Keywords:
Genitourinary, Colon, Contrast agents, Genital / Reproductive system female, MR, Contrast agent-other, Health policy and practice, Outcomes analysis, Outcomes, Retrospective, Diagnostic or prognostic study, Performed at one institution
Authors:
R.-E. Chung1, S. LEE2, A. Stankiewicz1, J. ritchie1; 1Stoke-on-Trent/UK, 2Stoke on Trent/UK
DOI:
10.26044/ecr2020/C-10859
Purpose
Endometriosis is a common gynaecological presentation seen in clinical practice with uncertain aetiology. Endometriosis can be broadly categorised into its location of involvement, whether they are superficial or within the deep spaces.1 However more significantly it can be recognised by their depth of infiltration, whether they are embedded with depth greater than 5mm (deep), or less (superficial). Deep infiltrative endometriosis is known for its complexity in different stages of clinical practice. There is often delay in diagnosis with significant debilitating symptoms and multiple hospital consultations, subsequently requiring more complex surgeries. Therefore, deep infiltrative disease warrants an MDT approach into management, with imaging workup guiding the overall management.
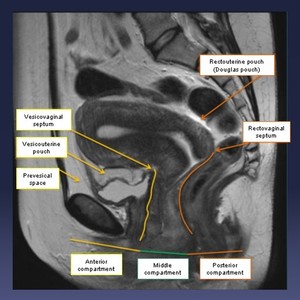
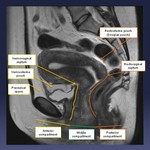
Fig. 1: Figure 1. MRI Pelvis T1w Sagittal view highlighting the normal anatomy.
References: R. M. Viguer Benavent et al. (2015) MRI findings in endometriosis :https://posterng.netkey.at/esr/viewing/index.php?module=viewing_poster&task=viewsection&pi=128262&ti=428336&si=1482&searchkey=
There remains no consensus of MRI’s diagnostic performances despite its crucial role in early accurate mapping of lesions for pre-operative staging and planning. The European Society of Urogenital Radiology (ESUR) has published a comprehensive guideline for MRI imaging of pelvic endometriosis2 that provides advice on the various factors in MRI protocol and patient preparation that might improve detection accuracy, which forms the basis of the protocol formulated in our local centre. Thus, we aim to assess the diagnostic performance of MRI in our hospital in detecting deep infiltrative colorectal endometriosis without the use of rectal contrast in concordance with the recent ESUR guidelines.

Fig. 2: Guidelines published by ESUR on MRI imaging of pelvic endometriosis.
References: European society of urogenital radiology (ESUR) guidelines: MR imaging of pelvic endometriosis Eur Radiol (2017) 27:2765–2775 DOI 10.1007/s00330-016-4673-z 5 December 2016