Diagnostic criteria and imaging techniques for HCC
In this educational review we compare four International guidelines/systems for HCC diagnosis in cirrhotic liver:
a. European Association for the Study of the Liver (EASL);
b. Liver Imaging Reporting and Data System (LI-RADS)/ American Association for the Study of Liver disease;
c. Organ Procurement and Transplant Network (OPTN)*;
d. Asian Pacific Association for the Study of the Liver (APASL).
EASL, LI-RADS and APASL underline the importance of dynamic MRI versus CT imaging in patient at risk (MRI has a sensitivity up to 88% and specificity up to 94%)5. In addition to the evaluation of vascular enhancement of lesions, MRI allows to identify lesion content including fat, hemorrhage, and iron.
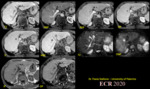
Imaging protocol includes unenhanced fast spin echo sequences with short and long echo times (T1 and T2 weighted images), in-phase and opposed phase T1 weighted gradient echo images (useful for the evaluation of fat within lesions) and fat suppression with T2 W fast spin echo sequences (Fig.1).
T1 weighted imaging is performed with breath hold spoiled gradient echo (SGE) technique. T2 weighted imaging is most frequently performed as echo train spin echo (FSE or TSE). Short tau inversion recovery (STIR) may also be used as a T2 weighted sequence and this can be modified to turbo STIR to save time6.
Suggested or optional images according to LI-RADS are DWI, subtraction imaging after contrast, and multiplanar acquisition. Subtraction imaging is useful whenever there are lesions that are spontaneously hyperintense on T1-weighted sequence, but it requires a reproducible breath-holding technique for satisfactory series co-registration.
MRI contrast agents for hepatic imaging are distinguished in two main groups: extracellular and hepatobiliary agents.
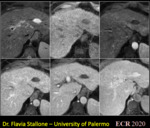
Extracellular agents tend to spread to the interstitial compartment after the vascular phases (Fig. 2) and are excreted trough glomerular filtrate in an unchanged state with an half life of approximately 1.5 h7.
Hepatobiliary agents (Gadobenate Dimeglumine, Gd-BOPTA and gadoxetate disodium, Gd-EOB-DTPA) have a distribution in the interstitial compartment and an hepatocyte uptake with subsequent biliary excretion in later phases. Gd-BOPTA has an hepatobiliary uptake of around 3% with a consequent hepatobiliary phase around 90 to 120 minutes after the contrast injection.
Gd-EOB DTPA instead has an uptake up to 50% with a much earlier hepatobiliary phase around 20 minutes after contrast injection8. However, Gd-EOB-DTPA looses the ability to evaluate the pure vascular on 3-minute phase because of the very fast hepatocyte uptake.
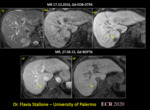
Regardless of the contrast agent, the following phases are always acquired after intravenous contrast agent injection: a “late arterial phase” which is critical for detection of HCC; “portal venous” phase and “delayed” or “equilibrium” or “3-minute” phase obtained typically 3 minutes after contrast agent injection9. Gd-BOPTA and Gd-EOB-DTPA allow also to acquire an hepatobiliary phase at 90-120 minutes and 20 minutes, respectively. Hepatobiliary phase can be used to increase the sensitivity of HCC detection of small lesions, suggest the diagnosis of HCC in lesions without washout or without arterial hyperenhancement (Fig. 3)10.