Type:
Educational Exhibit
Keywords:
Haemorrhage, Blood, Embolisation, Arterial access, Fluoroscopy, CT-Angiography, Catheter arteriography, Interventional vascular, Emergency, Arteries / Aorta, Interventional Radiology, Not applicable
Authors:
G. Rafart Martinez1, J. Sampere2, G. A. Tovar2, V. Benito Santamaría2, P. Puyalto De Pablo2, A. García Gámez3; 1Badalona/ES, 2Barcelona/ES, 3Zaragoza/ES
DOI:
10.26044/ecr2020/C-08985
Background
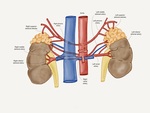
The adrenal gland is irrigated by three main arteries, which are visualized by angiography in 57-92% of cases ( Fig. 1 ):
It usually originates from the ipsilateral inferior phrenic artery and less frequently from the aorta.
It usually originates from the aorta.
It originates from the ipsilateral renal artery in most of the cases.
AAB is usually secondary to spontaneous hemorrhage of adrenal masses or high-energy adrenal trauma, only seen in 1-2% of all visceral bleeding related to closed abdominal trauma. Due to the retroperitoneal location of the adrenal gland, protected by other organs, AAB is a not very prevalent entity so its therapeutic strategy is not well standardized.
AAB is usually identified in CT as a well-defined, heterogeneous and non-enhancing adrenal mass (corresponding to the hematoma), which may be surrounded by trabeculation of the adjacent retroperitoneal fat of the perirenal space, and/or active extravasation after intravenous contrast administration.
By angiography, AAB is recognized as a contrast extravasation after the selective microcatheterization of the adrenal arteries. Once identified, the bleeding can be embolized with different materials such as microcoils, microparticles or sclerosing liquids.