We included 40 patients aged from 29 to 90 years old (65.8 medium age), one of which was included twice due to recurrent leaking (n=41 in total). The population consisted of 72.5% males and 27.5% females.
There were CT signs of anastomotic leak in 10 of 41(24.3%) patients.
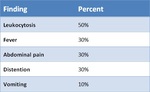
3(30%) of those patients with anastomotic leak were completely asymptomatic. 70% of patients with anastomotic leak presented one or several of the clinical and analytical parameters analyzed(Table 2). Leukocytosis was present in 50% of the patients and was the most common finding, followed by fever (30%), abdominal pain (30%), distention (30%) and vomiting (10%).
Emergent reintervention was needed in 9 of the patients with anastomotic leak (90%). In 4 cases, minimally invasive vacuum-assisted closure (VAC) treatment could be performed(Fig. 1)(Fig. 2)5. Another 4 patients underwent laparoscopic anastomosis repair. One of the patients underwent abdomino-perineal extirpation due to recurrent leak. On the resting patient, a conservative strategy with antibiotic treatment was adopted.
In regarding of early complications, 4 out of 10(40%) anastomotic leaks were already complicated with perianastomotic collections. One of them associated paralytic ileus and another case presented a postsurgical hematoma. There were no cases with peritonitis in this early postoperative phase.
About the CT findings, the highest certainty of diagnosis of anastomotic leak was made due to endorectal contrast agent leak in 9 of the 10 patients(S90%, E96.8%) (Fig. 3)(Fig. 4)(Fig. 5). There was an isolated case of endorectal contrast leak with no leaking found in following surgery. A clear bowel mural defect was identified in the resting anastomotic leak case (S10% E100%).
There was an isolated of a non-conclusive CT scan, with findings of anastomotic leak on the following surgical procedure performed due to clinical worsening.
Peri-anastomotic air bubbles were the most useful finding for probable anastomotic leak diagnosis, with S90% and E86.7%.
Sensitivity and specificity values for the findings studied are shown in Table 3.
The leaking anastomosis were 70% colorectal, 20% coloanal and 10% ileorectal.
Alternative diagnosis were made in 19 of the remaining 30 patients (63.3%) with prompt PCR and procalcitonin raise. Paralytic ileus was the most common finding (6/19, 31.5%), followed by intra-abdominal collections (3/19, 15.8%), pneumonia (2/19, 10.5%), enteritis/colitis (2/19, 10.5%), anastomotic edema or inflammation (2/19, 10.5%), haematomas (1/19, 5.2%), mechanical small bowel obstruction (1/19, 5.2%), overinfected seromas (1/19, 5.2%), heart failure and preexisting fecaloid peritonitis (1/19, 5.2%).