Keynotes:
•The incidence of Acute Aortic Dissection (AAD) is estimated to be 3 cases per 100.000 people per year with mortality of 1-2 % per hour without surgical treatment.
•Aortic Dissection (AD) with a type A prevalence is linked in 65%+ to patients with Marfan Syndrome (MS).
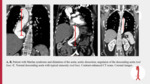
•Contrast-enhanced computed tomography (CT) is the gold standard in the diagnosis of AD.
•According to the American Heart Association (AHA) guidelines, every fifth patient with type A AD needs the next stage surgical treatment within 5 years after the first cardiac surgery.
The most lethal of all aortic diseases
- Acute ascending aortic dissection is a life-threatening condition with a surgical emergency requiring prompt diagnosis and treatment [1].
- Between 2,6-3,5 new cases of AAD are diagnosed from 100K people every year, most of them being men, around the age of sixty.
High mortality rate without surgical treatment
- Without treatment, the lethality rate is 1 to 2% per hour after a sudden onset of symptoms [2]
- The expected 90-day mortality of 70% to 90% without surgical therapy [3]
- Doubtless, timely diagnosis is crucial to permit prompt surgical management [4].
Post-operative mortality rate according to the International Registry of Acute Aortic Dissection (IRAD)
- Despite continuous improvements in imaging techniques, medical therapy and surgical management, early mortality in patients undergoing Type A AAD repair still remain high, ranging from 17% to 26% [5].
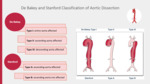
Different classifications of aortic dissection [6-8]:
- Stanford classification (Fig. 2)
- De Bakey classification (Fig. 2)
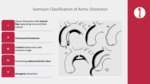
- Svensson classification (Fig. 3)
- Penn classification (Fig. 4)
The key to successful treatment is a good visualization of the aortic pathology.
The information must be reported and fulfil preoperative requirements for surgical intervention:
- initial intimal tear;
- aortic diameter;
- entry and reentry sites;
- patency of the false lumen;
- hemopericardium / tamponade?
- aortic branch and coronary ostia involvement;
- aortic valve competency;
- blood extravasation in surrounding spaces.
The underlying mechanism of type A AAD is tearing through the intima into the aortic wall (intimal tear), with the entry of luminal blood into the wall, resulting in the formation of a false lumen partitioned from the true lumen by the intimal flap [9]. (Fig. 5)
In Type A AAD patients, end-organ malperfusion is one of the most catastrophic complications that adversely influences outcomes.
It has an incidence ranging from 16% to 34%, and may involve any of the major arterial side branches resulting in [10]:
- myocardial
- cerebral
- spinal cord
- visceral
- limb ischemia (Fig. 6)
Marfan syndrome
• 6-8% of patients with Type A AAD has Marfan syndrome
• Marfan syndrome is a hereditary disorder with the defect of the fibrillin 1 (FBN 1) gene [9]
• The aortic pathology is registered in near 65-100% patients with Marfan syndrome
• The prevalence of type A dissection among patients with Marfan syndrome at 60 years of age is approximately 50% [11]. (Fig. 7)
According to the American Heart Association Guidelines, 2015
Every 5th patient with type A AAD after the 1st cardiac surgery procedure needs the next stage of surgical treatment during the first 5 years.
Progressive pathologies:
- Proximal aorta (aortic root; aortic annulus)
- Distal thoracic aorta (aortic arch; descending aorta)