Type:
Educational Exhibit
Keywords:
Not applicable, Metastases, Diverticula, Cancer, Biopsy, CT, Small bowel, Gastrointestinal tract, GI Tract
Authors:
M. Badulescu1, M. D. COMSA2; 1Cluj Napoca/RO, 2Cluj Napoca, Cl/RO
DOI:
10.26044/ecr2020/C-09946
Findings and procedure details
Duodenal lesions are primarily diagnosed using videoendoscopy and biopsy, but sometimes this is not enough or there are duodenal conditions that are incidentally discovered with computed tomography.
Computed tomography (CT) and magnetic resonance (MR) imaging technology improved other the time their diagnostic capabilities. Therefore, nowadays CT and MRI are used efficiently to evaluate the intraluminal content, duodenal wall, and extraduodenal space. The duodenal masses are completely assessed when CT is associated with optimal duodenal distention and intravenous administration of iodinated contrast material [1,2].
Computed tomography findings of the duodenal masses
Malignant duodenal masses
Neuroendocrine neoplasms (NEN)
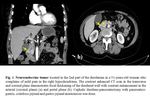
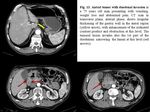
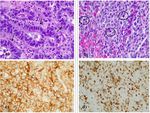
- Intraluminal polyps and mural masses with early arterial enhancement at CT, with delayed washout. ( Fig. 1 )
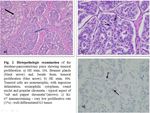
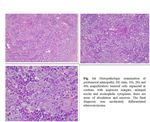
- Histopathologic examination reveals the presence of dense-core granules ultrastructurally and the expression of certain marker proteins (chromogranin, synaptophysin, and neuron-specific enolase); additionally, some cell-type-specific hormonal products (peptide hormones and amines) are expressed. Also, Ki-67 is very important giving the rate of proliferation ( Fig. 2) [9,10].
Gastrointestinal stromal tumors (GISTs)
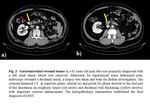
- Typically a well defined and exophytic mass of soft tissue density with heterogeneous enhancement and a clear delineation from the mesentery ( Fig. 3 ); it may ulcerate or have central necrosis.
- Obstruction is rare because GISTs do not involve the circumferential bowel wall, in contrast to adenocarcinoma [10].
Adenocarcinoma
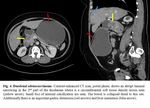
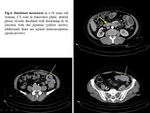
- Focal unilocular, circumferential mass with shouldering of the margins and obstruction ( Fig. 4 ).
- In some cases, adenocarcinoma presents as an intraluminal polypoid mass and causes intussusception.
- Frequently, adenocarcinoma can ulcerate.
- A specific characteristic of adenocarcinoma is the extraluminal infiltration as fatstranding.
- Adenocarcinoma shows moderate and late enhancement.
- It can invade the retroperitoneal fat planes, pancreatic and biliary duct [2,3,5].
Duodenal lymphoma
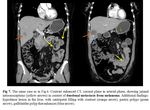
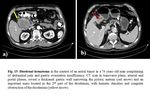
- Thick walled infiltrating mass with aneurysmal dilatation without obstruction (Fig. 5).
- The aneurysmal dilatation is caused by the destruction of the bowel wall.
- Duodenal lymphoma and adenocarcinoma can have similar appearances, but specific for lymphoma are bulky mesenteric or retroperitoneal lymphadenopathy and splenomegaly, while for adonocarcinoma the extraluminal infiltration is pathognomonic [2].
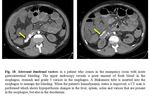
Duodenal metastasis
- Duodenal metastases predominantly manifest as gastrointestinal bleeding and don’t have specific imaging findings.
- Metastases from melanoma are single or multiple intraluminal masses that usually are hyperenhancing after intravenous administration of contrast material on CT and MR imaging [2,7]. They can cause intussusceptions, as is shown in Fig. 6 Fig. 7.
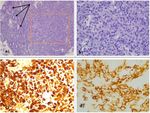
- Histopathologic examination with immunohistochemical staining can establish the final diagnosis, mainly because tumoral cells are positive for S100 and Melan A (Fig. 8).
Benign duodenal masses
Duodenal polyps
- Whether they are adenomatous or hamartomatous, they are well-defined, homogeneous sessile or pedunculated soft-tissue masses, measuring up to 2 cm, with mild enhancement after intravenous administration of contrast material [2].
Duodenal lipomas
- Round or oval, homogeneous lesions, with fat densities and without enhancement of the contrast material [2]. (Fig. 9)
Duodenal diverticulum
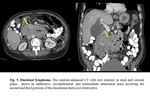
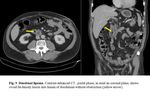
- Sacular outpouching duodenal mass, with thin, regular edges that may contain air, air-fluid level, fluid, contrast material, or debris ( Fig. 10 ).
- If it’s located peri-ampullary it may mimic pseudocyst or tumor.
- In case of duodenal diverticulitis, CT shows a duodenal wall thickening and infiltration of periduodenal fat [2].
Duodenal duplication cyst
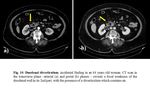
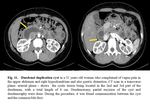
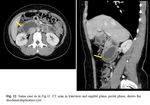
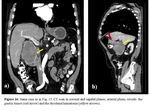
- Smoothly rounded, fluid-filled cyst or tubular structure with thin, slightly enhancing walls in or adjacent to the wall of the part of the alimentary tract ( Fig. 11, Fig. 12 )
- Cystic wall calcifications may occur rarely.
- The duplications usually do not communicate with the duodenal lumen, but can communicate with the bile duct [7, 11].
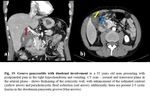
Possible duodenal involvement in other pathologies and the CT findings
- Pancreatic pathology consisted of tumors or chronical conditions, such as groove pancreatitis (Fig. 19), may involve also the duodenum.