Type:
Educational Exhibit
Keywords:
Genitourinary, Genital / Reproductive system female, CT, MR, Ultrasound, Education, Education and training, Not applicable
Authors:
A. S. G. Costa1, A. S. C. C. Germano2; 1Amadora/PT, 2Barcarena /PT
DOI:
10.26044/ecr2020/C-10661
Findings and procedure details
From the archives of our institution, we selected US, CT and MR images that demonstrate the spectrum of the most common imaging findings of the normal and pathologic vagina, including congenital anomalies, solid masses, common use foreign bodies, traumatic and inflammatory/infectious conditions.
Anatomy of the normal vagina
-
The vagina is a fibromuscular tube that extends from the uterus to the vulvar vestibule, with an average length of 7-9 cm. Usually, its anteroposterior axis is shorter than its transversal axis, except in its upper portion where it surrounds the cervix; however its morphology, position and length are widely variable, since it’s a distensible structure that adapts to its surroundings. It is commonly oriented upper and dorsal, and its posterior wall is longer than the anterior wall.
-
The vaginal wall is composed of three layers: the mucosa, which is hormonally active, and the muscularis and the adventitia, this last one providing support.
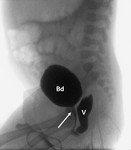
Conventional Radiology Appearance
US appearance
-
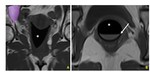
The vagina is best appreciated with a transabdominal midline sagittal approach. In premenopausal females, the normal vagina is seen as a hypoechoic tubular collapsed structure with a central hyperechoic line that represents the metabolic active mucosa (Fig. 2). In postmenopausal females, the vaginal mucosa is less echogenic due to a lack of estrogen stimulation (Fig. 3), making it more difficult to identify.
CT appearance
-
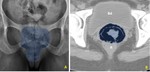
CT is very limited for the evaluation of the vagina, so it is important to know the normal anatomy to recognize it. In premenopausal women, the mucosa brightly enhances with intravenous contrast reflecting the hormonal influence (Fig. 4). The other layers are hypoattenuating and indistinguishable from the adjacent pelvic structures. In postmenopausal females, there is no enhancing of the vaginal mucosa, making its assessment even more difficult.
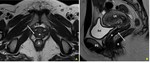
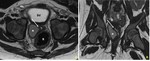
MR appearance
-
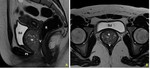
The anatomy of the vaginal wall is best appreciated on T2-weighted sequences (Fig. 5). On T1-weighted sequences, the vaginal wall has an intermediate and uniform signal intensity, which hinders its anatomical definition, making this sequence useful only for tissue characterization and for depicting enhancement after contrast administration.
-
The imaging appearance of the vagina varies with patient age and phase of the menstrual cycle. During the mid-secretory phase, the wall and central mucus are thickest and have the highest T2 signal. In postmenopausal women, the vaginal wall has decreased T2 signal and a thin mucus layer.
Congenital anomalies
-
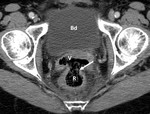
Vaginal congenital anomalies commonly have a nonspecific appearance at transabdominal US and CT: a complex cystic mass posterior to the bladder with or without endometrial cavity dilatation, representing the obstructed vagina, dilated and fluid-filled. It is crucial to correlate these findings with physical examination and clinical history.
-
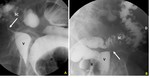
Vaginal anomalies include: a) imperforate hymen (Fig. 7 and Fig. 8), the most common, and easily diagnosed at physical examination, rarely requiring imaging studies; b) transverse septum, a fibromuscular membrane that divides the vagina into two segments reducing its length; c) longitudinal septum (Fig. 9 and Fig. 10), that divides the vagina in two parallel cavities that can go unrecognized unless there is obstruction in at least one of the cavities; and d) vaginal agenesis.
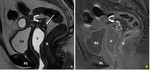
Cysts
-
Vaginal cysts are typically found incidentally at US, CT or MR done for other reasons. MR is the best modality to adequately determine its anatomic location, differentiating vaginal cysts (Gartner duct and Bartholin gland cyst) from cysts of adjacent structures (cervical and urethral cysts).
Solid lesions
-
Solid lesions of the vagina include benign and malignant abnormalities, such as leiomyomas, endometriosis (Fig. 13), primary malignancies and metastases.
-
Primary malignancies (Fig. 15) are also rare, the commonest type being squamous cell carcinoma, that is associated with the human papillomavirus. CT is frequently used for staging, but MR is better to define local invasion.
-
Metastases to the vagina are much more common than primary neoplasms (Fig. 16) and account for 80% of vaginal tumors. Most originate from adjacent cancers and spread contiguously, such as ovarian, cervical, endometrial and rectal cancers.
Foreign bodies
-
Pessary devices (Fig. 19), used for the treatment of uterine, vaginal, urinary and rectal prolapses, have a wide variety of sizes and shapes and are mostly found in elderly patients. The most common morphology is the "donut" of silicone (Fig. 20).
Traumatic
-
Even though obstetric-related trauma is the most common cause of injury to the vagina, trauma of non-obstetric origin is not infrequent. Severe lacerations may result in large volume vaginal bleeding, shock and even death. The most common mechanism of non-obstetric injury is coitus (Fig. 23).
Inflammatory/Infectious
-
The vagina is, by far, the female genital most involved in fistula formation. Colovaginal fistulas are most frequently caused by sigmoid diverticular disease (Fig. 27) and most women with these fistulas are hysterectomized. Other causes of fistulas involving the vagina include gynecologic neoplasms (Fig. 28), inflammatory bowel disease and radiation (Fig. 29, Fig. 30, Fig. 31 and Fig. 32). Post-radiotherapy vaginal stenosis (Fig. 33) can also occur. Sometimes the cause of the fistula is unknown (Fig. 34).