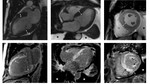
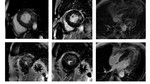
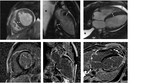
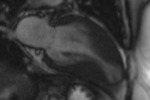
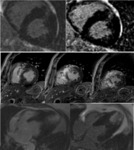
CMR with LGE was performed with 1.5 T systems. Different causes of LVH are illustrated with the representative cases from our database: sarcomeric HCM (n=65), amyloidosis (n=5), Fabry disease (n=15), hypertensive heart disease (n=10), Dannon disease (n=2).
1. HCM is a primary genetically heterogeneous non-inflammatory myocardial lesion, which is manifested by LVH (more than 15 mm) in the absence of objective reasons for this [4].
Cardiomyocyte apoptosis, microvascular ischemia and fibroblast proliferation leading to myocardial fibrosis may be a substrate for the development of diastolic disfunction and life-threatening arrhythmias such as ventricular tachycardia and ventricular fibrillation, which in turn underlie the mechanism of SCD [5].
There are several morphological types of HCM:
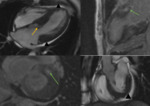
- the most common is asymmetric LVH, diffuse and segmental variants are possible; the anterior part of the LV is most often involved (Fig. 2);
- apical (difficult to diagnose with echocardiography) (Fig. 3);
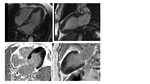
- symmetrical (Fig. 4).
The latter two forms occur in about 1% of patients.
Depending on the presence or absence of systolic pressure gradient in the LV cavity, HCM is divided into obstructive and non-obstructive. The severity of obstruction can vary from minor to severe, 50 mm Hg is recognized as an obstruction edge.
LVOT obstruction leads to complex disorders of intracardiac hemodynamics, including an increase in systolic pressure in the ventricular cavity, an elongation of the relaxation period, an increase in diastolic pressure in the LV, mitral regurgitation, myocardial ischemia, and a decrease in cardiac output. Furthermore, the left atrium (LA) overload and its dilatation due to the mitral regurgitation are associated with increased risk of LA fibrillation and SCD. The gradient between the proximal and distal parts of the chamber predisposes to the formation of LV apex aneurysm, which is revealed in 2% of patients with HCM (Fig. 5).
HCM is the most common cause of SCD in young people, including professional athletes. HCM is one of the leading causes of chronic heart failure at young age, acute cerebral circulation disorders, atrial fibrillation. 3.5% of patients with HCM may develop severe systolic dysfunction which determines the extremely unfavorable prognosis of these patients (11% of mortality during the year) [6].
CMR should be considered for patients with HCM as a baseline study method [7].
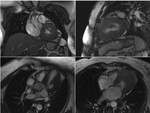
Different types of non-ischemic contrast enhancement in HCM patients (focal, diffuse, "burned-out apex") are demonstrated (Fig. 6).
2. Arterial hypertension
The prevalence of hypertension among individuals with LVH is 98.5%. Most patients with untreated hypertension have normal LV wall mass and thickness, while hypertensive concentric hypertrophy occurs in a minority. The positive aspects of this compensatory mechanism are outweighed by the undesirable effects of increasing LV myocardial mass — a decrease in myocardial oxygen consumption, coronary reserve decrease, myocardial fibrosis, an increase in the risk of heart failure due to systolic and diastolic dysfunction, arrhythmogenesis. All of the above can lead to an increase in mortality.
Patients with arterial hypertension usually have mild non-specific foci of LGE at the junction points of intraventricular septum (Fig. 7).
3. Heart amyloidosis
Heart amyloidosis is a manifestation of a group of diseases characterized by extracellular accumulation of insoluble fibrillar amyloid protein. Systemic amyloidosis with accumulation of light chains of immunoglobulins (AL-form) is the most common form involving the heart. Clinical manifestations include increasing shortness of breath, swelling up to ascites, chest pain, weight loss, syncope, peripheral and autonomic neuropathy. SCD is common due to electromechanical dissociation [8], ventricular arrhythmias are rare.
Morphologically, heart amyloidosis is characterized by amyloid that leads to thickening of the ventricular walls without dilation, diastolic dysfunction, development of restrictive cardiomyopathy [9, 10].
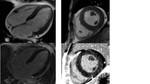
CMR with LGE is an accurate method for detecting amyloidosis. Circular subendocardial enhancement and early wash-out of contrast material are characteristic. The most clinically and prognostically unfavorable variants are transmural or subendocardial contrast accumulation (Fig. 8).
4. Fabry disease (FD)
FD belongs to the group of lysosomal accumulation diseases. In addition to the classic intracellular accumulation of sphingolipids, there is also interstitial accumulation, the result of which is myocardial fibrosis. It makes a significant contribution to the pathogenesis of FD, causing angina clinic and heart perfusion defects even with complete epicardial revascularization [11].
FD can be attributed to the small vessels disease. Patients have a high risk of transient ischemic attacks and strokes at young age.
Heart disease is the leading cause of death in patients with FD. A characteristic feature of heart disease is progressing concentric LVH. LVOT obstruction and systolic disfunction are not typical. Fibrosis is often observed in the later stages; firstly, it is concentrated in the middle layers of the myocardium of the posterolateral part of the heart, then it spreads transmurally. Atrial and ventricular arrhythmias and conduction disorders often develop.
The "gold standard" method for diagnosis of myocardial fibrosis in FD is CMR with LGE. Assessment of myocardial fibrosis is important for disease staging and monitoring of therapeutic effect (Fig. 9).
5. Danon disease (DD)
DD is a rare severe multisystem disorder clinically characterized by LVH, skeletal myopathy and mental retardation in male patients, and by a milder phenotype in female patients. The onset of the disease always manifests in the heart first. The disease has a rapid progression toward end-stage heart failure, and unless heart transplantation is performed, death usually occurs in males before the age of 30 years, whereas in females death occurs in the fourth or fifth decade.
Heart block, atrial fibrillation, flutter and life-threatening ventricular arrhythmias are frequent (up to 60% of patients).
An early diagnosis plays a fundamental role in the primary prevention of SCD, such as ICD implantation [12].
In patients with DD CMR is perfect diagnostic feature, subendocardial areas of enhancement are usually seen (Fig. 10).