Fig. 2
References: Sapienza University of Rome

Fig. 3
References: Sapienza University of Rome

Fig. 4
References: Sapienza University of Rome
On suspicion of active bleeding, it is necessary to perform a multi-phase acquisition protocol with:
-Non-contrast scan
-Arterial phase (30-35 '' from the CA injection) to detect the vessel/s that is/are supplying the bleeding
-Venous phase
-Late phase (4-5 'from the injection)
A rapid injection of contrast agent (5 mL/sec) is necessary to achieve an optimal arterial enhancement (250 to 300 HU). This enhancement makes possible the discrimination of intravascular contrast from aortic calcification and thrombus.
Normal appearance of post-surgical changes
During the days following cardiac surgery, the surgery site and the adjacent areas are common locations in which can be frequently detected small blood or serum collections.
Also mediastinal, pleural or pericardial effusion containing air bubbles are frequently founded [5].

Fig. 6
References: Sapienza University of Rome

Fig. 5
References: Sapienza University of Rome
Another frequent site of inflammatory tissue thickening, is the retrosternal space, that commonly shows a variable amount of fluid and/or hematic material in its context.
After closure, the sternotomic access can show different aspects:
- a small gap (maximum diameter of 4 mm)
- a step
- an overlap of the sternal stumps,
- small hematomas and fluid material with air bubbles, between the sternal stumps
All of these findings tend to resolve within 2 weeks [5,9].
On the other side the complete welding of the sternotomy takes place at 6 months (about half of the patients) or at most within 1 year of the operation.

Fig. 8
References: Sapienza University of Rome
Pericardial effusion/cardiac tamponade
The evidence of pericardial effusion is a frequent finding in the first days after cardiac surgery (up to 85% of cases) and usually it has no clinical relevance [10].
Hemopericardium is a dangerous complication, especially in patients with coagulation deficiency. It can be the consequence of a iatrogenic wall trauma, ventricular wall rupture secondary to myocardial infarction, the dehiscence of a suture or persistent bleeding from pericardial vessels [10].
A rare and deadly complication is cardiac tamponade. When it occurs within the first 2 hours after the procedure, it requires re-intervention [11,12].

Fig. 9
References: Sapienza University of Rome
Sternal complications
The most typical sternal complications are sternal dehiscence, diastasis and osteomyelitis.
They usually have a chronic course, but, sometimes, they could cause acute or subacute clinical manifestations.
The complete welding of the sternotomy takes place in 6 months in about 50% of the patients or, at most, in 1 year after the operation.

Fig. 11
References: Sapienza University of Rome

Fig. 12
References: Sapienza University of Rome
Mediastinal hematoma
In CT, mediastinal hematoma appears as a retrosternal fluid collection with high attenuation values, which is often accompanied by fluid-fluid levels with a relatively hyperdense component in the bottom[13].

Fig. 14
References: Sapienza University of Rome
Acute mediastinitis

Fig. 13
References: Sapienza University of Rome
Diabetes mellitus, peripheral vascular diseases, COPD and prolonged hospitalization considerably increase the risk to develop mediastinitis. BMI>30 double the risk [5].
Constrictive pericarditis
Often caused by a chronic inflammatory of pericardial layers, that become rigid and non-stretchable. It leads to severe diastolic dysfunction and ventricular failure [33,35].
It generally occurs lately after the inflammatory event, but it can also onset as a subacute condition.
CT can show typical findings such as the thickening of the pericardial layers (thickness> 4mm), often with calcifications. Enlargement of the atrial chambers, the superior and inferior vena cava, and compression of the ventricles are typical findings.
MRI may reveal active persistent inflammation of the pericardium with high signal in T2-weighted sequences and enhancement after CA and it can be discriminating in the differential diagnosis with other cardiac diseases (e.g. restrictive cardiomyopathies) [12,15,16].
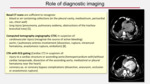
Complications after coronary artery bypass surgery
Graft stenosis or occlusion are the most common early complications in patients undergoing CABG and venous grafts are the most involved.
CTA should be performed when clinical and laboratory signs are equivocal, in cases of technical obstacles to select graft during angiography or to find adequate endovascular access.
The graft occlusion can be acute (CTA shows thrombus inside the graft or a dilated graft) or chronic (collapsed or "missing" vessel segments).

Fig. 17
References: Sapienza University of Rome

Fig. 15
References: Sapienza University of Rome
The CTA is also the reference method to accurately locate a coronary psuedoaneurysm, recognizable as an organized hematoma near a break point of the bypass, contained by a reaction of the adjacent connective tissues and often a narrow neck (more common in the first six months after surgery) [19].
Aneurysmal modification of the vascular graft is an uncommon complication (<1% are aneurysms of the great saphenous vein), consequent to the atherosclerotic degeneration of the graft.
Surgical correction is necessary when the dilation of the graft exceeds 2 cm, due to the risk of potentially catastrophic complications such as thrombosis, fistula formation and vessel rupture. The bypass aneurysm typically occurs more than 5 years after surgery and occurs in the body of the graft itself [20].
Complications after valve surgery
The malfunction of a prosthetic valve often has an insidious clinical presentation and the evaluation by transthoracic (TT) or transesophageal (TE) echocardiography may be difficult.
In those case CT with retrospective ECG gating, with a complete reconstruction of the whole cardiac cycle (a dataset every 10% of RR interval) may be very helpful!
COMPLICATIONS AFTER VALVE SURGERY
CT can detect:
•Valvular or paravalvular leakage
•Dehiscence of suture or anastomosis
•Valvular vegetations (endocarditis and abscess)
•Prosthesis obstruction
•Prosthesis rupture
•Aortic dissection
The mere assessment of the valve prosthesis motion with CT does not require the use of the contrast agent, given the high density of the metal component of the prosthesis [5.21].
A deadly (mortality rates 30-70%) and relatively frequent complication (incidence 1-6%) in these patients is the endocarditis of the prosthetic valve (PVE). The risk is maximum in the first 2 months after the intervention and remains high during the first year [22].
As with native valves, the typical lesion is the presence of a vegetation along the suture line that extends to the annulus and peri-annular tissue, leading to possible later formation of paravalvular abscesses or fistulas, dehiscence of the prosthesis or even obstruction of the prosthesis.
Transoesophageal echocardiography (TEE) is traditionally the first investigation for the study of native valves and PVE, and for the associated complications.
CTA seems to be an equivalent or potentially superior technique also showing less metal artefacts compared to TEE in the detection of valvular vegetations [22].
The vegetations can be recognized as irregular-shaped, hypodense and not-enhancing masses, attached to the edges of the prosthesis.
The abscesses appear as irregular and uneven paravalvular masses within the perianular region, with thick walls that enhance after CA [8].
Pseudoaneurysms appear as small paravalvular or perivascular outpouching. Their content has the same density as the circulating blood and it enhances after administration of contrast agent, communicating with the lumen of the heart chambers or with the lumen of the aortic root (Figure 2) [8].

Fig. 18
References: Sapienza University of Rome
Complications of aortic root and ascending aorta surgery
CTA represents the reference examination for the diagnosis of aortic dissection, intramural hematoma (blood collection in the aortic wall) and penetrating ulcer of the aorta following surgery [23].

Fig. 19
References: Sapienza University of Rome
In CT imaging, anastomotic dehiscence appears like a pseudoaneurysm and requires urgent treatment with suspension of anticoagulant therapy and / or angiographic closure of the leakage or reoperation for replacement with a new graft when possible [8].
CTA has high specificity and sensitivity (95-98%) in the diagnosis of aortic dissection, with very rapid execution that make it the first-choice examination for this clinical suspicion [24].
Correct knowledge of the surgical procedure performed is essential to correctly interpret the images and not to risk a misinterpretation of the hyperdense prosthetic walls in basal scans with the intramural hematomas or bleedings [23].
The acute angulation of the graft (kinking) can also simulate a focal dissection: the use of 3D-MPR may clarify the anatomy in these cases.
After the ascending aorta replacement, the CT low-density "peri-prosthetic" fluid collections represent the results of the physiological liquefaction of the hematoma; after reabsorption of this collection, fibrosis or granulation tissue may be present, even for a few months [23].

Fig. 20
References: Sapienza University of Rome
The graft infection often leads to the dehiscence of the anastomosis!
Complications after trans-catheter valve implantation (TAVI)
The implantation of aortic valve prosthesis by percutaneous transcatheter or by transapical thoracotomy is an emergent treatment for severe aortic valve stenosis in selected patients, especially in elderly population (over seventy and eighty) and high cardiac surgery risk (operative mortality >15%), or in patients with degeneration of previously implanted biological aortic valve.
The most common complications are bleeding, migration, mispositioning or thrombosis of the device [26]. CT imaging is the modality of choice to confirm suspected complication at echocardiography or to obtain a comprehensive assessment in candidate for re-intervention.
Mispositioning of the endoprosthesis is usually due to nodular calcifications at the level of the aortic valve annulus or wrong measurement in pre-procedural planning, that can cause an irregular distension of the device, with diastolic regurgitation [26].
TAVI carries an increased risk of coronary thrombosis (myocardial infarction, stroke, embolism) that we can diagnose through a Cardiac CT.