Type:
Educational Exhibit
Keywords:
Abdominal Viscera, Abdomen, Peritoneum, CT, MR, Ultrasound, Biopsy, Metastases, Neoplasia, Not applicable
Authors:
K. Kuriyama1, T. Koyama1, S. Nakashita2, K. Nakatani2, Y. Ishizaka1, K. Notohara2; 1Kurashiki/JP, 2Kurashiki, Okayama/JP
DOI:
10.26044/ecr2020/C-11398
Findings and procedure details
I. Image guided biopsy for omental cake
1) Indication
The indication for image-guided biopsy is the patients who were found to have omental cake but without any clinically apparent primary. CT is commonly used modality of choice for image-guidance. However, ultrasonography also have some advantages for biopsy, and is usually applied in our institute. Real-time visualization on US have advantages in avoiding vessels and intestine. The success of the procedure depends on the proficiency of the operator. Reported sensitivity and specificity of image-guided biopsy are 93 to 96% and 86 to 100%, respectively.
The presence of ascites do not hinder the procedure as far as the thickened omentum can be visualized in ascites. Of note is interventional radiologist should pay attention to whether there are any other more preferential site for biopsy, such as the liver, supraclavicular or inguinal lymph nodes, or umbilicus.
2) Techniques
Before the biopsy
- Obtain informed consent for the procedure and complications from the patients
- Confirm the coagulation parameters and platelet counts are within normal range
- Clean the planned needle entry area and surrounding area with providone iodine
- Apply local anesthesia by 0.5% lidocaine hydrochloride to the needle entry point and abdominal wall
US-guided biopsy
- Envelope the ultrasonography probe with sterile cover and attach the needle guidance
- Depict of the omentum on the needle path projected by needle guide software
- Assess needle path with Doppler US to avoid vessels
- Insert the biopsy needle along the course of needle path, and then perform the biopsy
II. Differential diagnosis of omental cake
Peritoneal carcinomatosis
- most common causes for omental cake
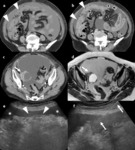
- majority of cases results from abdominal malignancies, including stomach, colon, gall bladder, pancreas, ovary, uterus (fig.1,3-5).
- Extra-abdominal tumors such as carcinomas of the breast, lung or malignant melanoma may be the primary (fig.2).
- specific forms include primary peritoneal serous carcinoma / pseudomyxoma peritonei
Primary peritoneal serous carcinoma
- has been considered as an epithelial tumor that arises from the peritoneum, previously
- now is considered originating from serous tubal intraepithelial carcinoma (STIC)
- markedly elevated of CA125 is one of clues to suspect this condition
- good response for chemotherapy in most of cases
Imaging findings
- similar to other peritoneal carcinoma but without any gross ovarian masses (Fig.6)
- extensive calcification is seen in psammomacarcinoma (Fig.7)
- careful investment of the endometrium to exclude uterine primary (Fig.8).
Pseudomyxoma penitonei
- condition characterized by mucin producing cell widely disseminated on the peritoneal surfaces
- majority of cases derive from low-grade mucinous tumor of the appendix
- female > male
- some cases result from mucinous carcinoma of the appendix and other site of gastrointestinal tract, pancreas, ovary and convey worse prognosis (fig.9)
- patients typically present with abdominal fullness due to rapidly increasing mucinous ascites
Imaging findings
- large amount of ascites with scalloped indentation of the surface of the liver and spleen
- echogenic ascites on ultrasonography suggesting gelatinous fluid
- in female patients, multilocular cystic ovarian simulating ovarian primary may be present
- small cystic lesion in the appendix
- unlike other peritoneal implants, usually nodular lesions are absent
- tumors do not invade visceral organs or metastasize in except for cases of carcinomas
Peritoneal lymphomatosis
- unusual form of non-Hodgkin's lymphoma that diffusely involve the peritoneum
- most frequently diffuse large B-cell lymphoma, but other subtypes of lymphoma, including Burkitt lymphoma and follicular lymphoma, can cause this condition
Imaging findings
- smudged appearance and omental cake suggesting infiltration of the omentum (Fig.10)
- simultaneous involvement of the small intestine resulting marked wall-thickening and aneurysmal dilatation are important findings suggestive of lymphoma
- involvement of mesenteric lymph nodes, frequently produce “sandwich sign” is another important sign of lymphoma
Desmoplastic small round cell tumor (DSRCT)
- a rare but highly aggressive neoplasm that afflicts mainly adolescents and young adults
- male> female
- pathologically characterized by small round cell tumors associated with marked desmoplastic changes
- belongs to the family of PNET/ Ewing tumor associated with specific gene translocation of t(1;22) (p13;q12)
Imaging findings
- multiple soft-tissue masses in the omentum, mesentery, peritoneal surfaces, without a distinct organ of origin (Fig.11)
- usually seen in the pelvic cavity (retrovesical or rectouterine space)
- heterogeneous appearance due to intratumoral necrosis and hemorrhage
- occasionally associated with calcification
Malignant peritoneal mesotheliomas
- rare neoplasms that arise from the mesothelial cells of the peritoneum
- male> female
- asbestos exposure in at least 60% of male cases
Imaging findings
- tend to spread in sheets of tissue over the parietal and visceral peritoneal surfaces and to become confluent, thereby encasing the abdominal organs (Fig.12)
- may have scalloping or direct invasion of adjacent abdominal organs
Inflammatory conditions
Tuberculous peritonitis
- usually secondary to primary deposit in lymph node or intestine
- almost always involves the ileocecal region, usually both the terminal ileum and cecum
- clinical manifestation includes mildly elevated c-reactive protein, and WBC
- patients commonly complaints abdominal fullness and vague abdominal pain in the right lower quadrant
- the patients usually do not have pulmonary involvement
- elevated ADA (adenosine deaminase) in the ascites is useful in establishing the diagnosis, though image-guided biopsy of the omentum can demonstrate granulomatous peritonitis
Imaging findings
- smooth thickening the peritoneum (Fig.13)
- the amount of the ascites vary according to the cases, though most cases are associated with large amounts of free or loculated ascites (wet type)
- ascites can be minimal or absent (dry type)
- fibrous adhesions of the mesenterium or intestine (fibrous type)
- nodular implants are uncommon
- diffuse and extensive FDG-uptake in the thickened peritoneum
Peritoneal actinomycosis
- closely associated with the prolonged use of intrauterine device (IUD)
- even occur months after the removal of an intrauterine device
- disease can spread over anatomical barriers since the microorganisms have an enzyme that destructs the fascia or membranes
Imaging findings
- presence of long-term placed IUD in the uterine endometrium
- ill-defined lesion spreading over the anatomic barriers
- extensive spread from the uterus to surrounding organs, including urinary bladder, rectal area, urachus, abdominal wall, and peritoneum, and may simulate malignancy (Fig.14)
- usually associated with solid adnexal masses