Review
There are many scientific concepts of normal COW [2]. Lack of posterior communication arteries (Pcomm) visualization on MR-angiography in some publications considered as aplasia. Others believe that their diameter so small that blood flow is not visible [3, 4].
Studies relating to the posterior COW (Pcomm and first posterior cerebral arteries segment P1) actively discuss periods of their formation [5]. Embryological studies generally distinguish three types of embryo circulation:
- Fetal - in which posterior cerebral artery (PCA) mostly derives from Internal Carotid Artery (ICA)
- Transitional - in which diameters P1=Pcomm
- Adult - in which diameters of P1>Pcomm
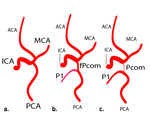
In certain individuals, a unilateral or bilateral fetal or transitional types functions in adulthood [7], (fig 3)
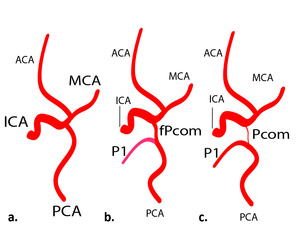
Fig. 3: Scheme of cerebral arterial types reflecting of fetal circulation development stages: a) fetal, b) transitional, c) adult.
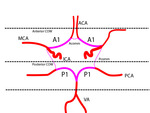
Closed COW is formed by precommunicant anterior cerebral artery segment (A1), anterior connective artery (Acomm), Pcomm's, P1. COW divided into anterior and posterior parts (fig 4).
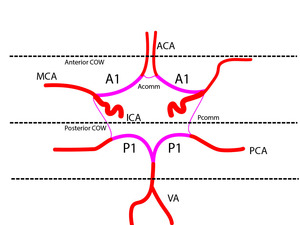
Fig. 4: Scheme of arteries that compose the COW
The anatomical variants are only if the anterior or posterior part of the COW opens. Although ACA is also a controversial issue because it is like the Pcomm arteries have a small diameter and is poorly visible on MR [8-10].
The components of groups
In our study the above variants of COW distributed into 5 groups (table 3):
Patients in groups Table 3
|
Group type
|
Patients (n)
|
Average age
|
Atherosclerotic
patients
|
|
Normal
|
27
|
47
|
2
|
|
Fetal
|
12
|
48
|
4
|
|
Transition
|
14
|
34
|
0
|
|
VA hypoplasia/aplasia
|
13
|
38
|
1
|
|
ACA hypoplasia/aplasia
|
5
|
39
|
2
|
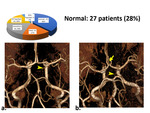
Normal. In a large number of patients - 27 (38%) were found a normal COW structure in which the Pcomm arteries are superfine or not visualized. 2 patients with the median artery of the corpus callosum arose from the Acomm artery were included in this variant (fig 5).
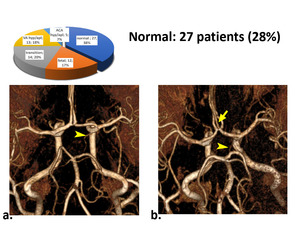
Fig. 5: Normal cerebral circulation type, one side thin Pcomm visible (arrowheads). a) Standard. b) With arteries of corpus callosum from Acomm (arrow).
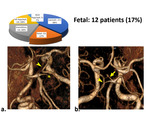
Fetal. The second largest group consisted of 12 (17%) patients with PCA from ICA - fetal type of blood circulation or trifurcation of the ICA. At the same time, only 4 patients had total aplasia of the P1 and the opened COW (fig 6).
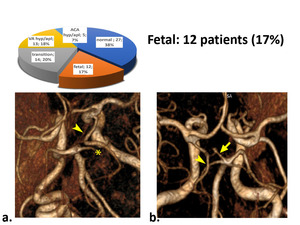
Fig. 6: Fetal cerebral circulation type, PCA from ICA are seen (arrowheads). a) Fetal type with aplasia P1, superior cerebellar artery (*). b) Fetal type with hypoplasia P1 (arrow).
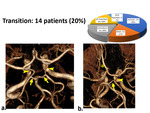
Transitional. In 14 (26%) patients from the third group visualized one-or-two-side transitional (from fetal to adult) form of COW type with the equivalent diameter of P1 and Pcomm artery. In one case, a transient type was combined with the presence of an azygos ACA (fig 7).
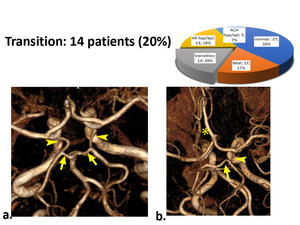
Fig. 7: Transitional cerebral circulation type, Pcomm are seen (arrowheads) in equal diameter with P1 (arrow). a) Bilateral transition type. b) Unilateral transition type with ACA azigos (*).
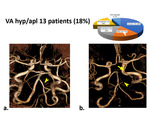
VA hypoplasia/aplasia. The next group was 13 (18%) patients with hypoplasia of the intracranial segment of the vertebral artery (VA). Most patients had a normal COW and in four patients this variant was supplemented by fetal or transitional types on one or two sides (fig 8).
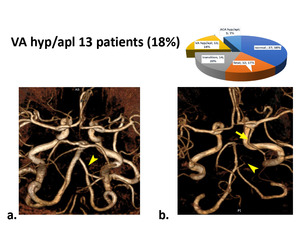
Fig. 8: Type of hypoplasia or aplasia of VA (arrowheads). a) Unequal diameter of VA. b) Aplasia of VA and its transition to the cerebellar artery (arrowhead), combined with the fetal type (arrow).
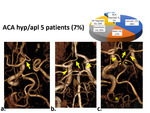
ACA hypoplasia/aplasia. The smallest group was 5 (7%) patients with A1 hypoplasia (3 patients) or aplasia with the ACA bifurcation on the other side. In two patients, this variant was combined with fetal or transitional type on both sides and VA hypoplasia (fig 9).
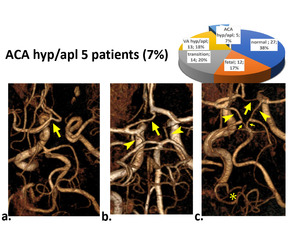
Fig. 9: Type of hypoplasia or aplasia of ACA. a) ACA aplasia on one side and ACA bifurcation on the other side (arrow). b) Aplasia of the A1 segment of ACA (arrow), combined with the bilateral transition type (arrowhead). c) Multiple variants: Aplasia of A1 segment of ACA (arrow), bilateral fetal type (arrowheads) with P1 segment of PCA hypoplasia (arrow), VA aplasia (*).
The results of the patient's survey
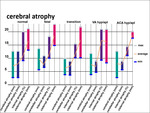
Cerebral liquor spaces measurements as atrophy signs and brain vascular changes grading distributed by groups (Diagrams 1, 2).
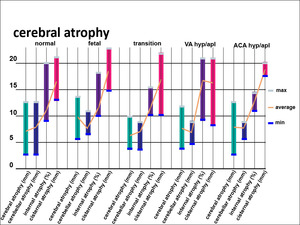
Fig. 10: Diagram 1
Diagram 1 shows the ranges of the measured liquor spaces.
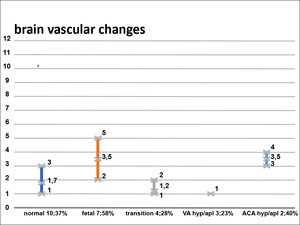
Fig. 11: Diagram 2
Diagram 2 shows the grouped scores of vascular brain changes on the scale (see table 2) and the number of patients in which they identified.
Analysis of patients' headache level and clinical complaints distributed by groups (Diagrams 3, 4).
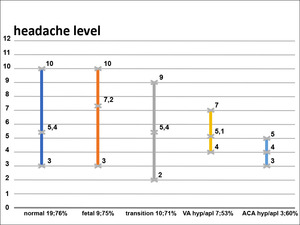
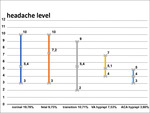
Fig. 12: Diagram 3
Diagram 3 reflects minimal/average/maximal levels of headache in group and percentage of patients heaving headache.
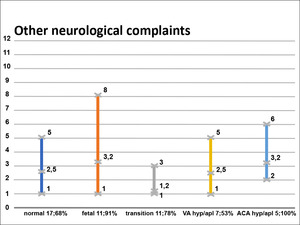
Fig. 13: Diagram 4
Diagram 4 reflecting on the number of complaints except for headache and percentage of patients having at least one.
Discussion
Comparative analysis liquor spaces wideness in diagram 1 revealed roughly the same maximal/average/minimal levels in groups with small increases in maximum values in the fetal group.
Diagram 2 revealed a higher percentage of patients with vascular brain changes and decreasing in maximal and average values iv the fetal group. In VA hyp/aplasia group shown the lowest percentage and value these changes.
It noticed that maximum changes were found in aged patients with carotid atherosclerosis. In the fetal group, there were the highest number of atherosclerotic patients (table 1) this can be explained by the increase in values in diagrams 1, 2 and minimum values in VA hypo/aplasia group which did not contain such patients.
In diagram 3, there was no increase in headache scores and a percentage of patients in groups of arterial variants compared to the norm group. But there was a higher average level in fetal group.
Diagram 4 demonstrating increasing in the maximum and the average number of other complaints (Table 2) and the percentage of patients with complaints in the fetal and ACA hypo/aplasia groups compared to the norm group.