Type:
Educational Exhibit
Keywords:
Not applicable, Ischaemia / Infarction, Imaging sequences, Diagnostic procedure, MR, CT, Neuroradiology brain, CNS, Neuro
Authors:
L. Guirado Isla, I. Garrido Márquez, P. PÉREZ NARANJO, M. Revelles Paniza, J. A. Miras Ventura, L. Díaz Rubia, C. Martínez Martínez, M. Fernández Conesa; Granada/ES
DOI:
10.26044/ecr2020/C-12465
Background
Ischemic stroke constitutes a pathology with a great social impact due to its frequency, mortality and potential physical sequelae, with a worldwide incidence of approximately 200 cases per 100,000 inhabitants/year according to the World Health Organization. It consists of an interruption in cerebral circulation that leads to a significant decrease in blood flow, associated with a neurological deficit.
It is usually of thromboembolic etiology, produced up to 35% by occlusion of a large intracranial vessel (distal internal carotid artery, proximal middle cerebral artery or basilar artery), followed by occlusion of arterial branches and small perforating vessels. Less frequently they are secondary to arterial dissection.
Age, history of previous stroke, hypertension, smoking, diabetes mellitus or heart disease have been described as risk factors.
Pathophysiology: when vascular occlusion occurs there is a decrease in oxygen and glucose levels that triggers a cascade of compensatory mechanisms and ultimately generates necrosis of the affected territory.
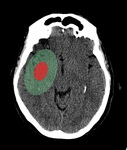
In this context it is necessary to define two concepts: ischemic core and penumbra (Fig. 1). The term core refers to infarcted brain tissue adjacent to the occlusion, with poor or absent blood flow, while penumbra includes viable ischemic tissue with low blood flow, maintained by collateral circulation. The latter can persist until 12-24 h after the onset of acute clinical episode.
As a result of these processes edema appears, on the one hand of the cytotoxic type secondary to the failure of the cell membrane potential, and on the other vasogenic due to the alteration of the blood-brain barrier.
In the acute phase there is a predominance of the edema, while in the subacute phase the swelling decreases and the blood-brain barrier repair takes place. Finally, during the chronic phase the lesion can remain as an area of encephalomalacia.