PSEUDOLESION
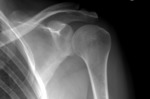
Commonly encountered pseudolesion that may give the impression of true osteolytic or cystic lesions on plain radiographs. (Fig. 1/Fig. 2)

Fig. 1: In the superolateral humeral head is observed a radiolucent round area simulating a lytic lesion.

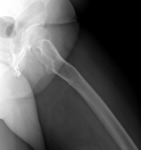
Fig. 2: Radiography shows an anterior lytic defect of the calcaneus due to a decreased trabecular architecture.
FIBROUS DYSPLASIA
Fibrous dysplasia is a benign fibro-osseous pseudotumor in which normal bone is replaced with fibrous tissue permeated with immature heterogeneous trabecular bone. It can be monostotic or polyostotic and affects the immature skeleton.
Radiographic features may include well-defined radiolucent lesions, with a characteristic intralesional ground-glass aspect and narrow zone of transition, frequently with a reactive sclerotic rim forming the so-called “rind sign”. (Fig. 3/Fig. 4)

Fig. 3: We can see a well-defined, metaphyseal, lytic lesion with characteristic “ground glass” aspect on the left proximal femur, with a reactive sclerotic rim, not breaking through the cortical bone.

Fig. 4: This is a patient with fibrous dysplasia involving the proximal femur.
BONE INFARCTION
Asymptomatic until it affects the joints, bone infarction is found upon investigation for adjacent articulation pain. Conventional radiography shows focal or diffuse medullary osteosclerosis. The lesions are mixed, with lytic areas, characterized by medullary bone necrosis and loss of normal bone trabeculae, permeated by areas of sclerosis, leading to a serpiginous sclerotic border. The lesions are restricted to the bone marrow, and do not affect the cortex or induce periosteal reaction. (Fig. 5)

Fig. 5: Radiography of the knee shows a lesion with a mixed, geographical radiological aspect in the medullary bone of the distal femur. The margins of the lesion are sclerotic with areas of localized internal sclerosis. The overlying cortex is uninvolved. On conventional radiography, it can be difficult to differentiate bone infarction from enchondroma and chondrosarcoma.
GORHAM DISEASE
This rare disease can affect almost any site but it tends to affect the proximal limbs, the axial skeleton and often crosses joints. There is a steady and gradual loss of bone from a bone site, which is accompanied by loss of usual function and composition.
On imaging, the lesions are radiolucent and affect the cortex and the cancellous bone. Serial radiographs demonstrate the progressive loss of bone and may lead to complete bone absence. (Fig. 6)

Fig. 6: There is an almost complete disappearance of the 3rd and 4th metacarpals and, to a lesser extent, the 5th metacarpal, by massive osteolysis.
PAGET DISEASE
Radiologic appearance varies as per the stage of the disease. There are three phases described: the lytic, mixed and blastic phases. These correspond to the predominant bone activity occurring at the time. The features include changes in bone density, bone expansion, cortical thickening and coarsening of the trabeculae. In long bones, the disease usually begins at the end of a bone and gradually progresses toward the other end. Paget’s disease mimics both osteolytic and osteoblastic malignancies. The latter, however, usually shows cortical disruption instead of cortical expansion, typical of Paget’s disease. (Fig. 7/Fig. 8)

Fig. 7: Increase of the left iliac bone mineral density with osseous expansion and some osteolytic areas (mixed-phase).

Fig. 8: Radiography shows increased right iliac bone density and expansion with marked sclerosis (sclerotic phase).
OSTEOPOIKILOSIS
It is a hereditary benign condition showing symmetric distribution of radiopaque densities around the joints. This appearance can mimic osteoblastic metastasis, especially when osteopoikilosis is present diffusely throughout the pelvis rather than just around the joints. A uniform size with distribution around the joints, rather than diffusely, is typical of osteopoiquilosis. (Fig. 9/Fig. 10)

Fig. 9: Radiograph shows numerous enostoses of varying sizes and mostly distributed around the femur-tibial joint.

Fig. 10: Pelvis radiograph reveals multiple small sclerotic densities.
MYOSITIS OSSIFICANS
Myositis ossificans is a common tumor-mimicking lesion that occurs as an heterotopic ossification in muscle usually following trauma, although the patient may be unable to recall the precipitating trauma. This commonly occurs in the upper and lower extremities, usually in the lateral muscles. Ossification develops 3‑8 weeks after onset, beginning peripherally and progressing centrally. Initially, myositis ossificans forms faint irregular densities, but with time, a rim of mature lamellar bone and central osteoid matrix can develop. Differentiation from an osteochondroma or osteosarcoma may also be difficult if the area of ossification is adherent to the adjacent bone. (Fig. 11/Fig. 12)

Fig. 11: Radiography shows a well-defined circumferential lesion with calcification in soft tissue. There is a radiolucent cleft "string sign" that separates the lesion from the cortex of the adjacent bone.

Fig. 12: Radiograph demonstrates an oval image with a peripheral rim of calcification, central ossification and a small cleft between the mass and the femur cortex calcification located along muscle.
MELORHEOSTOSIS
Melorheostosis is an uncommon benign bone dysplasia and can involve multiple contiguous bones. On imaging, there is characteristic flowing cortical hyperostosis in a sclerotome distribution, often described as “dripping candle wax.”. Hyperostosis rather than bone destruction is the rule for melorheostosis, which can aid in distinguishing this entity from osteosarcoma. A potentially confusing variable is associated with soft tissue mass formation, particularly near the joints. (Fig. 13/Fig. 14)

Fig. 13: Radiograph demonstrates dense cortical thickening along the tibia that simulates dripping candle wax.

Fig. 14: Radiograph demonstrates dense cortical thickening along the tibia that simulates dripping candle wax.
CRYSTAL DEPOSITION DISEASE
Gouty tophi can present as a palpable lesion with joint pain and can be misdiagnosed as a bone tumor. It is characterized by the deposition of monosodium urate or urate acid crystals in joints and soft tissues.
Radiologists are familiar with the classic radiographic features of calcified tophi and erosion of adjacent bone with overhanging spicules that affect the peripheral joints. However, tophaceous gout can result in masses and bone destruction that mimic malignancy when occurring in unusual locations or isolated and robust. (Fig. 15/Fig. 16)

Fig. 15: Radiographs reveals a tophaceous gout surrounding the first interphalangeal joint. Characteristic findings on radiography in combination with clinical and laboratory data, are diagnostic for these disorders.

Fig. 16: Gout involving the first metatarsal. There are erosive lesions seen in some phalanges and in the 5th metatarsal. The joint space is relatively preserved (usual in gout).
OSTEOMYELITIS
Distinguishing bone infection from bone neoplasm can be difficult, and multiple reports of osteomyelitis resemble tumors. Osteomyelitis can be caused by direct invasion of bone or hematogenous spread of an infecting agent. The infection of bone can also be subdivided based on the clinical course into acute, subacute, and chronic osteomyelitis. All stages have the potential to mimic neoplasm on imaging studies. In acute osteomyelitis, the radiographic findings include areas of aggressive periostitis, cortical destruction, endosteal scalloping, and intracortical tunneling. There may be soft tissue swelling or gas formation. Radiographs may not show appreciable findings in the bone for several days or even weeks after the onset of infection. Subacute or chronic osteomyelitis can cause an intraosseous abscess (Brodie’s abscess), commonly in the metaphysis of tubular bones. (Fig. 17/Fig. 18)

Fig. 17: Radiography shows an osteolytic lesion with bone lesion and soft tissue edema in the distal region of the head of the 5th metatarsal. Acute osteomyelitis may result in geographic moth-eaten or permeative bone destruction and can frequently mimic a malignant bone tumor, such as metastasis, multiple myeloma or Ewing’s sarcoma.

Fig. 18: The radiograph demonstrates an ill-defined osteolytic lesion in the tibia with sharp borders surrounded by extensive reactive sclerosis. On radiographs, Brodie’s abscess appears as single or multilobulated radiolucent lesions with surrounding sclerosis that fades toward the periphery. These lesions can mimic an osteoid osteoma or osteosarcoma.
SEPTIC ARTHRITIS
Septic arthritis is a destructive arthropathy caused by an intra-articular infection that usually is related to severe symptoms such as pain and decreased range of motion. The imaging appearance of inflammatory septic arthritis may mistake it for an intra-articular tumor, particularly if nodular in morphology. (Fig. 19)

Fig. 19: Radiography shows chronic osteomyelitis with a process of septic arthritis. There is marked bone destruction of the humeral head, with loss of its usual morphology.
AMILOIDOSIS
Amyloid lesions of bone are rare but should be considered in the differential diagnosis of skeletal abnormalities in a patient with generalized systemic disease. The more common form seen radiologically has been the involvement of multiple major joints and their para-articular structures by masses of amyloid. These joints can exhibit only soft tissue swelling, but the masses of amyloid may invade the underlying bone, producing multiple small erosions. These have been most often in the hips, shoulders, and elbows. (Fig. 20)

Fig. 20: Radiograph with an amyloid deposition seen in juxta-articular and peritendinous soft tissue calcification.
SYNOVIAL CHONDROMATOSIS
Synovial osteochondromatosis also is known as Reichel syndrome, is a benign monoarticular disorder of uncertain cause characterized by the metaplastic transformation of the synovium with the formation of multiple intrasynovial and intra-articular cartilaginous nodules which may, or may not be calcified or ossified. Imaging findings depend on the stage of the disease and the extent of calcification or ossification of the cartilaginous nodules. In its most distinctive appearance, multiple small, well-defined, juxta-articular nodules of uniform size are observed. (Fig. 21/Fig. 22)

Fig. 21: Lateral radiograph of the knee shows innumerable joint based calcifications compatible with synovial chondromatosis. Femorotibial degenerative changes are also observed.

Fig. 22: In the joint space, there are multiple juxtaposed calcifications.
PARTICLE DISEASE
Particle disease can present as areas of radiolucency surrounding the hardware components. However, unlike in mechanical loosening, the lucent areas do not follow the outline of the prosthesis. The arthroplasty components can incite a macrophage‑mediated granulomatous response, which then stimulates osteoclast activity. Particle disease can mimic osteolytic tumors/infection. However, it can be distinguished by the presence of hardware and the fact that abnormal lucencies are seen on both sides of a joint. (Fig. 23)

Fig. 23: Radiographs shows multiple lucent areas surrounding the prosthesis.