Study Design
An experimental study was conducted at the Imaging Department of a public, university and general hospital (not exclusively pediatric). It was developed in 3 main steps (Figure 1):
0. Current Practice (assessment)
1. Optimization Tests
2. Quality Evaluation
3. Clinical Application.
This research got the appropriate authorizations from the Ethical Board of the hosting hospital. There was no conflict of interest in this study.
Radiological Equipment and Quality Assurance
The equipment used to perform the tests was Philips Digital Diagnost, which has a Pixium 4600 (43 cm x 43 cm) detector consisting of caesium iodide and amorphous selenium with a matrix of 3,000 x 3,000 pixels. The pixel size is 143 µm and the greyscale depth is 14bit. This system features a 2.5mm Al permanent filtration, an anti-scatter grid (grid index 12:1) and three focal points: 0.6, 0.9 and 1.2mm. The Automatic Exposure Control (AEC) is realized through 3 exposure cameras. The estimation of the Air Kerma-Area Product (KAP) is made electronically.
Although the radiological equipment used in this study is covered by a quality control program, some tests were performed before starting the optimization tests, namely (Figure 2): measurement of peak tube potential, exposure time, total filtration and light alignment with the exposure field (4).
Phantoms
The anthropomorphic phantoms used were:
- CIRS ATOM® 705 - anthropomorphic phantom specific for dosimetric research that simulates a 5-year-old child with a height of 110 cm, a weight of 19 kg and a chest with dimensions 14x17cm (Figure 3)
- KYOTO KAGAKU® PBU-60 - Full-length phantom with a life-size skeleton with a length of 165 cm and a weight of 50 kg (Figure 4).
1. Optimisation Tests
For both phantoms, several exposures were performed which were intended to test several combinations of exposure parameters, namely tube potential (kV), tube current (mAs), use of AEC, additional filtration and anti-scatter grid. For each exposure, data were collected: resulting mAs (when using AEC), KAP and exposure time.
2. Image Quality Assessment
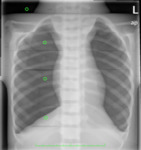
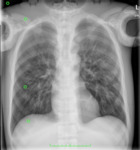
For each resulting image, the Signal to Noise Ratio (SNR) was calculated using the RadiAnt DICOM Viewer® software. Four Regions of Interest (ROI) were marked for each image: image background, pulmonary parenchyma (below the 7th rib), bone (1/3 external of the clavicle) and soft tissue (diaphragm). In the images obtained with the CIRS ATOM® 705 phantom, the ROIs have an area of 0.13 cm2 containing 682 pixels (Figure 5). For images obtained with the KYOTO KAGAKU PBU-60 phantom, the ROI area is 0.31 cm2 and the number of pixels contained in this same area is 1 589 (Figure 6).
SNR was calculated using the method described in Bourne according to the following equation (5):
SNR = (μ/σ) * 0,66
Where μ is the average signal value of the 4 ROI's and σ is the standard deviation of the background ROI.
A subjective evaluation was also performed in which 3 observers (1 Radiologist and 2 Radiographers) evaluated all images according to anatomical criteria and perception of physical characteristics (eg noise), using the ViewDex® software. The evaluation scale used classifies the degree of confidence of observers regarding the fulfilment of each criterion, in a 5-item scale for the anatomical criteria: 1 - Confident that the criterion is not met; 2 - A little confident that the criterion is not met; 3 - Undecided if the criterion is met or not; 4 - A little confident that the criterion is met; 5 - Confident that the criterion is met (6-8). For the physical characteristics of the image, the rating scale is 3 items: 1 - Unacceptable; 2 - Acceptable; 3 - Great (Figure 7).
3. Clinical Application
In this study, the population consisted of pediatric patients (0-18 years) from the Imaging Department who underwent AP/PA chest radiography during the data collection period. The sampling process was non-probabilistic, adopting a convenience sample, and all consecutive users who met the following inclusion criteria were recruited: being in pediatric age (0-18 years); perform the examination in the Philips Digital Diagnost room and with the digital detector Pixium 4600. The categorization of users was performed taking into account the guidelines of the document Radiation Protection No. 185 (9).
Several variables were collected regarding the patient and the radiographic examination: age, weight and height of the patient; projection of the exam; tube potential, tube current, exposure time, use of automatic exposure control, use of an anti-scatter grid, focus-detector distance and KAP.