Type:
Educational Exhibit
Keywords:
Cardiac, CT, MR, Diagnostic procedure, Inflammation, Not applicable
Authors:
P. Simkus1, A. Banišauskaitė1, J. Noreikaite2, V. Buroviené1, M. Gutierrez3, A. Jankauskas1, M. Arzanauskaite2; 1Kaunas/LT, 2Liverpool/UK, 3barcelona/ES
DOI:
10.26044/ecr2020/C-08529
Findings and procedure details
ANATOMY AND FUNCTION
- The pericardium is a double-walled fibrous sac surrounding the heart and consisting of 2 (visceral and parietal) layers. The visceral layer is a serous membrane adherent to epicardium. The parietal pericardium consists of an inner serous and outer fibrocollagenous layers (Fig.1).
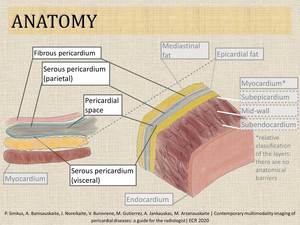
Fig. 1: Anatomy of pericardium.
References: Shared work of the authors
- The main functions of pericardium are to (Fig.2):
- fixate the heart within the thoracic cavity
- lubricate the constantly beating heart
- isolate the heart from the adjacent organs to reduce the spread of infection.
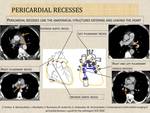
- There is a space between parietal and visceral layers normally containing 15-50ml of serous fluid, which is usually distributed over the interventricular and atrioventricular grooves and is particularly seen within pericardial recesses (Fig.3).
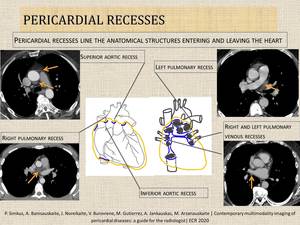
Fig. 3: Pericardial recesses.
References: Shared work of the authors
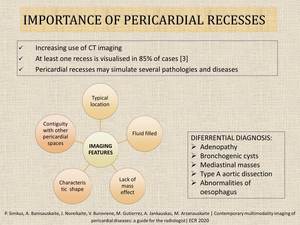
Fig. 4: Importance of pericardial recesses.
References: Shared work of the authors
- Knowledge of pericardial recesses prevents from misinterpretation of various pericardial pathologies (Fig.4).
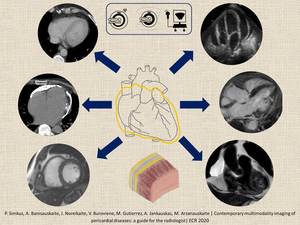
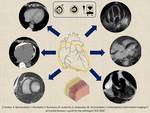
Fig. 5: Contemporary multimodality imaging of pericardial diseases
References: Shared work of the authors
DIAGNOSTIC IMAGING
- 3 imaging modalities (TTE, CT and MRI) are mainly used in daily practice with their different strengths and limitations (Table 1). Nevertheless, CXR and PET has their role in specific clinical situations.
Chest radiography (CXR)
- Has a limited value in diagnosing pericardial pathology. Some radiological signs and features can help to suspect pericardial diseases:
- enlargement of cardiac silhouette and “water bottle” sign suggest a massive pericardial effusion
- malposition or unusual appearance of the heart can be related to pericardial defects.
- pneumopericardium, pericardial calcification and contour of pericardial mass can be seen on chest radiographs
- CXR is useful in detecting concomitant lung, mediastinal, pleural diseases that may be responsible for pericardial manifestations.
Transthoracic echocardiography (TTE)
- Usually is the first-choice imaging modality for suspected pericardial diseases.
- TTE provides comprehensive assessment of both anatomy and physiology and is used to assess for hemodynamic compromise.
- New echocardiographic techniques (cardiac tissue Doppler analysis, strain and strain rate imaging by speckle tracking imaging and three-dimensional (3D) echocardiography) make progress in the assessment of pericardial diseases.
- The diagnostic accuracy of echocardiography can have limitations due to limited windows and suboptimal quality of images.
Computed tomography (CT)
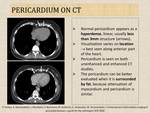
- CT image artefacts related to cardiac motion can be significantly minimized by using ECG-synchronized acquisitions, which improve visualization of the pericardial sinuses and recesses (Fig.6).
- CT has a high spatial resolution and allows to directly visualize pericardial thickening and calcifications.
- CT can play an important role in evaluating specific pericardial lesions, such as cysts, tumours and abscesses.
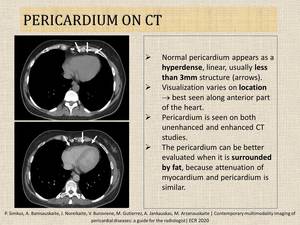
Fig. 6: Normal appearance of pericardium on CT.
References: Radiology, Hospital of Lithuanian University of Health Sciences Kauno klinikos - Kaunas/LT
Cardiovascular magnetic resonance imaging (MRI)
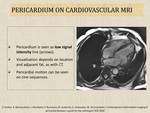
- Provides better anatomical description and superior tissue characterization compared to TTE or CT (Fig.7).
- Cardiovascular MRI allows morphologic evaluation of te cardiac chambers, pericardium, and surrounding mediastinum.
- Regional or global LV and RV function, tissue characterization, pericardial mobility and fusion of pericardial layers can be assessed. Therefore, cardiovascular MRI is suitable to identify pericardial effusions, pericardial inflammation and characterize pericardial masses.
- Haemodynamic compromise in pericardial constriction is seen as diastolic septal flattening on deep inspiration. Inferior vena cava flow can be directly measured by phase contrast imaging, additionally.
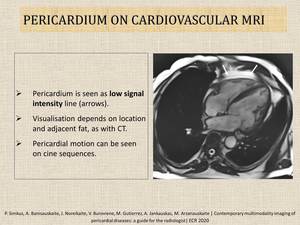
Fig. 7: Normal appearance of pericardium on cardiovascular MRI.
References: Radiology, Hospital of Lithuanian University of Health Sciences Kauno klinikos - Kaunas/LT
Positron emission tomography with CT (PET/CT)
- Detects hypermetabolic activity of pericardial diseases. High uptake of 18F-fluorodeoxyglucose (FDG) reflects malignancy or active inflammation of pericardium.
- In neoplastic cases PET/CT can be used to determine involvement of pericardium, evaluate staging and therapeutic response. In addition, PET/CT helps to identify inflammatory processes of pericardium.
- However, detecting the cause of pericardial disease remains challenging, therefore PET/CT is often used in combination with other tests.
PERICARDIAL DISEASES
Pericardial defects
- A rare congenital abnormality resulting in partial or total absence of pericardium. Partial defect is more common, mostly located on the left side of the heart (Fig.8).
- Pericardial defects sometimes coexist with other congenital defects.
- Diagnosis is complicated because normal pericardium is not always seen. Therefore, indirect signs are beneficial:
- unusual location of the heart structures.
- interposition of lung parenchyma: between aorta and pulmonary artery, between base of the heart and the diaphragm.
Pericardial cyst
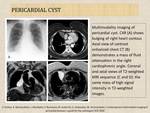
- Usually incidental finding having typical location of right cardiophrenic angle (about 70%).
- A fluid-filled thin-walled benign lesion, without septa or solid parts.
- Cysts show no contrast enhancement with fluid attenuation values on CT and of fluid signal intensity on MRI(Fig.9).
Pericardial effusion
- There is a broad aetiology of pericardial effusions (Table 2).
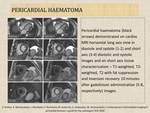
- Pericardial effusion can be readily detected on TTE. CT and MRI can more accurately determine the amount of fluid and specify its origin. MRI determines hemodynamic effect on heart (Fig.10, Fig.11).
Acute pericarditis
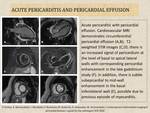
- Often manifests in combination with pericardial effusion (Fig.12).
- TTE: can be normal or show pericardial thickening and/or effusion, with or without features of restriction
- CT – thickening of the pericardium with or without enhancement of the layers
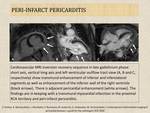
- Cardiovascular MRI – can show thickening of the pericardial layers, increased pericardial signal intensity on T2-weighted images, pericardial enhancement on gadolinium study, with or without haemodynamic compromise; important to rule out adjacent myocarditis (Fig.13).
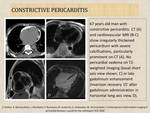
Constrictive pericarditis
- Is a result of inflammatory changes expressed in thickening, calcifications and adhesions of pericardium.
- Abnormal septal motion is characteristic finding in TTE. Exaggerated interventricular dependence is noted, when in inspiration IVS moves towards left ventricle in diastole, as during expiration it goes in opposite direction.
- CT is excellent in visualizing pericardial calcifications.
- Both CT and MRI can show thickened pericardium.
- Diastolic septal flattening can be seen in MRI. Adhesions can be evaluated with tagging sequences (Fig.14, Fig.15).
Pericardial tumours
- Pericardial tumours are very rare. Secondary tumours are more common than primary ones (Table 3).
- CT and in particular cardiovascular MRI are modalities of choice for identification and evaluation of extent of tumours (Fig.16).
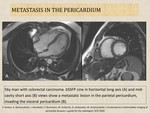
- Differentiation of metastatic lesions is complicated as masses on MRI usually exhibit high signal intensity on T2 and low signal intensity on T1-weighted images. Melanoma has characteristic feature of high signal intensity on T1W images.



![Table 1: Advantages and limitations of imaging modalities [4]. References: Shared work of the authors](https://epos.myesr.org/posterimage/esr/ecr2020/155067/media/880790?maxheight=150&maxwidth=150)