Background: Pelvic floor weakness refers to a spectrum of functional disorders caused by impairment of the ligaments, fasciae, and muscles that support the pelvic organs. Such disorders include urinary and fecal incontinence, obstructed defecation and pelvic organ prolapse. The most significant risk factors are ageing and female sex.
Pelvic organ prolapse is the abnormal descent of a pelvic organ through the hiatus beneath it. This condition may affect the bladder (cystocele), vagina (vaginal prolapse), uterus (uterine prolapse), mesenteric fat (peritoneocele), small intestine (enterocele) or sigmoid colon (sigmoidocele). Pelvic floor weakness may involve only one organ but usually tend to evolve to a multiorgan or multi-compartment prolapse.
Physical examination for assessing pelvic organ prolapse often leads to underestimation of the number of compartments affected. Moreover, failure to recognize prolapse in a substantial number of patients by using this approach contributes to high rates of therapeutic failure. [1]
MRI with dynamic sequences has been proven accurate and reliable for identifying pelvic floor weakness, because it allows all three compartments to be visualized simultaneously and lead to a change in surgical therapy. [2]
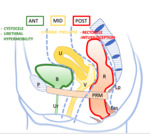
Anatomy: The pelvic floor is classically described as comprising three compartments: an anterior compartment containing the bladder and urethra, a middle compartment containing the vagina and uterus, and a posterior compartment containing the rectum.
The supporting structures of female pelvis consist of three layers from a superior to an inferior location: the endopelvic fascia, the pelvic diaphragm, and the urogenital diaphragm. [3]
Technique: 42 patients (40 Female; 2 Males; mean age 57,1) with symptoms consistent with pelvic floor disorders underwent a pelvic MR examination during 2019.
Our MRI protocol includes Static sequences made up of triplane T2-weighted (FSE) and sagittal Dynamic images (SSFSE) images during rest, squeezing, straining (Valsalva manoeuvre) and evacuation plus transverse plane images during rest and straining. Prior to the examination, the patient should be trained on how to correctly perform the dynamic phase and the of Ultrasound gel is introduced to distend the rectum.
Measurements: Static sequences were used to asses morphology of the supporting structures and anal sphincter complex, while dynamic ones to study abnormality of the pelvic organs by analyzing their position with reference lines in agreement with ESGAR/ESUR most recent recommendations. [4]
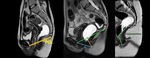
The pubococcygeal line (PCL) is the reference line most frequently used for measuring organ prolapse. It is drawn from the inferior border of the pubic symphysis to the last coccygeal joint and represents the line of attachment of pelvic floor muscles and thus the level of the pelvic floor.
Perpendicular lines drawn from PCL points in the anterior, middle, and posterior pelvic compartments to the PCL are drawn for the assessment of organ prolapse. The perpendicular distance from the reference points to the PCL must be measured both at rest and during the evacuation phase.
The severity of prolapse can be quickly graded according to the “rule of three” explained in the underlying table
Then, the H line and M line are measured. The H line corresponds to the anteroposterior width of the levator hiatus while The M line is a vertical line drawn perpendicularly from the PCL to the most posterior aspect of the H line and represents the vertical descent of the levator hiatus.
The anorectal angle is measured between two intersecting lines, one representing the central axis of the anal canal and the other passing by the posterior wall of the distal rectum. Notice that the angle becomes more acute during squeezing and more obtuse during defecation. Average value is <115°.
In the axial plane, the normal configuration of the anal sphincter must be assessed. (normal value at rest < 45mm, after Valsalva manoeuvre < 65mm).
The components of the levator ani muscles are clearly evident on T2-weighted MR images and should be of similar thickness, with homogeneous low signal intensity.
In the coronal plane, the iliococcygeus and pubococcygeus muscles can be easily assessed because of their horizontal position and upward convexity. Thinning and loss of its typical upward convexity should be noted.
Lastly, we note the urethral axis evaluating the angle between the urethra axis itself in the sagittal plane and PCL.
Template: Significant findings and measurements were reported following a structured template drawn up to standardize the evaluation of the severity of pelvic organ prolapse and other PFD findings.
The radiologist’s report should include all the information that might be useful to surgeons, including the location and number of compartments affected. Our reporting template is made up of two main sections, including the results from Static sequences and the Dynamic ones.
|
Grading Prolapses with the PCL
|
cm
|
|
Grade
|
Distance from PCL
|
|
Mild
|
1-3 below PCL
|
|
Moderate
|
3-6 below PCL
|
|
Severe
|
>6 below PCL
|
| |
|
|
|
Grading of Pelvic Floor Relaxation with H and M Lines
|
|
Grade
|
Hiatal Enlargement (H, cm)
|
Pelvic Floor Descent (M line)- Rectocele severity (cm)
|
|
Normal
|
<6
|
<2
|
|
Mild
|
6-8
|
2-4
|
|
Moderate
|
8-10
|
4-6
|
|
Severe
|
>10
|
>6
|