What radiologists need to know?
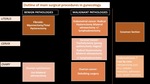
First of all, they need to know the different surgical procedures implemented for gynecological pathologies, to predict most frequent possible complications, both in acute and chronic phase (Fig. 1).
Complications often occur after interventions for malignant pathologies, in which, in addition to bilateral hysteroannectectomy, are often performed:
-lymphadenectomy;
-resection of peritoneal nodules/bowel resection (more often in ovarian cancer);
-resection of bladder or ureteres (more often in cervical cancer).
The frequency of complications also increases if the patient has undergone neoadjuvant chemotherapy and/or radiation therapy.
Secondly, radiologists, on the basis of the individual patient's signs and symptoms, may decide which is the best procedure for a correct diagnosis (Fig. 2).
The most appropriate imaging method should be chosen on a case by case basis. Among imaging modalities, conventional radiography and ultrasound may provide limited information. Computed Tomography (CT) and Magnetic Resonance (MR), on the other hand, allow for better comprehension of the causes of patient’s signs and symptoms.
CT is certainly the best method in emergency phase, for its speed of execution, its ability to demonstrate (already in basal conditions) the presence of collections, hemorrhages or bowel obstruction; after the administration of contrast medium it provides a precise study of arterial and venous vessels, for the search of source of bleeding.
When to choose MR?
When, in an urgent phase, may be useful a detailed study of the pelvic organs, or when it is preferable not to subject the patient to ionizing radiation (for example in case of young women of childbearing age).
Once chosen between CT and MR, radiologists must choose the best diagnostic protocol based on the case, as shown schematically in Fig. 3 (CT protocol) and Fig. 4 (MR protocol).