SMALL VESSELS
Wegener's granulomatosis
WG consists of ischemic necrosis with the formation of a non-microbial abscess and a polymorphonuclear granuloma containing polymorphonuclear leukocytes, lymphocytes and multinucleated giant cells.
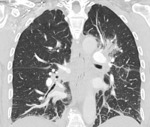
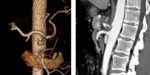
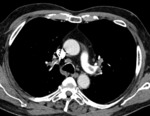
Imaging (Fig.3-Fig.7):
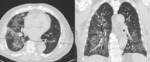
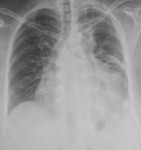
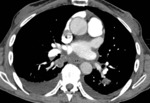
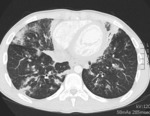
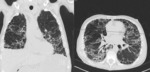
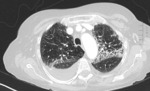
-CT Halo sign, characterized by a rim of ground-glass opacity surrounding the pulmonary lesion that represents alveolar hemorrhage around the nodule.
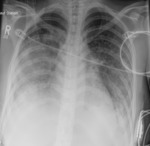
-Uni- or bilateral pulmonary infiltrates and pleurale effusion can be seen. Fig. 5
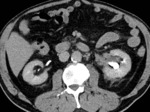
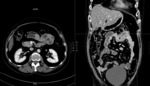
Renal involvement can lead to end-stage renal failure. Biopsy is important to esclude glomerulonephritis. Fig. 6
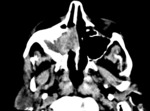
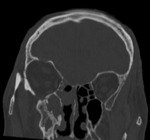
Long-lasting sinusitis or rhinitis is common. CT shows bone destruction. Fig. 7
Churg-Strauss syndrome (Eosinophilic Granulomatosis with Polyangiitis, EGPA).
In 1990, the American College of Rheumatology (ACR) proposed the following six criteria for the diagnosis of Churg-Strauss syndrome:
-Asthma (wheezing, expiratory rhonchi)
-Eosinophilia of more than 10% in peripheral blood
-Paranasal sinusitis
-Pulmonary infiltrates (may be transient)
-Histological proof of vasculitis with extravascular eosinophils
-Mononeuritis multiplex or polyneuropathy
Imaging findings (Fig.8-10):
Subpleural ground-glass attenuation or consolidation with lobular distribution, bronchial wall thickening, centrilobular nodules, interlobular septal thickenings, mediastinal or hilar lymphadenopathy, pleural or pericardial effusion. Fig. 9
Microscopic polyangiitis (MPA)
MPA is a systemic necrotizing vasculitis that affects kidneys (with blood and protein loss through the urine), lungs (alveolar hemorrhage or infiltrates), nerves, skin and joints.
Imaging Fig. 11 :
-Subpleural ground-glass attenuation or consolidation with lobular distribution usually bilateral;
-Centrilobular nodules, bronchial wall thickening and interlobular septal thickenings
Henoch-Schonlein purpura (HSP)
HSP is characterized by palpable purpura, arthralgias or arthritis, abdominal pain, GI bleeding, renal and pulmonary involvement.
Small vessel vasculitis containing IgA-dominant immune complex deposits.
Fig. 12
Essential cryoglobulinemic vasculitis
Cryoglobulins are single (Type I; associated with lymphoma, Waldenström’s macroglobulinemia, and multiple myeloma) or mixed immunoglobulins (80%, Type II and III, frequently presents as vasculitis, most commonly with recurrent lower extremity purpura, glomerulonephritis, and peripheral neuropathy) that undergo reversible precipitation at low temperatures.
Diagnosis: Biopsies of skin lesions and, where indicated, of kidney or other tissues.
Cutaneous leukocytoclastic angiitis (LCV)
LCV is a type of skin-predominant vasculitis, which most commonly presents with palpable purpura on the lower extremities.
Diagnosis: by extracutaneous manifestations and testing, or biopsy.
MEDIUM VESSELS
Polyarteritis nodosa (PAN)
PAN Involves: Kidney (75%), GI tract, peripheral nerve, skin (50%); M>F, any age
Imaging
Diffuse alveolar hemorrhage and Interstitial lung disease Fig. 13
Kawasaki disease
It is the most common cause of acquired heart disease in childhood.
Symptoms:
-The first phase, which can last for up to 2 weeks: fever, red eyes, erythema on the back, belly, lips, oral cavity, arms, legs, and genital area; edema of the hands and feet; swollen lymph glands in the neck
-The second phase presents: peeling skin on the hands and feet; joint pain; diarrhea; vomiting: belly pain.
Imaging findings:
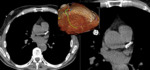
Giant coronary aneurysm that may be complicated by calcification, thrombosis, and even rupture. Coronary artery anatomy is best visualised with CT imaging and selective coronary angiography. Fig. 14
LARGE VESSELS
Takayasu's arthritis (TA)
Clinic: affect younger patients.
Symptoms: Claudication; dizziness, headaches or fainting; weakness and fatigue; chest pain; high blood pressure; Heart attack; Stroke.
Imaging findings Fig. 15 Fig. 16 :
• Vascular wall thickening (early stage);
• Arterial stenosis, occlusions and aneurysm (late stage).
Giant cell arteritis
Clinic: >50 years; predilection for the extracranial carotis arteries.
Symptoms: headaches, scalp tenderness, jaw pain and vision problems.
DD: TA
Imaging findings:
Aorta involvement (15%): Aneurysm; pulmonary involvement (rare) with nodules, interstitial lung disease Fig. 17
Vasculitis ass./ collagen vascular disease
Associated to: Scleroderma, Systemic lupus erythematosus, Rheumatoid arthritis, Dermatomyositis, Immune complex mediated vasculitis (Behçet disease and Goodpasture syndrome).
Goodpasture’s syndrome (GPS)
Glomerulonephritis, with or without pulmonary hemorrhage, and the presence of circulating anti–glomerular basement membrane (anti-GBM) antibodies.
Imaging findings: CT Fig. 18
Ground glass and airspace opacities that progress to reticular "crazy paving" pattern over a few weeks; hilar lymphadenopathy (rare).
Asymmetric pulmonary fibrosis, reticular opacities, and traction bronchiectasis (late phase).
Behcet’s syndrome
It is a chronic multisystemic vasculitis characterized by recurrent oral and genital ulcerations, uveitis and manifestations in multiple organ systems like large, medium and small vessels of both the arterial and venous circulation.
Presentation:
-Thoracic involvement;
-Thromboembolism of the superior vena cava and/or other mediastinal veins
-Aneurysms of the aorta & pulmonary arteries
-Pulmonary infarct & hemorrhage
Imaging Fig. 19 :
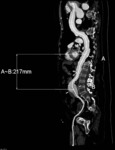
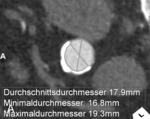
Wall-enhancing saccular pseudoaneurysms may develop in the abdominal and thoracic aorta. In one-fifth of affected patients, multiple pseudoaneurysms develop in large vessels such as the aorta and the iliac, femoral, popliteal and subclavian arteries.
Neuro-Behçet disease Fig. 20
Drug induced vasculitis
It is an inflammation (immune-complex mediated process) of blood vessels due to an adverse effect of a drug (propylthioruacil, hydralazine, minocycline, allopurinol, D-penicillamine, sulfasalazine, penicillins, cephalosporins and several immunomodulating agents). Usually serum ANCA positive.
Imaging findings:
Indistinguishable from other small vessel vasculitis.
Antiphospholipid antibody syndrome
Clinic:
Pulmonary hypertension; Thrombosis or stroke, History of heart murmur/ cardiac valvular vegetations/ nephropathy/ hematologic abnormalities. Fig. 21
Diagnosis:
Presence of circulating lupus anticoagulant and/or positive anticardiolipin antibodies or beta-2 glycoprotein I.