Multiple common and uncommon pathologies will be discussed:
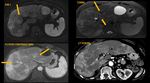
CASE 1 (Figure 2): Acute Ascending Cholangitis with perfusional changes.
Transient Hepatic Attenuation Differences (THADs), which appear as focal or diffuse hyperdense areas during the hepatic arterial phase on CT, have been reported in patients with acute cholangitis.
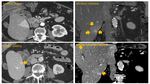
CASE 2 (Figure 3): Liver Hemangioma with associated perfusional changes.
With dynamic liver imaging on CT/MRI, both benign and malignant tumours can show perfusional changes due to the presence of portosystemic shunts. These appear as wedge-shaped enhancement on the arterial phase, which becomes less conspicuous on the subsequent phases.
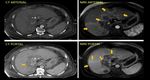
CASE 3 (Figure 4): PID with associated Fitz-Hugh–Curtis syndrome
Fitz-Hugh–Curtis syndrome is 'perihepatitis' associated with pelvic inflammatory disease. CT shows localized right upper quadrant peritonitis associated with salpingitis. Thickening and abnormal enhancement of the anterior liver capsule can also be seen. Reversible perfusion defects within the right lobe of the liver can be seen due to partial hepatic venous outflow obstruction from the perihepatic inflammatory process.
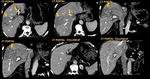
CASE 4 (Figure 5): Torted extrauterine fibroid with hepatic capsular inflammation.
This is an unusual case, with the pathophysiology likely similar to Fitz-Hugh-Curtis syndrome.
CASE 5 (Figure 6): Inflammatory Pseudotumors of Liver.
Inflammatory pseudotumor is due to the proliferation of plasma cells, other inflammatory cells, fibrous stroma and spindle cells, sometimes associated with a granulomatous reaction. These can be associated with IgG4 disease. This can mimic true hepatic neoplasms such as HCC.
CASE 6 (Figure 7): Nutmeg Liver.
This perfusion abnormality of the liver is due to hepatic venous congestion. Mottled enhancement is seen in the arterial and early portal venous phase with decreased enhancement of the liver periphery. This can be seen with congestive hepatopathy, hepatic veno-occlusive disease and Budd-Chiari syndrome.
CASE 7 (Figure 8): Hepatic infarction.
Hepatic infarction is defined as areas of coagulation necrosis resulting from hepatocyte cell death caused by local ischemia. Ischemia is commonly due to a thrombus or embolus that has obstructed circulation to the affected area. Infarction due to hepatic artery thrombosis most often occurs after liver transplantation. Hepatic infarction is uncommon, due to the dual blood supply from the hepatic artery and portal vein.
CASE 8 (Figure 9): Budd-Chiari due to hepatic vein occlusion.
Budd-Chiari syndrome is defined as lobar or segmental hepatic venous outflow obstruction at the level of hepatic veins or inferior vena cava (IVC). Primary causes of venous outflow obstruction include congenital factors, such as webs/diaphragms, injury and infection. Secondary causes are commonly thrombotic, related to hypercoagulability due to oral contraceptives, pregnancy, polycythemia, etc.
CASE 9 (Figure 10): Budd-Chiari due to absence of suprahepatic IVC.
This is an unusual cause of Budd-Chiari syndrome due to the congenital absence of the suprahepatic IVC.
CASE 10 (Figure 11): Portal vein thrombus with perfusional changes.
Complete occlusion of the main or branch of the portal can lead to the appearance of THADs in the arterial/early portal venous phase, showing increased enhancement/perfusion defect in the liver segment previously supplied by the portal vein due to hepatic arterial compensatory flow.
CASE 11 (Figure 12): Hot spot sign with IVC stenosis/obstruction.
The hot spot sign is caused by portosystemic venous shunting between the superior vena cava and the portal vein. Similarly, if there is inferior vena cava obstruction, hyperenhancement in segment IV of the liver can also be visualized if contrast is injected into a lower extremity vein. 99mTc–sulfur colloid scans also demonstrate uptake in hepatic segment IV and this sign was traditionally described for technetium scans.
CASE 12 (Figure 13): Chemotherapy-induced hepatitis.
Chemotherapy-induced focal hepatopathy (CIFH) is a focally accentuated manifestation of liver injury caused by chemotherapeutic drugs, including steatosis, steatohepatitis and sinusoidal obstruction syndrome. CIFH can be differentiated from metastasis because of the non-mass wedge-shaped enhancement. CIFH should be considered when new liver abnormalities are seen in patients undergoing chemotherapy.
CASE 13 (Figure 14): Hereditary Hemorrhagic Telangiectasia (HHT)
Symptomatic liver involvement by HHT is uncommon and has been categorized into three distinct clinical patterns. Patients are divided into clinical subtypes characterized by high-output cardiac failure, portal hypertension or biliary disease. The symptoms are the result of arteriovenous, arterioportal or portovenous hepatic shunting.