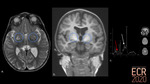
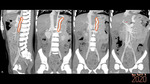
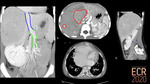
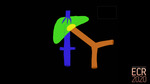
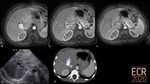
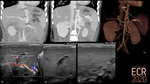
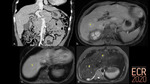
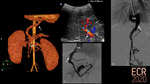
Congenital portosystemic shunts (CPSS) are abnormal communications between the portomesenteric flow and the systemic venous system due to an anatomical anomaly, bypassing the hepatic acini [1]. They can be associated with other malformations: cardiac and heterotaxia being the most common (Fig. 2) [2].
CPSS are a very different condition than acquired portosystemic shunts, that arise due to hypertension in the portosystemic flow (in this case, the portal system drains into the IVC to palliate the negative effects of hypertension in its vascular bed) [2,3].
Classification of CPSS is a controversial topic, with many different classifications arising in the last few years. We will use the classification proposed by Bicêtre (modified by Kanazawa), as it allows the selection of management options and guides the therapeutic approach [4].
The clinical manifestations vary between asymptomatic patients, nonspecific symptoms of liver disease and severe complications. The abnormalities and complications associated with CPSS are described in Table 1 [2] (Fig. 6, Fig. 7, Fig. 8).
Embryological development of the hepatic and portal vasculature
Since CPSS develop by the lack of involution of one or more of the primordial vessels, it is necessary to have a basic understanding of the embryology of the venous system.
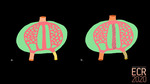
The 4-week embryo presents 3 sets of symmetrically disposed veins: the umbilical veins (UV), the cardinal veins (CV) and the vitelline veins (VV), that open into the sinus venosus (SV). The liver buds will over the next few weeks populate the septum transversum. The developing liver buds disrupt the cranial portion of both the UV and VV, forming the hepatic sinusoids (HS). The hepatic sinusoids tap first into both VV, and by day 32 they link to the UV system (Fig. 3).
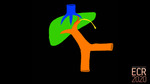
After the 5th week of development, the cranial part of the left VV atrophies, the remaining cranial right VV becomes the cranial part of the IVC (hepatocardiac portion), connected to the hepatic veins. The caudal portions of the VV form anastomoses and become the MPV. The UV system atrophies entirely except for the left UV, which remains the main conduit for blood from the placenta. The portal sinus (formed by vitelline anastomoses) connects the UV and the left portal branch. By week 6, the fetal circulation is established and at week 8 there is a connection between the hepatocardiac portion of the IVC and the portal sinus, a vessel called the ductus venosus (DV), formed by a coalescence of the HS (Fig. 4).
After birth, the UV collapses and forms the ligamentum teres. The DV closes and becomes the ligamentum venosum. The only afferent vein to the liver is the MPV (Fig. 5) [5].
Classification of CPSS:
The CPSS Bicêtre classification is based on the anatomy of shunts [2]:
Type 1: Lower extrahepatic portosystemic shunt (Fig. 9).
CPSS originating from any of the roots of the portal vein, draining to the lower inferior vena cava (IVC), below the renal veins or any such afferent systemic veins (Fig. 10).
Type 2: Upper extrahepatic portosystemic shunt.
Extrahepatic CPSS draining to the upper portion of the IVC, between the renal veins and the hepatic veins. This type can be further subdivided by the kind of connection between the MPV and the IVC:
-
End-to-side-like connection (Fig. 11): The MPV drains directly to the IVC, normally in the proximal or mid-third, end-to-side (like the name suggests). In this case, the right and left portal branches are usually absent (Fig. 12).
-
Side-to-side-like connection (Fig. 13): The MPV drains into the IVC, through a connection at the bifurcation or distal third. At this level, there is often an aneurismatic dilation (Fig. 14). The portal branches, though present, are hypoplastic most of the time.
-
H-like connection: A full abnormal vessel that connects the MPV and the IVC. This is difficult to assess via imaging.
Type 3: Portohepatic shunt (Fig. 15).
Intrahepatic CPSS that connects a portal branch and a hepatic vein (or an afferent vein) (Fig. 16). This type has been linked to hepatic hemangiomas in children [6,7].
Type 4: Persistent patent ductus venosus (DV) (Fig. 17).
The ductus venosus, as previously explained, is an embryological structure that connects the fetal left portal vein and a hepatic vein. If it persists after a month of life, it must be considered pathologic. The spontaneous non-closure of the DV manifests as a large connection arising from the left PV and draining into a hepatic vein (Fig. 18, Fig. 19), unlike the persistent DV secondary to portal hypertension, of normal caliber [6].
Not classifiable: Sometimes, CPSS are too complex to fit in this categorization (Fig. 20).