Different imaging methods play an important role in the management of CF patients by presenting a set of imaging findings in the most commonly affected extrapulmonary locations.
Head and neck manifestations:
Almost every patient with CF develops chronic rhinosinusitis and shows radiological evidence of sinus disease.
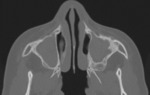
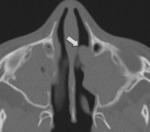
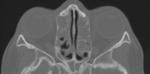
Computed tomography (CT) can depict sinus obstruction secondary to thick impacted mucus, mucocele formation, and bony sclerosis from chronic inflammation ( Fig. 1 ). Nasal polyps are frequently found on physical examination, but imaging can also display signs of this manifestation ( Fig. 2 ).
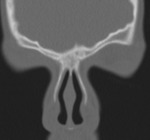
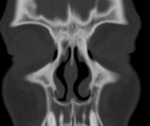
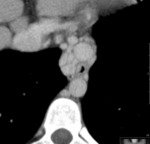
Frontal sinus hypoplasia ( Fig. 3, Fig. 4 ), together with the opacification of the maxillary and ethmoidal sinuses ( Fig. 1, Fig. 5 ), has been proposed as pathognomonic for CF.
Medial displacement of the lateral nasal wall and bilateral uncinate process demineralization are also common findings in this group of patients.
Pancreatic manifestations:
In CF, the most commonly affected abdominal organ is the pancreas. Obstruction of the pancreatic proximal ducts by inspissated and abnormally concentrated pancreatic secretions results in acinar disruption and atrophy, inflammation, fibrosis, fatty replacement, calcification, and cysts formation.
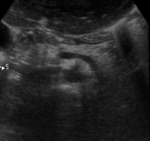
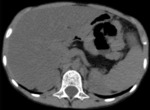
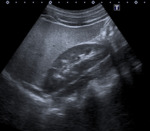
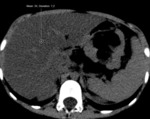
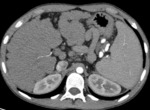
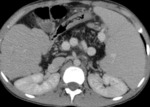
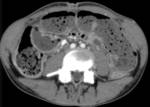
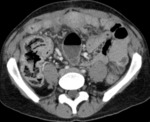
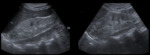
Pancreatic atrophy with complete fatty replacement is the most common finding. Ultrasound (US) shows a small, hyperechogenic pancreas ( Fig. 6 ). In CT studies, the pancreas has a diffuse low attenuation and is difficult to differentiate from the normal retroperitoneal fat ( Fig. 7 ).
Diffuse pancreatic atrophy without fatty replacement may also occur.
Lipomatous pseudohypertrophy, which refers to cases of pancreatic enlargement and complete replacement with fibrofatty tissue, occurs less commonly.
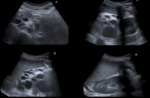
Pancreatic cysts are common in CF patients ( Fig. 8 ). Pancreatic cystosis refers to the presence of macroscopic true epithelium-lined cysts throughout the pancreas and may occur on rare occasions. In severe cases, this can result in the complete cystic replacement of the pancreas.
Hepatobiliary manifestations:
Hepatobiliary involvement in CF can be severe and, after respiratory and transplant complications, hepatic cirrhosis represents the third leading cause of death in this group of patients.
Hepatocytes do not express CFTR and hepatobiliary manifestations are caused by the abnormal expression of this protein in the apical surface of biliary epithelial cells.
Hepatic manifestations in CF include hepatic steatosis, cirrhosis and portal hypertension.
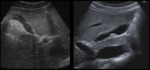
Steatosis is the most common hepatic manifestation in CF, can be focal or diffuse and manifests with the usual US and CT findings of fatty liver ( Fig. 9, Fig. 10 ). In T1-weighted magnetic resonance imaging (MRI) steatosis is depicted as hepatic hyperintensity, suppressed with fat saturation.
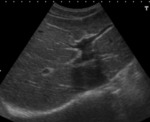
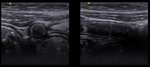
Focal biliary cirrhosis is found in most CF patients and is considered a pathognomonic manifestation of the disease. US shows prominent hyperechoic periportal tissue ( Fig. 11 ) in the setting of focal biliary fibrosis.
Multilobular cirrhosis develops in about 10% ( Fig. 12 ) of CF patients, and in a smaller percentage progresses to portal hypertension and its associated complications (splenomegaly, varices, and ascites) ( Fig. 13, Fig. 14 ). Few cases of CF associated hepatocellular carcinoma have been described thus far.
Gallbladder and bile ducts abnormalities are also common in CF.
The gallbladder may be absent or it may be very small - "microgallbladder" - ( Fig. 15). Pancreatic insufficiency and fat malabsorption favor the formation of gallstones, and about one-quarter of CF patients develop gallstones and/or sludge ( Fig. 16 ).
Bile ducts abnormalities such as dilatation, beading, strictures, and the presence of calculi, can be found in CF patients.
Gastrointestinal tract:
Most CF patients have gastrointestinal (GI) complications. This group of manifestations includes meconium ileus in the newborn, distal ileal obstruction syndrome (DIOS), constipation, appendiceal involvement, intussusception, colonic wall changes, and gastroesophageal reflux. As survival rates improve, gastrointestinal malignancies are becoming a concern in CF patients.
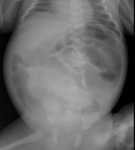
Meconium ileus can be the first manifestation of CF, results from the obstruction of the terminal ileum by viscid meconium. Abdominal plain films are usually the imaging modality of choice to evaluate this complication ( Fig. 17 ) and can reveal dilated bowel loops with or without air-fluid levels, absence of gas in the rectum, and a “soap-bubble” appearance from meconium mixed with swallowed air in the distal small intestine. A "microcolon" distal to the obstruction can be depicted with contrast enemas ( Fig. 18 ).
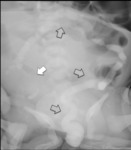
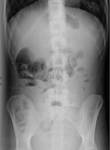
DIOS, sometimes described as the "meconium ileus equivalent" in adults, is relatively common in CF and results from the accumulation of viscid fecal material in the distal small bowel. Abdominal plain films can reveal dilated bowel loops with or without air-fluid levels, and a soft tissue mass in the right lower quadrant ( Fig. 19 ). CT is more accurate in evaluating the obstruction ( Fig. 20 ) and the potential complications associated with this condition such as ischemia or perforation.
Constipation is also common in CF patients, and it can be difficult to differentiate it from DIOS. Unlike DIOS, in constipation fecal material is distributed throughout the bowel.
Appendix enlargement in the absence of appendicitis is not unusual in CF patients ( Fig. 21 ). This results from mucoid impaction causing distention of the appendix, therefore size is not a reliable feature to evaluate appendicitis in these patients.
CF patients are at an increased risk for intussusception. In this group, intussusception is usually ileocolic and the presumed lead points include inspissated stool, lymphoid tissue or an abnormally enlarged appendix. Imaging findings are the same as in other cases of intussusception.
Proximal colonic wall thickening can occur in CF patients without colonic disease. Colonic wall redundancy with a wrinkle appearance has also been described ( Fig. 22 ).
Despite the common use of multiple courses of antibiotics and the elevated rates of Clostridium difficile colonization, pseudomembranous colitis is rare in CF patients.
Increased intraabdominal pressure due to respiratory complications, esophageal dysmotility and the chronic use of some drugs favor the development of gastroesophageal reflux in CF patients. Barium studies can help evaluate this complication.
Miscellaneous:
Renal complications in CF, although infrequent, encompasses both renal stone disease and renal parenchymal disease. The former includes nephrocalcinosis and nephrolithiasis. Renal parenchymal disease includes amyloidosis ( Fig. 23 ), diabetic nephropathy, glomerulosclerosis, and medication toxicity in post-transplant patients.
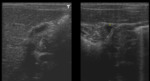
In CF male patients that reach adulthood, infertility is an important issue. Congenital bilateral absence of the vas deferens or complete involution of the vas deferens occurs in most men with CF. Scrotal US and/or MRI can be useful in evaluating this complication.
Poor nutritional status, vitamin D deficiency, elevated inflammatory cytokines, and glucocorticoid therapy, all favor the early development of bone disease in CF patients. Osteoporosis and bone fractures are of concern in CF.