaluation was required to confirm the diagnosis in many cases.
The majority of lesions were soft tissue in origin; pathologies included benign, inflammatory and malignant conditions.
Benign lesions
1. Foreign Body
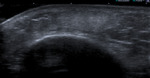
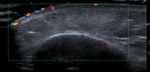
Ultrasound of this lump demonstrated a 2.5cm hyperechoic linear structure which casts posterior acoustic shadowing, typical of a foreign body(Fig. 1Fig. 2). There was associated hypoechoic inflammatory change within the surrounding soft tissues. The ultrasound appearances were diagnostic and no further imaging was required. Although the patient denied a history of trauma, a small twig was removed surgically.
2. Fat necrosis
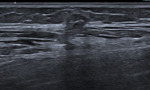
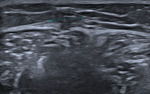
This child was referred with swelling following minor trauma to the shin, which had failed to resolve resulting in parental concern. Ultrasound demonstrated ill-defined increased echogenicity within the subcutaneous fat, typical of fat necrosis(Fig. 3Fig. 4). The patient was reassured and no further imaging was needed. Fat necrosis is usually seen within the subcutaneous tissues, often over osseous prominences and is a frequent sequelae of trauma[1].
3. Muscle herniation
A young teenager presented with bilateral pretibial lumps in similar positions. Ultrasound demonstrated fascial defects with muscle and fatty tissue herniating through(Fig. 5Fig. 6). The patient’s symptoms were exacerbated by standing and the ability to image dynamically with ultrasound proved useful in this instance. Muscle herniation may be caused by fascial weakness or acquired by trauma. The tibialis anterior muscle is most commonly involved in the leg[2].
4. Benign vascular lesion
Plain film demonstrated an area of increased pretibial soft tissue swelling with no periosteal reaction(Fig. 7). Ultrasound demonstrated an ill-defined hypoechoic region with no significant Doppler flow and surrounding oedema within the subcutaneous fat(Fig. 8). This corresponded to an irregular low signal T1w and T2w lesion with significant enhancement and stranding of overlying fat(Fig. 9Fig. 10Fig. 11Fig. 12). No pathological lymphadenopathy was present. Findings were indeterminate, subsequent biopsy confirmed a benign vascular lesion which was then excised.
5. Granuloma Annulare
On Ultrasound the lesion appeared hypoechoic relative to surrounding subcutaneous tissues with indistinct margins in places and no convincing internal vascular flow(Fig. 13Fig. 14). MR demonstrated an ill-defined low T1w and intermediate to low T2w signal lesion which enhanced mildly following contrast (Fig. 15Fig. 16Fig. 17). Imaging findings were inconclusive and a biopsy was required for diagnosis. The lesion gradually reduced in size since the biopsy, but is still under follow-up.
6. Angiomatoid fibrous histiocytoma
This 6 year old presented with a 6 week history of a lump increasing in size. On ultrasound a well-defined hypoechoic lesion was seen within the soft tissues, with low level specks of vascularity(Fig. 18Fig. 19). This was followed up three months later with a repeat ultrasound which demonstrated moderate internal vascularity and small peripheral tails suggesting that it arose from the connective tissue overlying the tibia and pretibial muscles(Fig. 20). There was no associated bony destruction. Histological diagnosis was made following excision biopsy. Close follow is required as local recurrence may occur along with potential low risk of metastatic spread.
7. Lymphatic malformation with fatty overgrowth
This 5 year old boy presented with a lump that had been present since birth. Ultrasound showed a mixed echogenicity soft tissue mass containing cystic areas and small foci of increased vascularity(Fig. 21Fig. 22Fig. 23). The lesion was confined to the subcutaneous tissues and did not involve adjacent muscle. Surgical excision was performed, histology confirmed a lymphatic malformation.
8. Ruptured epidermoid cyst
This teenager presented with a lump slowly increasing in size following possible minor trauma. The ultrasound findings were of a well defined, bi-lobed soft tissue lesion in the subcutaneous tissues(Fig. 24Fig. 25Fig. 26). There was no significant Doppler flow or bony involvement. MR confirmed that the well-defined mass consisted of two adjacent components. This lesion was hyperintense on T2w and intermediate on T1w(Fig. 27 Fig. 28). Due to the indeterminate appearances, a biopsy was required for diagnosis, which showed the lesion to be a ruptured epidermoid cyst. This was subsequently excised surgically.
9. Benign osteochondroma/Exostosis
The patient presented with a lump arising from the anteromedial aspect of the proximal tibia that had increased in size. A non-aggressive lesion characterised by a well-defined, broad-based exostosis, typical of an osteochondroma, was present on the initial radiograph(Fig. 29). A repeat radiograph was performed after 3 years due to an increase in size, which demonstrated exostosis growth with irregularity and ossification at its tip (Fig. 30). This prompted an MR to exclude malignant transformation of the cartilaginous cap - this confirmed a benign lesion with no sinister features(Fig. 31Fig. 32).
10. Osgood Schlatter’s Disease
Osgood Schlatter's is apophysitis of the tibial tuberosity commonly seen in older children and teenagers. It is usually a clinical diagnosis, based on tenderness and swelling related to the tibial tuberosity. Plain film findings include prominent fragmentation of the tuberosity, overlying soft tissue swelling and thickening/inflammation of the patellar tendon(Fig. 33). No further imaging is required.
Malignant lesions
1. Small cell variant of Anaplastic Large Cell Lymphoma
Plain film of this pretibial lump, that had been increasing in size, demonstrated cortical thickening of the anterior tibial diaphysis which contained some ill-defined lucency(Fig. 34). Whilst there was no cortical breach, there was minor overlying soft tissue swelling. Repeat films two weeks later showed more marked periosteal reaction and cortical scalloping medially(Fig. 35). A CT was performed which confirmed a destructive lesion of the tibial diaphyseal cortex and associated soft tissue mass(Fig. 36). MR showed a corresponding low T1w and high fat supressed T2w signal lesion causing cortical erosion of the anteromedial aspect of the tibia, but no underyling marrow oedema(Fig. 37Fig. 38). Ultrasound also demonstrates low echogenicity lesion and cortical scalloping(Fig. 39).
2. Ewing’s Sarcoma
An older teenager presented with increasing pain and swelling around the proximal tibia. Plain film demonstrates a heterogeneous sclerotic appearance to the proximal tibial meta-diaphysis extending to the growth plate, with laminated periosteal reaction(Fig. 40Fig. 41). On MR the lesion was found to have both encased and infiltrated the proximal tibial metadiaphysis(Fig. 42Fig. 43Fig. 44). There was also abnormal signal within popliteus, medial soleus, tibialis anterior and tibialis posterior muscles, consistent with invasion(Fig. 45). Despite amputation, the patient progressed with disease recurrence and lung metastatic spread.
The tibia is the third most common site affected by Ewing’s and is involved in 11% of cases; the most commonly affected sites are the femur and sacrum[3].
3. Ewing’s Sarcoma
This 11 year old presented with pain and swelling over the tibia. Plain film showed cortical destruction and Codman's triangle periosteal reaction involving the mid-diaphysis of the tibia, suggestive of a primary bone tumour(Fig. 46). MR confirmed a tumour arising from and encasing the anteromedial aspect of the tibia(Fig. 47Fig. 48Fig. 49Fig. 50).
There was associated subperiosteal oedema and permeative destruction of the medial tibial cortex. Oedema was identified within the tibial diaphysis medullary cavity, however there were no large medullary tumour deposits. There was no evidence of metastatic spread and the patient was referred to primary bone centre for further management. This case was included to highlight the spectrum of appearances of Ewing’s.