TYPICAL MRI FINDINGS
-
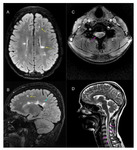
Perivenular T2 hyperintense lesions in typical regions of the CNS - periventricular, juxtacortical U-fibers, infratentorial, spinal cord
“Dawson's finger” sign (Fig. 1)
According to the McDonald criteria, activity of the disease is sometimes evaluated with contrast enhancement on T1WI, although some recent publications suggest that DWI might replace contrast enhanced imaging (CE-MRI) in this regard. [11]
LESS COMMON AND RARE FORMS
-
Baloo concentric sclerosis - a rare and severe monophasic demyelinating disease, appearing as a rounded lesion with alternating layers of high and low signal intensity on MRI, giving it a characteristic onion bulb appearance.
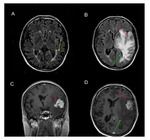
On Fig.2 we demonstrate a female patient who after a 16-year therapy with DMD for RS MS was admitted to our hospital with an acute onset of dysarthria. On CT scan a suspicion of subacute stroke was suggested, however, MRI confirmed a new active baloo concentric lesion. After intensive corticosteroid therapy, her symptoms diminished and her medication has been changed to natalizumab.
Fig.3 shows young female patient. Her first symptom was visual impairment. On MRI an active tumefactive lesion was depicted. After corticotherapy, her symptoms subsided and the lesion diminished. In the differential diagnosis a lymphoma was considered, however laboratory results confirmed CIS and thus she was indicated to DMD therapy.
-
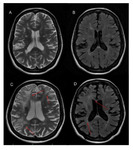
MS in infants - children's form of MS accounts for up to 5% of all MS cases. Pediatric MS is defined as the development of MS before the age of sixteen. MS in children is associated with more frequent and severe relapses. Treatment is the same as in adults. For pediatric patients, higher number of T2 bright lesions in the posterior fossa is typical and gadolinium enhancement is more common than in adults. Lesions are typically more reversible on follow-up imaging in children and suggest a better prognosis [13].
On Fig.4 we present 13-year-old patient suffered from visual impairment for five days. On MRI we found hyperintense lesions in bilateral periventricular white matter. MS, borreliosis, ADEM and neurofibromatosis were considered in the differential diagnosis. Laboratory findings confirmed MS.
COMPLICATIONS OF TREATMENT
- Progressive multifocal leukoencephalopathy (PML) (Fig.5)
Natalizumab treatment is associated with an increased risk of PML due to reactivation of John Cunningham virus (JCV) in MS patients with positivity of JCV antibodies [14]
For follow up in high risk patients we use simplified PML surveillance protocol based on T2 FLAIR and diffusion-weighted imaging, performed every 3 months.
Fig.6 reveals PCNSL and MS in one patient. One of our patients with RR MS developed PCNSL within a year on follow up MRI. There are some reports in literature that natalizumab treatment might be associated with increased risk of PCNSL but there is a lack of evidence in this regard [15].
DIFFERENTIAL DIAGNOSIS ON MRI
Differential diagnosis needs to be carefully considered, as neurosarcoidosis, CADASIL, ADEM, neuromyelitis optica spectrum disorder. MS-specific disease-modifying therapy may lead to an impairment of these conditions [16]. Table 3. lists the most common MS differential diagnosis or mimics.