We reviewed the results of all imaging modalities carried out on obstetric patients over a five-year period (2015 – 2019). We searched the image database with the words: pregnant, pregnancy, antenatal, ante natal, postpartum, post partum and post-partum. 45 cases were reviewed of which 12 met inclusion criteria. A breakdown of these can be seen in Table 1 .
The imaging findings were reviewed highlighting learning points and pitfalls in diagnosis.
Diagnoses were mainly gastrointestinal, urinary and gynaecological in nature. This delineates the range of differential diagnosis clinicians face when presented with this high-risk group. Radiological findings are detailed below.
Gastrointestinal Diagnosis:
Appendicitis
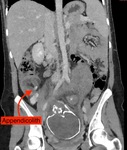
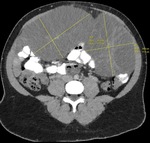
25% of the cases (3/12) were diagnosed with appendicitis. Recognised as the commonest cause of acute abdomen pain during pregnancy, (Augustin et al, 2007) it’s an important differential to consider. The first case underwent a laparoscopic appendectomy but the pregnancy required termination at 8/40 weeks. The second underwent emergency surgery following perforation (see Fig. 1 for CT image demonstrating appendicolith). The third was imaged via MRI, but a delay in surgery lead to small bowel obstruction and resection.
Although CT is the most sensitive and specific modality of imaging abdominal pain (Woodhead et al, 2019), MRI is preferred for the obstetric patient and needs to be considered as first line where resources allow.
Small bowel obstruction
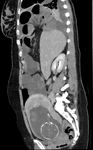
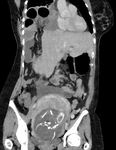
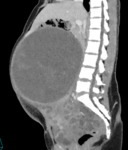
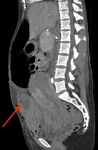
Two cases of small bowel obstruction were reported, one during pregnancy and one post C-Section. Fig. 2 and Fig. 3 show a patient imaged with CT for small bowel obstruction secondary to an incarcerated hernia.
Small bowel obstruction is a rare occurrence during pregnancy (Webster et al, 2015), nevertheless it poses significant risk. Although most commonly secondary to adhesions, hernias are important differentials in need of quick surgical management. Literature suggests urgent MRI when possible, however an individualised multidisciplinary approach is imperative in such situations balancing risks to both mother and foetus (Webster et al, 2015).
Gynaecological Diagnosis:
Red cell degeneration
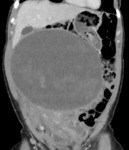
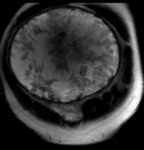
Fibroids are extremely common in women and evidence suggest that these smooth muscle cell tumours may increase in size during the first trimester (Lee et al, 2010). Red cell degeneration results from ischaemia and necrosis of a fibroid; its cause remains under debate. Although rare, it’s an important differential to consider and should not be missed. We include 2 sets of images ( Fig. 4 , Fig. 5 and Fig. 6 - CT and MRI) to aid the identification of red cell degeneration during pregnancy.
Ovarian cysts
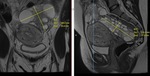
Although common, only 5% are diagnosed during pregnancy (Mukhopadhyay et al, 2016). Usually imaged via US or MRI, they’re an important pathology for radiologists to gain familiarity. The case highlighted was a 17x14x15cm complex cyst arising from the left adnexa (see Fig. 7) diagnosed by US and characterised by MRI at 11/40. The ovarian cyst was deemed neoplastic on imaging. The patient underwent a left oophorectomy at 21/40 and went on to deliver a healthy baby.
Ovarian Hyperstimulation
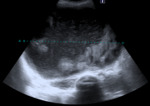
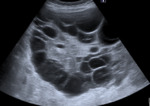
Ovarian hyperstimulation syndrome is associated with induced reproductive technology, specifically the body’s response to beta hCG (human chorionic gonadotrophin). The ovaries appear characteristically cystic and enlarged with signs of associated third space fluid loss secondary to increased ovarian permeability and ovarian neoangiogenesis (Kumar et al, 2011). Images below include a diagnosis ultrasound and CT scan at 5/7 post-delivery by C-section (Fig. 8 , Fig. 9 and Fig. 10). The range of images demonstrate the differences in modalities and image associated qualities.
Urinary
Bladder flap haematoma
A bladder flap haematoma is blood within the vesico-uterine space iatrogenically caused by C-section. They can occur in up to 50% of women undergoing C-section (Rodgers et al, 2012) and imaged via a range of modalities. Although generally considered routine, if above 4cm they become significant. On US they appear as a well circumscribed hyperechoic collection between the bladder and uterus, whilst on CT a hyperattenuating mass is present (Rodgers et al, 2012) (see Fig. 11).
Cardiorespiratory
Pulmonary Embolism secondary to Deep Vein Thrombosis
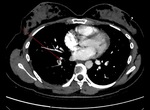
In the developed world, pulmonary embolism (PE) is the leading cause of maternal mortality (Leung et al, 2012). Prompt diagnosis and treatment is imperative to improving this statistic.
The Royal College of Obstetricians and Gynaecologists (RCOG) have published guidelines on thromboembolic disease in pregnancy. Women presenting with symptoms of PE should have both an echocardiogram and chest x-ray first line. If the patient also demonstrates symptoms of deep vein thrombosis (DVT) they should undergo a compression duplex ultrasound and treated with low molecular weight heparin. In those with symptoms of PE without symptoms/signs of DVT a ventilation/perfusion (V/Q) lung scan or computerised tomography pulmonary angiogram (CTPA) should be performed without delay (RCOG, 2015).
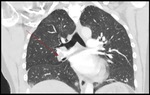
The patient we present demonstrates the complexities of non-obstetric complications. She underwent thrombolysis for a left ileo-femoral DVT and PE (see Fig. 12 and Fig. 13 ) at 8/40. Further to this, complications of a cystic hygroma resulted in termination of the pregnancy at 12/40. During this time, anticoagulation was stopped for a short period which lead to a second left sided DVT. The patient was treated with a DOAC and IVC filter. She has recovered well and is back to baseline.