Case#1:
Patient with history of neurogenic bladder was signed out to our computed tomography (CT) technician as having a recently placed suprapubic catheter that was no longer draining after the patient returned from a diagnostic procedure. The primary nurse placed a foley catheter prior to the patient’s transfer to our department and stated that it was draining mildly cloudy blood tinged urine. Upon receiving the patient in our department, the technician noted the suprapubic catheter and an appropriately draining foley catheter.
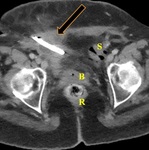
The CT pelvis demonstrated the suprapubic catheter with its tip terminating outside the confines of the urinary bladder with the tip terminating in the space of Retzius and the catheter balloon inflated in the right rectus abdominis muscle (Fig. 1 and 2). This information was immediately relayed to the primary team who concluded that the catheter must have been pulled back during transport of patient and requested the interventional radiologist to remove the suprapubic catheter.

Fig. 1: Axial contrast enhanced CT through the pelvis demonstrates a suprapubic catheter with balloon inflated in the right rectus sheath muscle (orange block arrow) and the tip terminating outside the urinary bladder (B). The rectum (R) is seen posterior to the bladder and the sigmoid colon (S) is seen in the left lateral pelvis.

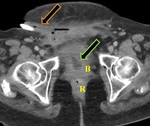
Fig. 2: Axial contrast enhanced CT through the pelvis demonstrates a suprapubic catheter tubing in the right groin with adjacent subcutaneous gas and soft tissue stranding (orange block arrow). The collapsed urinary bladder (B) is anterior to the (R), with a partially visualized foley catheter balloon tip (green block arrow).
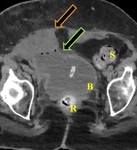
A follow-up CT pelvis (Figure 3) demonstrated a thickened right rectus abdominis muscle bundle, an iatrogenic urinary bladder diverticulum with neoepithelialization and an appropriately positioned foley catheter in the urinary bladder.

Fig. 3: A follow-up axial noncontrast CT through the pelvis after removal of the suprapubic catheter demonstrates thickening of the right rectus sheath muscle (orange block arrow). The distended urinary bladder (B) demonstrates discontinuity and neoepithelialization with an iatrogenic bladder diverticulum (green block arrow). The collapsed rectum (R) is posterior to the bladder and the sigmoid colon (S) is seen in the left lateral pelvis.
Case#2:
Patient was brought to the radiology department for a chest radiograph to evaluate positioning of the two left chest tubes. Prior to their arrival to the department, the x-ray technician received a hand-off from the patient’s nurse that the chest tubes were functioning well and draining the left pleural effusion and the left pneumothorax. After arrival to our department, the patient began complaining of left sided chest pain, and elicited pain over the left chest tube insertion site. The technician immediately alerted the radiologist of an acute change in patient’s condition.
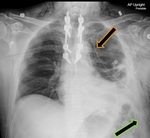
Upon review of the image, it was determined that the chest tube had been retracted into the thoracic soft tissues and appeared kinked at the left lung base (Fig. 4). Moderate amount of subcutaneous air was also noted in the left thoracic soft tissues, which was new from prior chest radiograph. This information was immediately relayed to the primary team. Physical exam revealed that the suture holding the chest tube in place had come undone sometime during transport which resulted in retraction of the chest tube into the thoracic soft tissues during transport to the stretcher.

Fig. 4: Chest X ray demonstrates a left pleural effusion in the presence of a left apically directed chest tube (orange block arrow), and a kinked and retracted left basilar chest tube (green block arrow). The side port of the retracted chest tube is outside the field of view and likely terminating the subcutaneous soft tissues. Note the subcutaneous air in the left lateral thoracic soft tissues
Case#3:
A portable chest radiograph was requested on a patient status post ST elevation myocardial infarction (STEMI) on intra-aortic balloon pump (IABP) complaining of intermittent upper extremity paresthesia. After performing the portable chest radiograph, the technician immediately called the radiologist to inform them of a ‘dark spot’ in the expected location of the aortic knob, and they were concerned about a possible artifact and requested that they repeat the chest radiograph. Upon review of the image, all life support monitoring lines and tubes were thoroughly evaluated. In addition, it was noted that the IABP was malpositioned extending into the aortic arch with the proximal marker positioned somewhere in the ascending aorta and the distal marker positioned somewhere in the distal thoracic descending aorta (Fig. 5). The primary team was immediately informed of this critical finding for emergent management of the malpositioned IABP and a repeat chest radiograph was not performed.

Fig. 5: Chest carestream radiograph demonstrates several lines and tubes in the chest: Right internal jugular venous sheath (green solid arrow) with a Swan Ganz catheter terminating in the pulmonary outflow tract (yellow solid arrow). Additional lines include: endotracheal tube (red solid arrow), enteric catheter with the side port below gastroesophageal junction (purple solid arrow), and 3 perimediastinal chest tubes (blue solid arrows). It may sometimes be difficult to notice ALL lines and tubes in the presence of so many monitoring devices, but note the inflated intra-aortic balloon pump in the aortic arch (orange block arrow), with the proximal marker in the ascending aorta (green block arrow) and the distal marker in the distal thoracic aorta (yellow block arrow).